Autism
Topic: Medicine
 From HandWiki - Reading time: 64 min
From HandWiki - Reading time: 64 min
Autism, also known as autism spectrum disorder (ASD),[lower-alpha 1] is a condition characterized by differences or difficulties in social communication and interaction, a need or strong preference for predictability and routine, sensory processing differences, focused interests, or repetitive behaviors.[1] Features of autism are present from early childhood and the condition typically persists throughout life.[2][3] Autism is classified as a neurodevelopmental disorder,[4] and a formal diagnosis requires professional assessment that these characteristics cause significant challenges in daily life beyond what is expected given a person's age and social environment.[5][6][7][8] Because autism is a spectrum disorder, presentations vary and support needs range from minimal to the person being non-speaking or needing 24-hour care.[9][5][6][10]
Autism diagnoses have risen since the 1990s, largely because of broader diagnostic criteria, greater awareness, and wider access to assessment.[11] Changing social demands may also play a role.[12][13] The World Health Organization estimates that about 1 in 100 children were diagnosed between 2012 and 2021, noting an increasing trend.[lower-alpha 2][11][14] Surveillance studies suggest a similar share of the adult population would meet diagnostic criteria if formally assessed.[15] Autism is highly heritable and involves many genes, while environmental factors appear to play a smaller, mainly prenatal role.[16][17][18][19] Boys are diagnosed several times more often than girls, with girls being better at hiding autistic traits.[20][11][21] Conditions such as anxiety, depression, attention deficit hyperactivity disorder (ADHD), epilepsy, as well as intellectual disability, are more common among autistic people.[22][23][24] Certain savant abilities are also more common in autistic people than in other groups.[25]
There is no cure for autism.[26] Several autism therapies aim to improve self-care, social, and language skills.[27] Reducing environmental and social barriers helps autistic people participate more fully in education, employment, and other aspects of life.[28][29][30] No medication addresses the core features of autism, but some are used to help manage commonly co-occurring conditions, such as anxiety, depression, irritability, ADHD, and epilepsy.[31][32]
The idea of autism as a disorder has been challenged by the neurodiversity framework, which frames autistic traits as a healthy variation of the human condition.[33] This perspective, promoted by the autism rights movement, has attracted increasing research attention,[34] but is debated and remains controversial among autistic people, advocacy groups, healthcare providers, and charities.[35][36]
Signs and characteristics
Autism is primarily characterized by differences and difficulties in social interaction and communication, alongside restricted or repetitive patterns of interests, activities, or behaviors (stimming), and, in many cases, distinctive reactions to sensory input. The specific presentation varies widely.[37][38] Clinicians often consider assessment for autism when these characteristics are present, especially if they are associated with difficulty obtaining or sustaining employment or education, difficulty initiating or maintaining social relationships, involvement with mental health or learning disability services, or a history of neurodevelopmental conditions (including learning disabilities and ADHD) or mental health conditions.[39][40] In most cases, signs of autism are first observable in infancy or early childhood and remain throughout life.[41] Autistic people may be significantly disabled in some respects, but average—or, in some cases, superior—in others.[42][43][44]
Social and communication skills
Autistic people may have differences in social communication and interaction, which can lead to challenges in environments structured around non-autistic norms. Diagnostic criteria for autism require difficulties across three social domains: social-emotional reciprocity, nonverbal communication, and developing and maintaining relationships.[45]
Social–emotional reciprocity
Common early signs of autism include little or no babbling in infancy.[37] Difficulties may also be apparent in traditional forms of reciprocal social interaction, such as games like peek-a-boo[37] or pat-a-cake,[46] as well as in shared attention to objects of interest;[37] this may distinguish autistic from non-autistic infants.[47]
Historically, autistic children were said to be delayed in developing a theory of mind, and the empathizing–systemizing theory proposed that while autistic people may have compassion (affective empathy) for others with similar autistic traits, they often have limited, though not necessarily absent, cognitive empathy.[48] This may present as social naïvety,[49] lower-than-average intuitive perception of the meaning or utility of body language, social reciprocity,[50] or social expectations, including the habitus, social cues, and certain aspects of sarcasm,[51] which to some degree may be influenced by co-occurring alexithymia.[52]
Recent research has increasingly questioned these earlier interpretations,[53] as the double empathy problem theory (2012) proposes that misunderstandings arise mutually between autistic and non-autistic people, rather than solely from autistic deficits in empathy or social cognition.[54][55][56] This perspective has contributed to a growing recognition that autistic behavior and communication may reflect different, rather than deficient, social behavior and communication styles.[53][55][56] Autistic interests and conversational styles are often characterized by a strong focus on specific topics, a phenomenon known as monotropism.[57][58]
Spoken communication
Differences in verbal communication often become noticeable in early childhood, as many autistic children develop language skills at an uneven pace. Speech may emerge later than is typical or not at all (non-speaking autism), while reading ability may be present before school age (hyperlexia).[59] Infants may show delayed onset of babbling, atypical gestures, lower responsiveness, or vocal patterns that are less synchronized with caregivers. During the second and third years, autistic children may produce less frequent and less varied babbling, consonants, words, and word combinations, and may integrate gestures with speech less often. They are less likely to make requests or share experiences, and more likely to repeat others' words or phrases (echolalia).[60] About 25–35% of autistic school-age children are non-speaking or minimally speaking.[61] The age at which speech develops and the complexity of early language development are significant predictors of verbal communication abilities in later life.[61]
Nonverbal communication
Autistic people often display atypical behaviors or differences in nonverbal communication. Some may make infrequent eye contact, even when called by name, or avoid it altogether because they find it uncomfortable, distracting, or overstimulating.[62] They may recognize fewer emotions or interpret facial expressions differently, and may not respond with expressions expected by their non-autistic peers.[63][59] They can also have difficulty inferring social context or subtext in conversation or text, resulting in different interpretations of meaning.[64] Speech characteristics such as volume, rhythm, and intonation (prosody) can vary,[65] and atypical prosody is estimated to occur in at least half of autistic children.[65]
Developing and sustaining relationships
Signs of autism in childhood include less apparent interest in other children or caregivers, possibly with more interest in objects.[37] Behaviors that may appear as indifference to non-autistic people often reflect autistic differences in recognizing others' personalities, perspectives, and interests.[64] Most research has focused on interpersonal relationship difficulties between autistic and non-autistic people and on teaching social skills to address these gaps; however, newer studies indicate that autistic people often form satisfying relationships with other autistic people, which can enhance quality of life.[66]
Children on the autism spectrum are more likely than their non-autistic peers to be involved in bullying, most often as victims.[67] Among autistic people who seek friendships, reduced friendship quality and quantity are often associated with increased loneliness.[68] Autistic people also face greater challenges in developing romantic relationships than non-autistic people.[69]
Over time, many autistic people learn to observe and form models of social patterns, and develop coping strategies, such as "masking".[70] Masking is associated with poorer mental health outcomes as well as delayed diagnosis, which can limit access to appropriate supports.[70]
Restricted and repetitive behaviors

The second core feature of autism is a pattern of restricted and repetitive behaviors, activities, and interests. To be diagnosed with autism under the DSM-5-TR, a person must exhibit at least two of the following behaviors:[45][71]

- Repetitive behaviors: actions such as rocking, hand flapping, finger flicking, head banging, or repeating phrases or sounds (including echolalia[46]).[72] These behaviors may occur consistently or primarily when the person is stressed, anxious, or upset. They are also known as stimming. Other examples include playing with toys in ways others might consider limited or unusual[37] (e.g., arranging toys in a row[46]).
- Resistance to change: a strong preference for routine, such as performing daily tasks in a specific order or showing distress in response to changes others may consider minor.[73] The person may become distressed if their routine changes or is disrupted.[73]
- Focused interests: intense interest in a particular activity, topic, or hobby, often accompanied by sustained attention and deep knowledge; for example, a strong attachment to certain objects[45] or frequent discussion of a specific topic.[74]
- Sensory reactivity: atypical responses to certain sensory inputs, such as aversion to specific sounds or textures, fascination with lights or movement, or apparent indifference to pain or temperature.[75]
It is increasingly argued that these characteristics should be accepted, which is supported by their recognized functions, such as self-regulation.[76] Focused interests can also provide personal fulfillment and contribute to the development of specialized knowledge.[74] A distinction should be made between these features and those of obsessive–compulsive disorder, which can co-occur with autism and involve compulsions or obsessions aimed at preventing feared outcomes.[77]
Self-injury
Self-harm occurs about three times more often in autistic people than in non-autistic people.[78] Behaviors can include head-banging, hand-biting, and skin-picking, and can lead to serious injury or, in rare cases, death.[79] Several explanations have been proposed for why self-harm develops and persists among people with developmental conditions such as autism.[80] Communication difficulties may lead some autistic people to use self-injury to express needs, distress, or other messages.[79] Self-harm may also help regulate sensory input[81] or modulate pain perception, particularly for those experiencing chronic discomfort or medical conditions.[80] Neurological factors are also under investigation, with atypical basal ganglia connectivity suggested as a potential biological predisposition in some autistic people.[80]
Wandering (elopement)
Some autistic people "wander" off—a behavior known as elopement—and place themselves in danger. About half of families with autistic children report elopement.[82] The propensity for elopement increases with the severity of the autism.[82] Siblings unaffected by autism show much lower rates of elopement.[82] Drowning, a leading cause of death for autistic children,[83] and traffic injuries are among the dangers associated with elopement.[82]
Fatigue, burnout, inertia, meltdown, shutdown
Several non-diagnostic models have been used to describe challenges that autistic people face in their daily lives.[84] These concepts lack formal clinical criteria, but are widely described by autistic people themselves.[84][85]
Autistic fatigue or burnout is a prolonged state of mental and physical exhaustion.[86][85][84][87] It is described as distinct from, but similar to, occupational burnout, and is often linked to the pressure to camouflage or mask autistic traits in social interactions.[85][86] The term "autistic burnout" was first used in 2008, with research into the phenomenon undertaken in the 2020s.[86] Several researchers have proposed various characterizations of autistic burnout, but no consensus definition exists. Depression can be misattributed to autistic burnout, as they have several overlapping criteria. Reported coping strategies include reduced masking, increased stimming, engaging in special interests and familiar activities, and seeking stress relief. Some affected people temporarily withdraw from social contact as a recovery strategy; while providing relief, interpersonal withdrawal can also result in loneliness and worsening mental health. There is limited data on professional interventions.[86]
Autistic inertia is a difficulty experienced among autistic people with initiating, transitioning between, or stopping activities or mental states.[85] It may manifest as a feeling of being "stuck", where people find it challenging to begin a task, shift focus to a different activity, or disengage from an action, even when they want to.[84]
A meltdown may occur if, upon processing large amounts of information, an autistic person experiences anxiety or feels overwhelmed.[88] Triggers may be sensory or social, and often include unpredictability, unmet basic needs, and emotional situations, which tend to accumulate.[88] A meltdown can be expressed audibly (e.g., screaming or crying) or physically.[88] The person often shows signs of distress beforehand, such as pacing, asking repetitive questions, trembling, or sweating.[88] An autistic shutdown is similar, but inward, and the autistic person is often unable to speak or withdraws completely.[88] Meltdowns or shutdowns may be prevented by eliminating the distressing factors.[88] They may be ameliorated by avoiding further questions or pressure, showing the person that one is there to help, and allowing the person to calm down by leaving the situation or breathing slowly.[88]
Cognitive profile
Autistic people often show an uneven or "spiky" cognitive profile, with relative strengths in some cognitive domains alongside difficulties in others.[89] The otherwise rare savant syndrome, characterized by an isolated skill in a narrow area, is more common among autistic people, but studies of its prevalence have found different results. These special skills are related to prodigious memory. Most common are splinter skills, such as memorization of sports trivia or historical facts.[90][91] Research has also reported enhanced performance by autistic participants on certain perceptual and attentional tasks.[92]
Other features
Autistic people may exhibit traits or characteristics that are not part of the formal diagnostic criteria but can nonetheless affect their personal well-being or family dynamics.[93]
- An estimated 60–80% of autistic people have motor signs that include poor muscle tone, poor motor planning, and toe walking;[94][95] difficulties in motor coordination appear common across the autism spectrum.[96][97]
- Unusual or atypical eating behavior occurs in about 70% of children on the autism spectrum,[98] to the extent that it was once considered a diagnostic indicator.[93] Selectivity is the most common characteristic, although eating rituals and food refusal are also reported.[98]
- Several studies report moderate correlations between autism, Internet addiction disorder, and video game addiction.[99]
Causes
The exact causes of autism are unknown,[100][101][102][103] with genetics likely being the largest contributing factor. It was long presumed a single cause at the genetic, cognitive, and neural levels underpinned the social and non-social features,[104] but autism is increasingly thought to be a complex condition with distinct, often co-occurring, causes for its core aspects.[104][105] It is unlikely that autism has a single cause;[105] research has identified many factors as potential contributors,[106] including genetics,[71] prenatal and perinatal (shortly after birth) history,[106] neuroanatomical anomalies, changing social demands in the workplace or in school,[12] and environmental influences.[106] It is possible to identify general factors but difficult to determine specific ones.[107] Research into causes is complex due to challenges in identifying distinct biological subgroups in the autistic population.[108]
Genetics
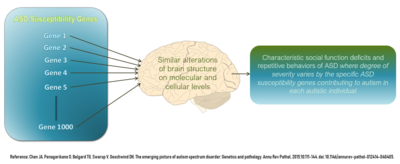
Autism has a strong genetic basis, but the genetics of autism are complex and it is unclear whether autism is explained more by rare mutations with major effects or by rare multi-gene interactions of common genetic variants.[109][110] Twin studies indicate that autism is highly heritable, with genetic factors explaining most of the risk and shared environmental effects playing a minor role.[16] Numerous genes have been found to be associated with autism, with most loci individually explaining less than 1% of autism cases[111] and having only small effects.[109] While these genetic variants are associated with a higher likelihood of being autistic, they do not individually determine whether someone will be autistic.[112] Complexity arises from interactions among multiple genes, the environment, and heritable epigenetic factors (which influence gene expression without changing DNA sequence).[113]
Typically, autism is not traceable to a single-gene (Mendelian) mutation or chromosome anomaly, and no known genetic syndrome selectively causes autism.[109] If autism is one characteristic of a broader medical condition, such as fragile X syndrome, it is called syndromic autism, as opposed to non-syndromic or idiopathic autism, which is typically polygenic without a known cause.[114] Syndromic autism is present in approximately 25% of autistic people.[115] Research has suggested that autistic people with intellectual disability tend to have rarer, more impactful, genetic mutations than those found in people diagnosed solely with autism.[116] A number of genetic syndromes causing intellectual disability may also co-occur with autism, including fragile X, Down, Prader–Willi, Angelman, Williams syndrome,[117] and SYNGAP1-related intellectual disability.[118]
Research suggests that autism is associated with genes that influence neural development and connectivity. These are involved in key neuronal processes such as protein synthesis, synaptic activity, cell adhesion, and the formation and remodeling of synapses, as well as the regulation of excitatory and inhibitory neurotransmission. Studies have identified lower expression of genes linked to the inhibitory neurotransmitter gamma-aminobutyric acid, alongside higher expression of genes associated with glial (e.g., astrocytes) and immune (e.g., microglia) cells, correlating with higher numbers of these cells in post-mortem brain tissue. Genes associated with variation in the mTOR signaling pathway, which is involved in cell growth and survival, are also under investigation.[119] Some hypotheses in evolutionary psychiatry suggest that autism-associated genes may persist because of proposed links to traits such as intelligence, systematizing abilities, or innovation.[120]
If parents have one autistic child, the chance of having a second autistic child ranges from 7% to 20%.[71] Though autism is highly heritable, many autistic people have only non-autistic family members. In some cases, this may be explained by de novo structural variations—such as deletions, duplications, or inversions—that arise spontaneously during meiosis and are not present in the parents' genomes.[121][122] The likelihood of being autistic is greater with older fathers than with older mothers; two potential explanations are the known increase in the number of mutations in older sperm and the hypothesis that men marry later if they carry a genetic predisposition and show some signs of autism.[123]
Evolutionary perspectives
Research on the evolutionary advantages of autism and associated genes has suggested that autistic people may have contributed uniquely to human development, particularly in technological innovation (such as tool-making) and in detailed observation and analysis of the natural environment.[124] Systematic reviews emphasize that these ideas remain speculative and that no single evolutionary explanation has been established.[125]
Social factors
Social factors such as upbringing are not known to cause autism, but it is possible that increasing demands for flexibility and social interaction in education, or in one's personal and professional life, may cause people to exhibit pronounced difficulties that would not have led to diagnosis in a different setting.[12][13]
Neurocognitive theories
Various theoretical frameworks attempt to integrate underlying genetic and environmental causes with observed neurobiological findings and behavioral traits.
- The Intense World Theory proposes that a higher neural responsiveness in autism leads to more intense sensory perception, attention, memory, and emotional responses, shaping the person's experience.[126]
- The Enhanced Perceptual Functioning model of autism posits that superior and more independent functioning of auditory and visual perception is the root cause of the specific pattern of cognitive, behavioral, and neural performance observed in autistic people.[29] The model asserts the importance of perception, arguing it is more central to the autistic phenotype than social or higher-order cognitive processes.[29]
Beyond models of causation and brain function, cognitive theories have been developed to explain patterns of information processing common in autistic people, to better understand the autistic phenotype.[127] While these cognitive accounts describe how autistic traits may manifest, they are generally viewed as explanations of the behavioral and cognitive consequences of the underlying neurobiological development rather than primary causes themselves.[127]
- The weak central coherence theory suggests a tendency to focus on details over broader context.[127]
- The empathising–systemising theory posits that autistic people have distinct cognitive styles related to analyzing systems versus empathizing with others.[127]
Early life and prenatal or perinatal factors
Certain factors during pregnancy and birth may increase the likelihood of autism,[128] although no single factor is conclusive and study results are often inconsistent.[129] These factors include advanced parental age,[130][131] maternal health conditions (e.g., gestational diabetes, infections such as rubella,[132] inflammation[133]), exposure to certain medications (e.g., valproate[129]), and some environmental exposures like significant air pollution during pregnancy.[134] While many environmental factors have been investigated, few have established links,[129] and some prominent claims (e.g., vaccines or parenting styles) have been disproven.[135]
Disproven refrigerator mother hypothesis
Work on autism in the mid-20th century proposed the "frigid mother" or refrigerator mother hypothesis, according to which poor parenting or lack of emotional support from parents leads to autism.[136] When it was proposed, the hypothesis contributed to considerable media attention about autism, which had previously been mostly ignored.[137] The hypothesis has since fallen out of favor, and has not garnered support when studied.[136] But the blame placed on parents of children on the autism spectrum, especially mothers, has contributed to substantial stigma.[138][139]
Early social experiences, such as caregiver interactions or deprivation, may shape the development of autism, potentially via gene–environment correlations, and are distinct from the discredited refrigerator mother hypothesis.[19]
Disproven vaccines hypothesis
Parents may first become aware of autistic characteristics in their child around the time of a routine vaccination. This has led to theories – subsequently disproven – blaming vaccine "overload", the vaccine preservative thiomersal, or the MMR vaccine for causing autism.[140] In 1998, British physician Andrew Wakefield led a fraudulent, litigation-funded study that suggested that the MMR vaccine may cause autism.[141][142][143][144][145] His co-authors have since recanted the claims made in the study.[146] Wakefield was struck off the British medical register for "serious professional misconduct" after determination that his involvement in the study amounted to fraud, leading to the loss of his right to practice medicine.[147]
Two versions of the vaccine causation hypothesis were that autism results from brain damage caused by either the MMR vaccine itself,[148] or by mercury used as a vaccine preservative.[149] No convincing scientific evidence supports these claims.[148] They are biologically implausible,[140] and further evidence continues to refute them, including the observation that the rate of autism continues to climb despite elimination of thimerosal from most routine vaccines given to children from birth to 6 years of age.[149][150][151][152][153]
A 2014 meta-analysis examined ten major studies on autism and vaccines involving 1.25 million children worldwide; it concluded that neither the vaccine preservative thimerosal (mercury), nor the MMR vaccine, which has never contained thimerosal,[154] lead to autism.[155] Despite this, misplaced parental concern has led to lower rates of childhood immunizations, outbreaks of previously controlled childhood diseases in some countries, and the preventable deaths of several children.[156][157]
Anti-vaccine activists have spread false claims about the absence of autism in North America's Amish population due to lower vaccination rates. A 2010 study revealed that autism is present in 1 out of every 271 Amish children.[158][159][160][161]
Mechanism
Diagnosis
This section may not properly summarize its corresponding main article. (Learn how and when to remove this template message) |
Classification
The DSM-5 and ICD-11 are the two main frameworks for classification of mental disorders in use today. Autism spectrum disorder is classified in both as a neurodevelopmental disorder, with its definition encompassing a spectrum of highly varied presentations.[162][51] The spectrum concept signals diversity rather than a simple range from mild to severe.[163] Before the DSM-5 (2013) and ICD-11/ICD-11 CDDR (2019/2024),[162][164] autism fell within a broader pervasive developmental disorder category that included labels such as Asperger syndrome and classic autism (also called childhood autism or Kanner syndrome). Because these diagnoses overlapped, the manuals unified them under "autism spectrum disorder" (ASD).[165]
Since 1980, the committees behind both manuals have aimed for greater convergence, incorporating biological research while keeping behavior-based criteria.[166][167][168][169] ICD-11 instead records whether the person has co-occurring intellectual disability or language impairment.[170]
Some researchers have questioned whether existing criteria capture the full phenomenon, prompting proposals for prototype descriptions, transdiagnostic biological markers, or distinctions between common behavioral traits and rarer genetic or environmental factors.[171] Others have proposed alternatives to the disorder-focused spectrum model that deconstruct autism into separate phenomena: a non-pathological spectrum of behavioral traits in the general population,[172] and rare genetic mutations or environmental factors influencing neurodevelopmental and psychological conditions.[172]
DSM
The American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR), released in 2022, is the latest version.[173] Its fifth edition—DSM-5, released in 2013—was the first to define ASD as a single diagnosis,[174][175] combining the previously distinct diagnoses of classic autism, Asperger syndrome, childhood disintegrative disorder, and pervasive developmental disorder not otherwise specified (PDD-NOS).[175][176] This is still the case in the DSM-5-TR.[45][non-primary source needed]
The DSM-5 and DSM-5-TR adopt a dimensional approach, with one diagnostic category for disorders that fall under the autism spectrum umbrella. Within that category, the DSM-5 has a framework that differentiates individuals by dimensions of symptom severity and by associated features (i.e., the presence of other conditions or factors that may contribute to the symptoms, other neurodevelopmental or mental conditions, intellectual disability, or language impairment).[45] The two core symptom domains are (a) social communication and (b) restricted, repetitive behaviors. Clinicians may specify separate severity levels for each domain based on the degree to which symptoms affect daily functioning, rather than providing a single overall severity rating.[177]
Before the fifth edition, the DSM separated social deficits and communication deficits into two domains.[178] The DSM-5 also revised the onset criteria to specify that symptoms appear in the early developmental period, noting that symptoms may manifest later when social demands exceed capabilities; the previous edition had required onset before age three.[179] These revisions remain in the DSM-5-TR.[45]
ICD
The World Health Organization's International Classification of Diseases (11th revision), ICD-11, was released in 2018 and came into full effect in 2022.[180][166] Its classification of autism spectrum disorder (6A02) is based on whether or not intellectual impairment is present as well as the level, if any, of language impairment, as follows:[162]
| with mild or no impairment of functional language | with impaired functional language | with complete, or almost complete, absence of functional language | |
|---|---|---|---|
| without Disorder of Intellectual Development | 6A02.0 | 6A02.3 | |
| with Disorder of Intellectual Development | 6A02.1 | 6A02.4 | 6A02.5 |
Management
There is no cure for autism.[26] From the perspective of neurodiversity, "curing" or otherwise treating autism may not be an appropriate goal.[181][182]
Interventions targeting specific challenges or co-occurring conditions associated with autism are widely regarded as important.[183] Perspectives on the goals of these interventions vary: the medical model of disability often focuses on addressing core characteristics such as social communication difficulties and restricted/repetitive behaviors.[184] The neurodiversity movement supports interventions aimed at enhancing functional communication (spoken or non-spoken), managing related issues like anxiety or inertia, or addressing behaviors considered harmful, rather than seeking to alter core autistic features.[185][184]
Studies of interventions have methodological problems that prevent definitive conclusions about efficacy,[186] but the development of evidence-based interventions has advanced.[187] Several therapies can help autistic children,[188] and they are typically tailored to the child's needs.[189] The main goals of therapy are to lessen associated difficulties and family distress, and to increase quality of life and functional independence. In general, higher IQs correlate with higher responsiveness to interventions and larger intervention outcomes.[190][187] Behavioral, psychological, educational, and skill-building interventions may be used to help autistic people learn skills for living independently, as well as other social, communication, and language skills.[27] Therapy also aims to reduce behaviors perceived as inappropriate and to build upon strengths.[191] Medications have not been found to reduce autism's core features, but may be used for associated difficulties, such as irritability or inattention.[192]
Non-pharmacological interventions
Certain interventions, such as intensive, sustained special education, remedial education programs, and behavior therapy, are considered beneficial early in life for autistic children to acquire self-care, social, and job skills.[193] Available approaches include applied behavior analysis, developmental models, structured teaching, speech and language therapy, cognitive behavioral therapy,[194] social skills therapy, and occupational therapy.[189] These interventions may either target autistic features comprehensively or focus on a specific area of difficulty.[187]
Applied behavior analysis
This section may be too technical for most readers to understand. Please help improve it to make it understandable to non-experts, without removing the technical details. (August 2025) (Learn how and when to remove this template message) |

Applied behavior analysis (ABA) is a behavioral therapy that aims to teach autistic children certain social and other behaviors by prompting using rewards and reinforcement learning. This includes learning fine and gross motor and language skills through play, expressive labeling, and requesting. It also seeks to reduce aggressive and self-injurious behavior by assessing its environmental causes and reinforcing replacement behaviors. Early, intensive ABA therapy has demonstrated effectiveness in enhancing preschool children's language skills, adaptive functioning, and intellectual performance.[195][196][197][198] Another review reported a lack of adverse event monitoring, although such adverse effects may be common.[199]
Interventions for early childhood may be based on different theoretical frameworks, such as ABA (with its structured and naturalistic approaches) and Developmental Social Pragmatic (DSP) models.[187] Research indicates that in acquiring spoken language, autistic children with higher receptive language skills tend to make progress with fewer hours (2.5 to 20 per week) of a naturalistic approach, whereas those with lower receptive language skills tend to show more progress only with a greater intensity of intervention (25 hours per week) using discrete trial training, a structured form of ABA.[195][197]
ABA has faced criticism.[200][201][202] Sandoval-Norton et al. describe it as unethical and argue that it has unintended consequences, such as prompt dependency, susceptibility to psychological abuse, and overemphasis on compliance, which can create challenges in the transition to adulthood.[200] Increasingly, ABA is also criticized for trying to reduce or eliminate autistic behaviors to make children appear less autistic, rather than respecting neurodiversity.[203] A problem with unreported conflicts of interest in ABA research has been described, with potential effects on the quality of evidence.[204] In response, some ABA advocates suggest that instead of discontinuing the therapy, efforts should focus on increasing protections and ethical compliance.[205]
A related type of intervention is parent training models.[187] These teach parents to implement various ABA and DSP techniques themselves. Several parent-mediated behavioral therapies target social communication difficulties, while their effect on restricted and repetitive behaviors (RRBs) is uncertain.[206] Similarly, teacher-implemented interventions that combine naturalistic ABA with a developmental social pragmatic approach have been associated with effects on young children's social-communication behaviors, although there is limited evidence regarding effects on broader autistic characteristics.[187]
Inclusion in education and the workplace
Inclusive education models strive to support autistic students in mainstream educational settings, moving away from segregated special education environments toward participation alongside their peers.[207] Despite these efforts, autistic students can face significant barriers, sometimes leading to trauma or emotionally-based school non-attendance.[207][208] This avoidance is often rooted in overwhelming sensory environments, social anxieties, communication breakdowns, bullying, or lack of adequate support and understanding, rather than defiance.[207][208]
Central to successful inclusion is the application of frameworks like Universal Design for Learning (UDL), which proactively designs curricula and learning environments to be accessible and engaging for all students, including those who are autistic.[209] UDL principles accommodate varied learning styles, sensory sensitivities, and communication preferences often present in autistic people.[209]
The SPACE framework (sensory, predictability, acceptance, communication, empathy) developed by Doherty et al. primarily for healthcare settings offers a lens for identifying and addressing common environmental barriers that can contribute to distress and avoidance behaviors for autistic people.[28] Accommodations may include providing quiet spaces as a retreat for people feeling overwhelmed.[210] Autistic students may also need help initiating and maintaining social relationships with their peers if they wish to do so.[207] Especially in higher education, some autistic students may need help with executive functioning, e.g., managing their own work, and the ability to initiate and complete tasks.[211]
Transitioning to adulthood, autistic people often encounter substantial barriers to securing and maintaining meaningful employment, leading to high rates of unemployment and underemployment compared to the general population.[30] Challenges can include navigating traditional interview processes,[212] difficulties with unspoken social rules in the workplace, sensory sensitivities to office environments (e.g., lighting, noise), and needs for clear, direct communication and structured tasks.[30][213] Effective workplace inclusion involves implementing reasonable adjustments such as flexible working hours or locations, providing noise-canceling headphones, staff training, and mentorship programs.[30][213] Working from home can help to avoid overwhelming sensory or social situations, even if this means losing desirable social contact.[214][215] Autism-friendly workplaces not only allow autistic employees to utilize their unique skills and perspectives but also benefit employers through increased innovation, problem-solving capabilities, and employee loyalty.[213][216]
Pharmacological interventions
Autistic people may be prescribed medication to manage specific co-occurring conditions or behaviors, such as ADHD, anxiety, aggression, or self-injurious behaviors, particularly when non-pharmacological interventions alone have been insufficient.[217][218] Medications are not routinely recommended for autism's core features, such as social and communication difficulties or restricted and repetitive behaviors.[219]
More than half of autistic children in the United States are prescribed psychoactive drugs or anticonvulsants.[220] Commonly used drug classes include antidepressants, stimulants, and antipsychotics.[220] Among antipsychotics, risperidone and aripiprazole are the only medications approved by the U.S. Food and Drug Administration specifically for reducing irritability, aggression, and self-injurious behaviors in autistic people.[192][221] These drugs can have significant side effects and responses to them may vary.[192] The UK's National Health Service cautions against the overprescription of antipsychotics and recommends their use only for specific indications, at the lowest effective dose and for the shortest duration necessary.[222]
Some research suggests that risperidone and aripiprazole may also reduce restricted and repetitive behaviors, such as hand-flapping or body-rocking.[219] The evidence supporting this use has limitations, including study size and scope, alongside concerns about adverse effects.[223] A meta-analysis found no significant efficacy of these antipsychotics or SSRI antidepressants in reducing these behaviors.[224] Stimulant medications like methylphenidate may reduce inattention or hyperactivity in some autistic children, particularly when ADHD is also present.[189] But methylphenidate's efficacy is lower in autistic people with ADHD compared to non-autistic people with ADHD, and side effects are more common.[225]
Alternative medicine
Alternative therapies have been researched and implemented, and many have resulted in harm to autistic people.[189] For example, chelation therapy is not recommended as a treatment for autism, with risks outweighing potential benefits.[226] Reports of death from botched chelation therapy as treatment for autism have been documented.[227][228] Medical authorities have condemned bleach-based approaches, such as chlorine dioxide solutions marketed as Miracle Mineral Solution, as dangerous and ineffective.[229] The British NHS also warns against CEASE therapy, which rejects vaccinations and recommends potentially harmful amounts of dietary supplements.[230] There is also no evidence for the efficacy of hyperbaric oxygen therapy and its use is not recommended.[231]
Although sometimes used for autistic people, no reliable evidence indicates a gluten- and casein-free diet as a standard intervention.[232][233][234] Autistic children's preference for unconventional foods as well as gastrointestinal problems and lack of exercise can lead to reduction in bone cortical thickness, and this risk is greater in those on casein-free diets, as a consequence of the low intake of calcium and vitamin D.[235]
Emerging evidence-based interventions
Interventions for autistic adults have limited evidence; cognitive behavioral approaches and mindfulness are considered promising.[236] Music therapy for autistic people likely improves overall autism severity, global functioning, and quality of life, but evidence is unclear for social and communication skills.[237] Animal-assisted activities and therapies show promise in improving social communication, irritability, hyperactivity, and word usage in autistic people.[238]
Caregivers
Families who care for an autistic child often experience greater stress.[239] Parents may struggle to understand their child and to find appropriate care options. Affiliate stigma can also reduce quality of life, where negative attitudes toward the autistic child are extended to those close to them.[240] Family members who are themselves autistic may be better able to understand the autistic child.[66]
Prognosis
The prognosis after diagnosis of autism in childhood is poorly understood.[3] Some core diagnostic symptoms, including restricted and repetitive behaviors, are stable, but some gradual symptom changes occur.[241] Among children diagnosed before age 6, about 9 in 10 continue to meet diagnostic criteria one year later.[242] Some report that those with limited support needs are likely to have lessened autistic features over time,[243] while others argue that this perception is likely due to masking—hiding autistic characteristics to avoid stigma.[244] Long-term outcomes vary, in part due to variability in presentation between individuals and across affected domains.[242] Autistic adults are more likely to be unemployed and have greater mental health service needs than the general population.[15] About 85% of autistic people need support with independent living in adulthood.[245] Factors such as developing spoken language before age six, having an IQ above 50, and possessing marketable skills are associated with higher likelihood of independent living in adulthood.[246] Mortality among autistic people is approximately twice that of the general population, particularly among those with co-occurring neurologic or psychiatric disorders.[15]
Suicide
Risk factors for self-harm and suicidality include circumstances that could affect anyone but are more common among autistic people, such as mental health problems (e.g., anxiety disorder) and social problems (e.g., unemployment and social isolation). In addition, there are autism-specific factors, such as exhausting attempts to behave like a non-autistic person to avoid stigma and negative reactions of society towards autistic people (masking).[247] Autistic people are also at significantly increased risk of victimization, including bullying, sexual assault, and other forms of criminal abuse.[248] A 2019 meta-analysis found autistic people to be four times more likely to have depression than non-autistic people.[249]
Rates of suicidality vary significantly depending upon what is being measured.[247] This is partly because questionnaires developed for non-autistic subjects are not always valid for autistic people.[247] As of 2023, the Suicidal Behaviours Questionnaire–Autism Spectrum Conditions (SBQ-ASC) is the only test validated for autistic people.[247] According to some estimates, about a quarter of autistic youth[250] and a third of all autistic people[247][251] have experienced suicidal ideation at some point. Autistic people are about three times as likely as non-autistic people to make a suicide attempt.[78][252] Almost 10% of autistic youth[250] and 15% to 25% of autistic adults[247][251] have attempted suicide. Rates of suicide attempts and suicidal ideation are the same for people formally diagnosed with autism and people who have typical intelligence and are believed to be autistic but have not been diagnosed.[247] The suicide risk is higher for autistic people who are not cisgender males and do not have intellectual disabilities.[247][252]
Epidemiology
Most professionals believe that race, ethnicity, and socioeconomic background have limited effect on the occurrence of autism.[253]
Research indicates that autistic people are significantly more likely to be LGBTQ than the general population.[254] Autistic people are also significantly more likely to be non-theistic or non-religious.[255]
Co-occurring conditions

Several conditions can co-occur with autism at a higher rate than in the rest of the population.[256] This may be referred to as comorbidity, and may increase with age, causing difficulties for youth on the autism spectrum, and can make interventions and therapies more challenging. Features of autism and other diagnoses often overlap, and autism's characteristics can make traditional diagnostic procedures more difficult.[257][258] This is sometimes known as diagnostic overshadowing.[259] Common co-occurring conditions are:
- ADHD is seen in between 25% to 32% of autistic people.[260] Characteristics similar to those of ADHD can be part of an autism diagnosis.[261]
- Epilepsy occurs in about 10% of autistic people.[262] The risk is higher for older autistic people and those with intellectual disability.[263]
- Intellectual disabilities are some of the most common co-occurring conditions with autism (30% to 40%).[264] As autism diagnosis is increasingly given to people with lower support needs, there is a tendency for the proportion with co-occurring intellectual disability to decrease over time.
- Various anxiety disorders can co-occur with autism, with overall co-occurring rates of 17% to 23%.[260] Many anxiety disorders have characteristics better explained by autism itself, or are hard to distinguish from autism's features.[265]
- Rates of co-occurring depression in autistic people range from 9% to 13%.[260]
- Obsessive–compulsive disorder (OCD) occurs in 7% to 10% of autistic people.[260]
- Starting in adolescence, some autistic people fall under the criteria for the similar-looking schizoid personality disorder, which is characterized by a lack of interest in social relationships, a tendency toward a solitary or sheltered lifestyle, secretiveness, emotional coldness, detachment, and apathy.[266]
- Genetic conditions: About 10% of autistic people are diagnosed with a rare genetic syndrome such as Prader–Willi, Angelman, Fragile X, or 16p11.2 deletion syndrome.[267]
- Gastrointestinal problems are among the most commonly reported co-occurring medical conditions in autistic people, and occur at higher rates than in the general population.[268][269] Frequently reported issues include chronic constipation, diarrhea, abdominal pain, gastroesophageal reflux, and functional gastrointestinal disorders.[270] Gastrointestinal symptoms in autistic people have been associated with increased irritability, distress, sleep disturbances, and challenges in communication, particularly in children who have limited spoken language.[268][271][272][273] The underlying mechanisms are not fully understood and are likely multifactorial, involving interactions between diet, gut motility, sensory sensitivities, stress responses, and the gut-brain axis.[274][270]
- Sleep problems affect about two-thirds of autistic people at some point in childhood. These most commonly include symptoms of insomnia, such as difficulty falling asleep, frequent nocturnal awakenings, and early-morning awakenings. Sleep problems are associated with difficult behaviors and family stress, and are often a focus of clinical attention over and above the autism diagnosis.[275]
- Motor difficulties, including features of dyspraxia, are highly prevalent in autistic people,[276] and there is a significantly higher rate of joint hypermobility/hypermobility spectrum disorders/Ehlers-Danlos syndrome in autistic people.[277]
- There is tentative evidence that gender dysphoria occurs more frequently in autistic people.[278][279]
Prevalence
The World Health Organization notes that reports on prevalence vary widely. It estimates that about 1 in 127 children were autistic between 2012 and 2021 with a trend of increasing prevalence over time. This may reflect an underestimate of prevalence in low- and middle-income countries.[11][14] Surveillance studies in community samples of adults suggest a similar share of the adult population would meet diagnostic criteria if formally assessed.[15] The number of people diagnosed has increased since the 1990s, likely due to a combination of increased recognition of autism, better availability of diagnosis, and changes to the diagnostic criteria.[11] The increase in autism is largely attributable to changes in diagnostic practices, referral patterns, availability of services, age at diagnosis, and public awareness,[280][281][282] particularly among women,[283] though other unidentified environmental factors may exist.[284]
The Centers for Disease Control's Autism and Developmental Disabilities Monitoring Network reported that approximately 1 in 31 children in the United States is diagnosed with autism, based on data collected in 2022.[285] For 2016 data, the estimate was 1 in 54, compared to 1 in 68 in 2010 and 1 in 150 in 2000.[285] Diagnostic criteria for autism have changed significantly since the 1980s; for example, U.S. special-education autism classification was introduced in 1994.[286]
Sex ratio
Males are about three times more likely to be diagnosed with autism than females.[21] Several theories about the higher prevalence in males have been investigated.[287] Prevalence differences may be mainly due to a result of differences in expression of characteristics between males and females, with autistic women and girls showing less atypical behaviors and therefore being less likely to be diagnosed with autism.[288]
History
Etymology
In 1911, Swiss psychiatrist Paul Eugen Bleuler coined the German term Autismus to characterize the social withdrawal he observed in people with schizophrenia.[289] Rendered in English as autism, the term derives from the Greek word autos ("self").[290] Bleuler used the term for a symptom of adult schizophrenia: a person's retreat from reality into their own subjective world. He also mentioned "autistic thinking" as a fleeting, illogical thought process everyone experiences. In the mid-1920s, German psychiatrist Fritz Künkel categorized over 100 schizophrenic patients into four groups, one of which he labeled "autistic", highlighting disturbances in emotional life. In 1926, building on his work and Bleuler's, Grunya Sukhareva published an article about six boys who were musically gifted and had a tendency toward abstract thinking. She called their affects "flattened" and their tendency to avoid other children an "autistic attitude".[291] Scholars have credited Sukhareva with making observations that closely mirror ASD as described by the DSM-5 and ICD-11.[292] Her work expanded on the definition throughout her career while making great strides in differentiating ASD and schizophrenia nearly 30 years before the establishment of separate classifications for these diagnoses with the 1980 publication of the DSM-III.[293]
Society and culture

The autistic rights and neurodiversity movements argue autism should be accepted as a difference to be accommodated instead of cured,[295][296][297][298][299] although a minority of autistic people might still accept a cure.[300] Social-science scholars study autistic people in hopes of learning more about "autism as a culture, transcultural comparisons ... and research on social movements".[299] Events related to autism include World Autism Awareness Day, Autism Sunday, Autistic Pride Day, Autreat, and others.[301][302][303][304]
Focused interests are commonly found in autistic people and can include activism. Environmental activist Greta Thunberg has spoken favorably about her autism diagnosis, saying that autism can be a source of life purpose, as well as the basis of careers, hobbies, and friendships.[305][306][294] Entrepreneur and co-founder of Microsoft Bill Gates has written, "If I were growing up today, I probably would be diagnosed on the autism spectrum."[307]
Legal implications of diagnosis
In Sweden, people with an autism diagnosis are required to provide additional proof of suitability to apply for a driver's license[308] and may face barriers to entering military service.[309]
In the United Kingdom, an autistic police officer was rejected from firearms training, which a tribunal later ruled was illegal discrimination.[310]
In the United States, autism is generally a "disqualifying condition" for joining the military, but autistic people can apply for a medical waiver.[311]
Discrimination
Discrimination against autistic people occurs in various forms, both directly and indirectly, in a variety of settings, professional, educational, or clinical.[312] Such discrimination is often initiated after other people identify the autistic person as different from themselves, which may occur very quickly.[312] This discrimination sometimes leads to violence, assault, or social exclusion.[312] Various legal limitations on people with an autism diagnosis have also been considered discriminatory.[308][310]
Neurodiversity movement

Some autistic people and affiliated researchers[313] have advocated a shift in attitudes toward the view that autism is a difference, rather than a disease that ought to be treated or cured.[314][315][316] Critics have bemoaned the entrenchment of some of these groups' opinions, and that they speak to a select group of autistic people with limited difficulties.[297][317][299][318][319] Clinical and policy guidance in Australia, the United States, and the United Kingdom now promote neurodiversity-affirming language—for example, using "characteristics" instead of "symptoms" and avoiding words such as "cure".[320][181][321]
The neurodiversity movement and the autism rights movement are social movements within the context of disability rights, emphasizing the concept of neurodiversity, which describes the autism spectrum as a result of healthy and valuable variations in the human brain rather than a disorder to be cured.[297][322] The autism rights movement advocates including greater acceptance of autistic behaviors, therapies that focus on coping skills rather than imitating the behaviors of non-autistic people,[323] and the recognition of the autistic community as a minority group.[323][319] Autism rights or neurodiversity advocates believe that the autism spectrum is genetic and should be accepted as a healthy variation in the human genome.[297] These movements are not without detractors. A common argument against neurodiversity activists is that most have relatively low support needs, or are self-diagnosed, and do not represent the views of autistic people with higher support needs.[319][324][325] The argument has been made that only autistic people with lower support needs should be included under the neurodiversity banner, as autism with high support needs "may rightfully be viewed as a disability".[319] The concept of neurodiversity is contentious in autism advocacy and research groups and has led to infighting.[317][299]
See also
- Animal model of autism
- Autism and memory
- Autism in popular culture
- Autism in psychoanalysis
- Autistic art
- Controversies in autism
- Empathy in autistic people
- Global perceptions of autism
- List of autistic fictional characters
- List of films about autism
- Mechanism of autism
- Outline of autism
- Twice exceptional
- Violence and autism
Notes
References
- ↑ Diagnostic and Statistical Manual of Mental Disorders (5th ed.). American Psychiatric Association. 2013. p. 31. https://archive.org/details/diagnosticstatis0005unse.
- ↑ Whiteley, Paul; Carr, Kevin; Shattock, Paul (7 October 2019). "Is Autism Inborn And Lifelong For Everyone?" (in English). Neuropsychiatric Disease and Treatment 15: 2885–2891. doi:10.2147/NDT.S221901. PMID 31632036.
- ↑ 3.0 3.1 Steinhausen, H.-C.; Mohr Jensen, C.; Lauritsen, M. B. (13 January 2016). "A systematic review and meta-analysis of the long-term overall outcome of autism spectrum disorders in adolescence and adulthood". Acta Psychiatrica Scandinavica 133 (6): 445–452. doi:10.1111/acps.12559. PMID 26763353.
- ↑ Kamp-Becker, Inge (March 2024). "Autism spectrum disorder in ICD-11—a critical reflection of its possible impact on clinical practice and research" (in en). Molecular Psychiatry 29 (3): 633–638. doi:10.1038/s41380-023-02354-y. PMID 38273107. "In DSM-5 as well as in ICD-11, ASD is assigned to the category "neurodevelopmental disorders", characterized by impairments in cognition, communication, behavior and/or motor skills resulting from abnormal brain development.".
- ↑ 5.0 5.1 (World Health Organization: International Classification of Diseases version 11 (ICD-11)): https://icd.who.int/browse/2024-01/mms/en#437815624
- ↑ 6.0 6.1 "IACC Subcommittee Diagnostic Criteria - DSM-5 Planning Group". https://iacc.hhs.gov/about-iacc/subcommittees/resources/dsm5-diagnostic-criteria.shtml.
- ↑ Guidelines from the UK National Institute for Health & Care Excellence (NICE): https://www.nice.org.uk/guidance/cg170/resources/autism-spectrum-disorder-in-under-19s-support-and-management-pdf-35109745515205
- ↑ "ESCAP practice guidance for autism: a summary of evidence‑based recommendations for diagnosis and treatment". European Child & Adolescent Psychiatry 30 (6): 961–984. 2020. doi:10.1007/s00787-020-01587-4. PMID 32666205. PMC 8140956. https://www.autismeurope.org/wp-content/uploads/2020/09/Fuentes2020_Article_ESCAPPracticeGuidanceForAutism.pdf.
- ↑ "Autism spectrum disorder: Pathogenesis, biomarker, and intervention therapy". Medcomm 5 (3). 2024. doi:10.1002/mco2.497. PMID 38434761.
- ↑ Waizbard-Bartov, Einat; Fein, Deborah; Lord, Catherine; Amaral, David G. (2023). "Autism severity and its relationship to disability" (in en). Autism Research 16 (4): 685–696. doi:10.1002/aur.2898. PMID 36786314.
- ↑ 11.0 11.1 11.2 11.3 11.4 Cite error: Invalid
<ref>tag; no text was provided for refs namedAutism-Research - ↑ 12.0 12.1 12.2 Anderson-Chavarria, Melissa (14 September 2022). "The autism predicament: models of autism and their impact on autistic identity". Disability & Society 37 (8): 1321–1341. doi:10.1080/09687599.2021.1877117.
- ↑ 13.0 13.1 Ogundele, Michael O.; Morton, Michael J. S. (3 April 2025). "Subthreshold Autism and ADHD: A Brief Narrative Review for Frontline Clinicians". Pediatric Reports 17 (2): 42. doi:10.3390/pediatric17020042. PMID 40278522.
- ↑ 14.0 14.1 "Autism" (in en). 30 March 2022. https://www.who.int/news-room/fact-sheets/detail/autism-spectrum-disorders.
- ↑ 15.0 15.1 15.2 15.3 Hirota, Tomoya; King, Bryan H. (10 January 2023). "Autism Spectrum Disorder: A Review". JAMA 329 (2): 157–168. doi:10.1001/jama.2022.23661. PMID 36625807.
- ↑ 16.0 16.1 Tick, Beata; Bolton, Patrick; Happé, Francesca; Rutter, Michael; Rijsdijk, Frühling (2016). "Heritability of autism spectrum disorders: a meta-analysis of twin studies" (in en). Journal of Child Psychology and Psychiatry 57 (5): 585–595. doi:10.1111/jcpp.12499. PMID 26709141.
- ↑ Hodges, Holly; Fealko, Casey; Soares, Neelkamal (February 2020). "Autism spectrum disorder: definition, epidemiology, causes, and clinical evaluation". Translational Pediatrics 9 (Suppl 1): S55–S5S65. doi:10.21037/tp.2019.09.09. PMID 32206584.
- ↑ Ratajczak, Helen V. (1 March 2011). "Theoretical aspects of autism: Causes—A review". Journal of Immunotoxicology 8 (1): 68–79. doi:10.3109/1547691X.2010.545086. PMID 21299355.
- ↑ 19.0 19.1 "Annual Research Review: The role of the environment in the developmental psychopathology of autism spectrum condition". Journal of Child Psychology and Psychiatry, and Allied Disciplines 57 (3): 271–292. March 2016. doi:10.1111/jcpp.12501. OCLC 01307942. PMID 26782158.
- ↑ Alaghband-rad, Javad; Hajikarim-Hamedani, Arman; Motamed, Mahtab (2023). "Camouflage and masking behavior in adult autism". Frontiers in Psychiatry 14 (16). doi:10.3389/fpsyt.2023.1108110. PMID 37009119.
- ↑ 21.0 21.1 Loomes, Rachel; Hull, Laura; Mandy, William Polmear Locke (1 June 2017). "What Is the Male-to-Female Ratio in Autism Spectrum Disorder? A Systematic Review and Meta-Analysis". Journal of the American Academy of Child & Adolescent Psychiatry 56 (6): 466–474. doi:10.1016/j.jaac.2017.03.013. PMID 28545751.
- ↑ Bertelli, Marco O.; Azeem, Muhammad Waqar; Underwood, Lisa; Scattoni, Maria Luisa; Persico, Antonio M.; Ricciardello, Arianna; Sappok, Tanja; Bergmann, Thomas et al. (2022). "Autism Spectrum Disorder". Textbook of Psychiatry for Intellectual Disability and Autism Spectrum Disorder. pp. 369–455. doi:10.1007/978-3-319-95720-3_16. ISBN 978-3-319-95719-7. https://books.google.com/books?id=4mtvEAAAQBAJ&pg=PA391. "Persons with autism spectrum disorder and/or other neurodevelopmental problems are more likely than the general population to have transgender identity, non-heterosexual sexual orientation, and other gender non-conformities."
- ↑ Lord, Catherine; Charman, Tony; Havdahl, Alexandra; Carbone, Paul; Anagnostou, Evdokia; Boyd, Brian; Carr, Themba; de Vries, Petrus J et al. (2022). "The Lancet Commission on the future of care and clinical research in autism". The Lancet 399 (10321): 299–300. doi:10.1016/s0140-6736(21)01541-5. PMID 34883054.
- ↑ Graham Holmes, Laura; Ames, Jennifer L.; Massolo, Maria L.; Nunez, Denise M.; Croen, Lisa A. (1 April 2022). "Improving the Sexual and Reproductive Health and Health Care of Autistic People". Pediatrics (American Academy of Pediatrics) 149 (Supplement 4): e2020049437J. doi:10.1542/peds.2020-049437J. PMID 35363286. "A substantial proportion of autistic adolescents and adults are LGBTQIA+. Autistic people are more likely to be transgender or gender nonconforming compared with non-autistic people, and findings from a recent autism registry study suggest that among autistic people able to self-report on a survey, up to 18% of men and 43% of women may be sexual minorities.".
- ↑ Happé, Francesca (2018). "Why are savant skills and special talents associated with autism?". World Psychiatry 17 (3): 280–281. doi:10.1002/wps.20552. PMID 30192091.
- ↑ 26.0 26.1 "Fake and harmful autism 'treatments'" (in en). 2 May 2019. https://www.nhs.uk/conditions/autism/autism-and-everyday-life/fake-and-harmful-treatments/.
- ↑ 27.0 27.1 CDC (18 July 2024). "Treatment and Intervention for Autism Spectrum Disorder" (in en-us). https://www.cdc.gov/autism/treatment/index.html.
- ↑ 28.0 28.1 Doherty, Mary; McCowan, Sue; Shaw, Sebastian CK (2 April 2023). "Autistic SPACE: a novel framework for meeting the needs of autistic people in healthcare settings". British Journal of Hospital Medicine 84 (4): 1–9. doi:10.12968/hmed.2023.0006. PMID 37127416.
- ↑ 29.0 29.1 29.2 Mukerji, Cora; Mottron, Laurent; McPartland, James C. (2013), Volkmar, Fred R., ed. (in en), Enhanced Perceptual Functioning, New York: Springer, pp. 1117–1118, doi:10.1007/978-1-4419-1698-3_723, ISBN 978-1-4419-1698-3
- ↑ 30.0 30.1 30.2 30.3 Doyle, Nancy (14 October 2020). "Neurodiversity at work: a biopsychosocial model and the impact on working adults". British Medical Bulletin 135 (1): 108–125. doi:10.1093/bmb/ldaa021. PMID 32996572.
- ↑ "Medication Treatment for Autism" (in en). 19 April 2021. https://www.nichd.nih.gov/health/topics/autism/conditioninfo/treatments/medication-treatment.
- ↑ Rzepka-Migut, Beata; Paprocka, Justyna (2020). "Efficacy and Safety of Melatonin Treatment in Children with Autism Spectrum Disorder and Attention-Deficit/Hyperactivity Disorder—A Review of the Literature". Brain Sciences 10 (4): 219. doi:10.3390/brainsci10040219. PMID 32272607.
- ↑ Kapp, Steven K. Autistic community and the neurodiversity movement: Stories from the frontline. Springer Nature, 2020.
- ↑ Happé, Francesca; Frith, Uta (2020). "Annual Research Review: Looking back to look forward - changes in the concept of autism and implications for future research". Journal of Child Psychology and Psychiatry, and Allied Disciplines 61 (3): 218–232. doi:10.1111/jcpp.13176. PMID 31994188.
- ↑ "Disorder or difference? Autism researchers face off over field's terminology" (in en). https://www.science.org/content/article/disorder-or-difference-autism-researchers-face-over-field-s-terminology.
- ↑ Rodríguez Mega, Emiliano (10 May 2023). "'I am not a broken version of normal' — autistic people argue for a stronger voice in research". Nature 617 (7960): 238–241. doi:10.1038/d41586-023-01549-1. PMID 37165246.
- ↑ 37.0 37.1 37.2 37.3 37.4 37.5 "Autism: Signs and characteristics". 12 February 2025. https://www.canada.ca/en/public-health/services/diseases/autism-spectrum-disorder-asd/signs-characteristics.html.
- ↑ "What is Autism Spectrum Disorder?". 25 March 2020. https://www.cdc.gov/ncbddd/autism/facts.html.
- ↑ Autism spectrum disorder in adults: diagnosis and management, NICE, 14 June 2021, CG142, https://www.nice.org.uk/guidance/cg142, retrieved 24 October 2021
- ↑ "About autism spectrum disorder (ASD)" (in en). 18 January 2016. https://www.canada.ca/en/public-health/services/diseases/autism-spectrum-disorder-asd/about-autism-spectrum-disorder-asd.html.
- ↑ F84
- ↑ "Autism Spectrum Disorder". Handbook of Pragmatic Language Disorders. Cham, Switzerland: Springer. 2021. pp. 45–78. doi:10.1007/978-3-030-74985-9_3. ISBN 978-3-030-74984-2. OCLC 1269056169.
- ↑ Biopsychology (8th ed.). Boston, Massachusetts: Pearson. 2011. p. 235. ISBN 978-0-205-03099-6. OCLC 1085798897.
- ↑ "Cognitive Assessment". Autism Spectrum Disorders. American Psychiatric Association. 2018. doi:10.1176/appi.books.9781615371921. ISBN 978-1-61537-192-1.
- ↑ 45.0 45.1 45.2 45.3 45.4 45.5 DSM-5-TR.
- ↑ 46.0 46.1 46.2 CDC (19 July 2024). "Signs and Symptoms of Autism Spectrum Disorder" (in en-us). https://www.cdc.gov/autism/signs-symptoms/?CDC_AAref_Val=https://www.cdc.gov/ncbddd/autism/signs.html.
- ↑ "Identification and evaluation of children with autism spectrum disorders". Pediatrics 120 (5): 1183–1215. November 2007. doi:10.1542/peds.2007-2361. PMID 17967920. Bibcode: 2007Pedia.120.1183J.
- ↑ Henderson, Donna; Wayland, Sarah; White, Jamell (2023). Is This Autism?. p. 35. doi:10.4324/9781003242130. ISBN 978-1-003-24213-0.
- ↑ El-Salahi, Shama; Khaki, Zahra; Vohora, Reena (27 September 2023). "Experiences of Inclusive School Settings for Children and Young People on the Autism Spectrum in the UK: a Systematic Review" (in en). Review Journal of Autism and Developmental Disorders 12 (3): 517–534. doi:10.1007/s40489-023-00405-2.
- ↑ Henderson, Donna; Wayland, Sarah; White, Jamell (2023). Is This Autism?. pp. 32–79. doi:10.4324/9781003242130. ISBN 978-1-003-24213-0.
- ↑ 51.0 51.1 , Wikidata Q3064664
- ↑ "Alexithymia". Disorders of Emotion in Neurologic Disease. Handbook of Clinical Neurology. 183. Elsevier. 2021. pp. 47–62. doi:10.1016/b978-0-12-822290-4.00004-9. ISBN 978-0-12-822290-4.
- ↑ 53.0 53.1 Long, Emily L.; Catmur, Caroline; Bird, Geoffrey (9 January 2025). "The theory of mind hypothesis of autism: A critical evaluation of the status quo". Psychological Review. doi:10.1037/rev0000532. PMID 39786849.
- ↑ Milton, Damian Elgin Maclean; Heasman, Brett; Sheppard, Elizabeth (2021), Double Empathy, Springer, Cham, pp. 1509–1517, doi:10.1007/978-3-319-91280-6_102273, ISBN 978-3-319-91280-6
- ↑ 55.0 55.1 Milton, Damian; Gurbuz, Emine; López, Beatriz (November 2022). "The 'double empathy problem': Ten years on" (in en). Autism 26 (8): 1901–1903. doi:10.1177/13623613221129123. PMID 36263746.
- ↑ 56.0 56.1 Marocchini, Eleonora; Baldin, Irene (31 July 2024). "Cross-neurotype communication from an autistic point of view: Insights on autistic Theory of Mind from a focus group study". International Journal of Language & Communication Disorders 59 (6): 2465-2482. doi:10.1111/1460-6984.13095. https://onlinelibrary.wiley.com/doi/abs/10.1111/1460-6984.13095. Retrieved 16 February 2026.
- ↑ Murray, Dinah (2021). "Monotropism: An Interest-Based Account of Autism". in Volkmar, Fred R.. Encyclopedia of Autism Spectrum Disorders. Cham: Springer International Publishing. pp. 2954–2956. doi:10.1007/978-3-319-91280-6_102269. ISBN 978-3-319-91280-6.
- ↑ "Being Monotropic: Definition, Examples, and Benefits" (in en). 2024-09-20. https://psychcentral.com/autism/monotropic.
- ↑ 59.0 59.1 "Autism Spectrum Disorder: Communication Problems in Children". 18 August 2015. https://www.nidcd.nih.gov/health/autism-spectrum-disorder-communication-problems-children.
- ↑ "Language disorders: autism and other pervasive developmental disorders". Pediatric Clinics of North America 54 (3): 469–81, vi. June 2007. doi:10.1016/j.pcl.2007.02.011. PMID 17543905.
- ↑ 61.0 61.1 Byrne, Katherine; Sterrett, Kyle; Lord, Catherine (1 December 2024). "Examining the Transition from Single Words to Phrase Speech in Children with ASD: A Systematic Review". Clinical Child and Family Psychology Review 27 (4): 1031–1053. doi:10.1007/s10567-024-00507-1. PMID 39550470.
- ↑ Henderson, Donna; Wayland, Sarah; White, Jamell (2023). Is This Autism?. p. 60. doi:10.4324/9781003242130. ISBN 978-1-003-24213-0.
- ↑ "Autism: Overview". American Speech-Language-Hearing Association. https://www.asha.org/Practice-Portal/Clinical-Topics/Autism/.
- ↑ 64.0 64.1 "Social communication and language characteristics associated with high-functioning, verbal children and adults with autism spectrum disorder". Indiana Resource Center for Autism. https://www.iidc.indiana.edu/pages/Social-Communication-and-Language-Characteristics-Associated-with-High-Functioning-Verbal-Children-and-Adults-with-ASD.
- ↑ 65.0 65.1 "Is voice a marker for Autism spectrum disorder? A systematic review and meta-analysis". Autism Research 10 (3): 384–407. March 2017. doi:10.1002/aur.1678. PMID 27501063.
- ↑ 66.0 66.1 Watts, Georgina; Crompton, Catherine; Grainger, Catherine; Long, Joseph; Botha, Monique; Somerville, Mark; Cage, Eilidh (3 June 2024). "'A certain magic' – autistic adults' experiences of interacting with other autistic people and its relation to Quality of Life: A systematic review and thematic meta-synthesis". Autism 29 (9). doi:10.1177/13623613241255811. PMID 38829019.
- ↑ Maïano, Christophe; Normand, Claude L.; Salvas, Marie-Claude; Moullec, Grégory; Aimé, Annie (2016). "Prevalence of School Bullying Among Youth with Autism Spectrum Disorders: A Systematic Review and Meta-Analysis". Autism Research 9 (6): 601–615. doi:10.1002/aur.1568. PMID 26451871.
- ↑ Grace, Kana; Remington, Anna; Lloyd-Evans, Brynmor; Davies, Jade; Crane, Laura (1 November 2022). "Loneliness in autistic adults: A systematic review". Autism 26 (8): 2117–2135. doi:10.1177/13623613221077721. PMID 35257592.
- ↑ Yew, Rui Ying; Samuel, Priscilla; Hooley, Merrilyn; Mesibov, Gary B.; Stokes, Mark A. (2021). "A systematic review of romantic relationship initiation and maintenance factors in autism". Personal Relationships 28 (4): 777–802. doi:10.1111/pere.12397.
- ↑ 70.0 70.1 Cook, Julia; Hull, Laura; Crane, Laura; Mandy, William (1 November 2021). "Camouflaging in autism: A systematic review". Clinical Psychology Review 89. doi:10.1016/j.cpr.2021.102080. PMID 34563942.
- ↑ 71.0 71.1 71.2 "Autism spectrum disorder". The Lancet 392 (10146): 508–520. August 2018. doi:10.1016/S0140-6736(18)31129-2. PMID 30078460. Bibcode: 2018Lanc..392..508L.
- ↑ Henderson, Donna; Wayland, Sarah; White, Jamell (2023). "Repetitive or idiosyncratic behavior". Is This Autism?. pp. 101–115. doi:10.4324/9781003242130. ISBN 978-1-003-24213-0.
- ↑ 73.0 73.1 Henderson, Donna; Wayland, Sarah; White, Jamell (2023). "Flexibility". Is This Autism?. pp. 116–133. doi:10.4324/9781003242130. ISBN 978-1-003-24213-0.
- ↑ 74.0 74.1 Henderson, Donna; Wayland, Sarah; White, Jamell (2023). "Intense or atypical interests". Is This Autism?. pp. 134–149. doi:10.4324/9781003242130. ISBN 978-1-003-24213-0.
- ↑ DSM-5-TR, "Hyper- or hyporeactivity to sensory input or unusual interest in sensory aspects of the environment (e.g., apparent indifference to pain/temperature, adverse response to specific sounds or textures, excessive smelling or touching of objects, visual fascination with lights or movement)".
- ↑ Lung, Stephanie Lock Man; Picard, Ève; Soulières, Isabelle; Bertone, Armando (1 September 2024). "Identifying the functions of restricted and repetitive behaviours and interests in Autism: A scoping review". Research in Autism Spectrum Disorders 117. doi:10.1016/j.rasd.2024.102458.
- ↑ Henderson, Donna; Wayland, Sarah; White, Jamell (2023). Is This Autism?. pp. 178–179. doi:10.4324/9781003242130. ISBN 978-1-003-24213-0.
- ↑ 78.0 78.1 Blanchard, Ashley; Chihuri, Stanford; DiGuiseppi, Carolyn G.; Li, Guohua (1 October 2021). "Risk of Self-harm in Children and Adults With Autism Spectrum Disorder: A Systematic Review and Meta-analysis". JAMA Network Open 4 (10): e2130272. doi:10.1001/jamanetworkopen.2021.30272. PMID 34665237.
- ↑ 79.0 79.1 "The association between self-injurious behaviors and autism spectrum disorders". Psychology Research and Behavior Management 7: 125–36. April 2014. doi:10.2147/PRBM.S44635. PMID 24748827.
- ↑ 80.0 80.1 80.2 "Practitioner Review: Self-injurious behaviour in children with developmental delay". Journal of Child Psychology and Psychiatry 56 (10): 1042–54. October 2015. doi:10.1111/jcpp.12425. PMID 25916173. https://research.birmingham.ac.uk/en/publications/b511897e-5285-4447-8a90-1c5690dd3ca1.
- ↑ Vandewalle, Katie; Melia, Yvonne (1 March 2021). "Psychosocial and behavioural factors associated with self injurious behaviour (SIB) in individuals with autism spectrum disorders (ASD)". Research in Autism Spectrum Disorders 81. doi:10.1016/j.rasd.2020.101713.
- ↑ 82.0 82.1 82.2 82.3 Andersen, Allan M.; Lipkin, Paul H.; Law, J. Kiely (2021). "Encyclopedia of Autism Spectrum Disorders". in Volkmar, Fred R.. Encyclopedia of Autism Spectrum Disorders (2nd ed.). Cham: Springer International Publishing AG. ISBN 978-3-319-91280-6.
- ↑ Thomas, Bekah; Crowley, Meg; Riley, Samantha; Rezendes, Johnny (2024). Massachusetts Child Fatality Review (Report). https://www.mass.gov/doc/fy24-child-fatality-review-annual-report/download. Retrieved 2026-02-05.
- ↑ 84.0 84.1 84.2 84.3 White, Susan W.; Siegle, Greg J.; Kana, Rajesh; Rothman, Emily F. (1 August 2023). "Pathways to Psychopathology Among Autistic Adults" (in en). Current Psychiatry Reports 25 (8): 315–325. doi:10.1007/s11920-023-01429-5. PMID 37378790.
- ↑ 85.0 85.1 85.2 85.3 Lai, Meng-Chuan (2023). "Mental health challenges faced by autistic people" (in en). Nature Human Behaviour 7 (10): 1620–1637. doi:10.1038/s41562-023-01718-2. PMID 37864080.
- ↑ 86.0 86.1 86.2 86.3 Jahandideh, Pardis; Seyedmirzaei, Homa; Rasoulian, Pegah; Memari, Amirhossein (3 May 2025). "Low Battery Alarm; A Scoping Review of Autistic Burnout" (in en). Journal of Autism and Developmental Disorders. doi:10.1007/s10803-025-06860-6. PMID 40317352.
- ↑ "Autistic fatigue and burnout | Autism Space" (in en-GB). https://www.leicspart.nhs.uk/autism-space/health-and-lifestyle/autistic-fatigue-and-burnout/.
- ↑ 88.0 88.1 88.2 88.3 88.4 88.5 88.6 "Understanding autistic meltdowns and shutdowns, Autism Space" (in en). https://www.leicspart.nhs.uk/autism-space/health-and-lifestyle/meltdowns-and-shutdowns/.
- ↑ Wilson, Alexander C (1 June 2024). "Cognitive Profile in Autism and ADHD: A Meta-Analysis of Performance on the WAIS-IV and WISC-V". Archives of Clinical Neuropsychology 39 (4): 498–515. doi:10.1093/arclin/acad073. PMID 37779387.
- ↑ "The savant syndrome: an extraordinary condition. A synopsis: past, present, future". Philosophical Transactions of the Royal Society of London. Series B, Biological Sciences 364 (1522): 1351–1357. May 2009. doi:10.1098/rstb.2008.0326. PMID 19528017.
- ↑ Heaton, Pamela (2021). "Autistic Savants". Encyclopedia of Autism Spectrum Disorders. pp. 554–555. doi:10.1007/978-3-319-91280-6_1372. ISBN 978-3-319-91279-0.
- ↑ "Perception and apperception in autism: rejecting the inverse assumption". Philosophical Transactions of the Royal Society of London. Series B, Biological Sciences 364 (1522): 1393–1398. May 2009. doi:10.1098/rstb.2009.0001. PMID 19528022.
- ↑ 93.0 93.1 "The screening and diagnosis of autistic spectrum disorders". Journal of Autism and Developmental Disorders 29 (6): 439–484. December 1999. doi:10.1023/A:1021943802493. PMID 10638459. This paper represents a consensus of representatives from nine professional and four parent organizations in the US.
- ↑ "Advances in autism". Annual Review of Medicine 60: 367–380. 2009. doi:10.1146/annurev.med.60.053107.121225. PMID 19630577.
- ↑ "Automatic Assessment of Motor Impairments in Autism Spectrum Disorders: A Systematic Review". Cognitive Computation 14 (2): 624–659. 10 January 2022. doi:10.1007/s12559-021-09940-8. https://hal.science/hal-03520967.
- ↑ "Motor coordination in autism spectrum disorders: a synthesis and meta-analysis". Journal of Autism and Developmental Disorders 40 (10): 1227–1240. October 2010. doi:10.1007/s10803-010-0981-3. PMID 20195737.
- ↑ Wang, Leah A. L.; Petrulla, Victoria; Zampella, Casey J.; Waller, Rebecca; Schultz, Robert T. (2022). "Gross motor impairment and its relation to social skills in autism spectrum disorder: A systematic review and two meta-analyses" (in en). Psychological Bulletin 148 (3–4): 273–300. doi:10.1037/bul0000358. PMID 35511567.
- ↑ 98.0 98.1 Baraskewich, Jessica; von Ranson, Kristin M; McCrimmon, Adam; McMorris, Carly A (1 August 2021). "Feeding and eating problems in children and adolescents with autism: A scoping review". Autism 25 (6): 1505–1519. doi:10.1177/1362361321995631. PMID 33653157.
- ↑ Murray, Alayna; Koronczai, Beatrix; Király, Orsolya; Griffiths, Mark D.; Mannion, Arlene; Leader, Geraldine; Demetrovics, Zsolt (2021). "Autism, Problematic Internet Use and Gaming Disorder: A Systematic Review". Review Journal of Autism and Developmental Disorders (Springer) 9: 120–140. doi:10.1007/s40489-021-00243-0.
- ↑ MacOun, Sarah J.; Bedir, Buse; Sheehan, John (2022). "Autism across the Ages: An Abbreviated History". Handbook of Autism and Pervasive Developmental Disorder. Autism and Child Psychopathology Series. pp. 3–28. doi:10.1007/978-3-030-88538-0_1. ISBN 978-3-030-88537-3. OCLC 1341298051. "To date no one genetic feature or environmental cause has proven etiological in explaining most cases autism or has been able to account for rising rates of autism."
- ↑ Sauer, Ann Katrin; Stanton, Janelle E.; Hans, Sakshi; Grabrucker, Andreas M. (2021). "Autism Spectrum Disorders: Etiology and Pathology". in Grabrucker, Andreas M. (in en). Autism spectrum disorders. Brisbane: Exon Publications. pp. 1–16. doi:10.36255/exonpublications.autismspectrumdisorders.2021.etiology. ISBN 978-0-6450017-8-5. OCLC 1280592589. "The cause of ASD is unknown, but several genetic and non-genetic risk factors have been characterized that, alone or in combination, are implicated in the development of ASD."
- ↑ Kałużna-Czaplińska, Joanna; Żurawicz, Ewa; Jóźwik-Pruska, Jagoda (2018). "Focus on the Social Aspect of Autism" (in en). Journal of Autism and Developmental Disorders (Springer Nature) 48 (5): 1861–1867. 29 November 2017. doi:10.1007/s10803-017-3407-7. PMID 29188587. "Despite extensive ASD research lasting more than 60 years, its causes are still unknown.".
- ↑ Medavarapu, Srinivas; Marella, Lakshmi Lavanya; Sangem, Aneela; Kairam, Ram (2019). "Where is the Evidence? A Narrative Literature Review of the Treatment Modalities for Autism Spectrum Disorders". Cureus (Springer Nature) 11 (1). 16 January 2019. doi:10.7759/cureus.3901. PMID 30911457. "It is important to realize that the etiology of autism is unknown and at present, there is no cure, although there are interventions that may be effective in alleviating some symptoms and improving skills that may help autistic persons lead more productive lives.".
- ↑ 104.0 104.1 "The 'fractionable autism triad': a review of evidence from behavioural, genetic, cognitive and neural research". Neuropsychology Review 18 (4): 287–304. December 2008. doi:10.1007/s11065-008-9076-8. PMID 18956240.
- ↑ 105.0 105.1 "Time to give up on a single explanation for autism". Nature Neuroscience 9 (10): 1218–1220. October 2006. doi:10.1038/nn1770. PMID 17001340.
- ↑ 106.0 106.1 106.2 Modabbernia, Amirhossein; Velthorst, Eva; Reichenberg, Abraham (17 March 2017). "Environmental risk factors for autism: an evidence-based review of systematic reviews and meta-analyses". Molecular Autism 8 (1): 13. doi:10.1186/s13229-017-0121-4. PMID 28331572.
- ↑ "The origins of social impairments in autism spectrum disorder: studies of infants at risk". Neural Networks 23 (8–9): 1072–6. 2010. doi:10.1016/j.neunet.2010.07.008. PMID 20800990.
- ↑ "Autism and the environment: challenges and opportunities for research". Pediatrics 121 (6): 1225–1229. June 2008. doi:10.1542/peds.2007-3000. PMID 18519493.
- ↑ 109.0 109.1 109.2 "Advances in autism genetics: on the threshold of a new neurobiology". Nature Reviews. Genetics 9 (5): 341–355. May 2008. doi:10.1038/nrg2346. PMID 18414403.
- ↑ "Multiple rare variants in the etiology of autism spectrum disorders". Dialogues in Clinical Neuroscience 11 (1): 35–43. 2009. doi:10.31887/DCNS.2009.11.1/jdbuxbaum. PMID 19432386.
- ↑ "Autism genetics". Behavioural Brain Research 251: 95–112. August 2013. doi:10.1016/j.bbr.2013.06.012. PMID 23769996.
- ↑ Goh, Shuxiang; Thiyagarajan, Lavvina; Dudding-Byth, Tracy; Pinese, Mark; Kirk, Edwin P. (1 January 2025). "A systematic review and pooled analysis of penetrance estimates of copy-number variants associated with neurodevelopment". Genetics in Medicine 27 (1). doi:10.1016/j.gim.2024.101227. PMID 39092588.
- ↑ "Autism: definition, neurobiology, screening, diagnosis". Pediatric Clinics of North America 55 (5): 1129–46, viii. October 2008. doi:10.1016/j.pcl.2008.07.005. PMID 18929056.
- ↑ Fernandez, Bridget A.; Scherer, Stephen W. (2017). "Syndromic autism spectrum disorders: moving from a clinically defined to a molecularly defined approach". Dialogues in Clinical Neuroscience 19 (4): 353–371. doi:10.31887/DCNS.2017.19.4/sscherer. PMID 29398931.
- ↑ Wiśniowiecka-Kowalnik, Barbara; Nowakowska, Beata Anna (1 February 2019). "Genetics and epigenetics of autism spectrum disorder—current evidence in the field" (in en). Journal of Applied Genetics 60 (1): 37–47. doi:10.1007/s13353-018-00480-w. PMID 30627967.
- ↑ Woodbury-Smith, Marc; Scherer, Stephen W (2018). "Progress in the genetics of autism spectrum disorder". Developmental Medicine & Child Neurology 60 (5): 445–451. doi:10.1111/dmcn.13717. PMID 29574884.
- ↑ "Childhood autism and associated comorbidities". Brain & Development 29 (5): 257–272. June 2007. doi:10.1016/j.braindev.2006.09.003. PMID 17084999.
- ↑ Holder, J. Lloyd; Hamdan, Fadi F.; Michaud, Jacques L. (1993). "SYNGAP1-Related Intellectual Disability". GeneReviews®. University of Washington, Seattle. https://www.ncbi.nlm.nih.gov/books/NBK537721/.
- ↑ "The emerging picture of autism spectrum disorder: genetics and pathology". Annual Review of Pathology: Mechanisms of Disease 10: 111–44. 2015. doi:10.1146/annurev-pathol-012414-040405. PMID 25621659.
- ↑ The pattern seekers: how autism drives human invention. Basic Books. 10 November 2020. ISBN 978-1-5416-4713-8. OCLC 1204602315.
- ↑ "Copy-number variations associated with neuropsychiatric conditions". Nature 455 (7215): 919–923. October 2008. doi:10.1038/nature07458. PMID 18923514. Bibcode: 2008Natur.455..919C.
- ↑ "Autism: highly heritable but not inherited". Nature Medicine 13 (5): 534–536. May 2007. doi:10.1038/nm0507-534. PMID 17479094.
- ↑ Geschwind, Daniel H. (31 October 2008). "Autism: Many Genes, Common Pathways?" (in English). Cell 135 (3): 391–395. doi:10.1016/j.cell.2008.10.016. PMID 18984147.
- ↑ "The Stone Age Origins of Autism" (in en). Recent Advances in Autism Spectrum Disorders. II. 6 March 2013.
- ↑ Nesse, Randolph M. (June 2023). "Evolutionary psychiatry: foundations, progress and challenges" (in en). World Psychiatry 22 (2): 177–202. doi:10.1002/wps.21072. PMID 37159362.
- ↑ Markram, Kamila; Markram, Henry (21 December 2010). "The Intense World Theory – A Unifying Theory of the Neurobiology of Autism" (in English). Frontiers in Human Neuroscience 4: 224. doi:10.3389/fnhum.2010.00224. PMID 21191475.
- ↑ 127.0 127.1 127.2 127.3 Fletcher-Watson, Sue; Happé, Francesca (2019). Autism: A New Introduction to Psychological Theory and Current Debate (2nd ed.). Milton: Taylor & Francis Group. ISBN 978-1-138-10612-3.
- ↑ Wang, Chengzhong; Geng, Hua; Liu, Weidong; Zhang, Guiqin (2017). "Prenatal, perinatal, and postnatal factors associated with autism: A meta-analysis". Medicine (Lippincott Williams & Wilkins) 96 (18). doi:10.1097/MD.0000000000006696. PMID 28471964.
- ↑ 129.0 129.1 129.2 "Perinatal and neonatal risk factors for autism: a comprehensive meta-analysis". Pediatrics 128 (2): 344–55. August 2011. doi:10.1542/peds.2010-1036. PMID 21746727. Bibcode: 2011Pedia.128..344G.
- ↑ Sandin, Sven; Hultman, Christina M.; Kolevzon, Alexander; Gross, Raz; MacCabe, James H.; Reichenberg, Abraham (2012). "Advancing Maternal Age Is Associated With Increasing Risk for Autism: A Review and Meta-Analysis". Journal of the American Academy of Child & Adolescent Psychiatry (Elsevier) 51 (5): 477–486.e1. doi:10.1016/j.jaac.2012.02.018. PMID 22525954.
- ↑ de Kluiver, Hilde; Buizer-Voskamp, Jacobine E.; Dolan, Conor V.; Boomsma, Dorret I. (2017). "Paternal age and psychiatric disorders: A review". American Journal of Medical Genetics (Wiley-Blackwell) 174 (3): 202–213. doi:10.1002/ajmg.b.32508. PMID 27770494.
- ↑ Jash, Sukanta; Sharma, Surendra (2022-04-29). "Viral Infections and Temporal Programming of Autism Spectrum Disorders in the Mother's Womb" (in English). Frontiers in Virology 2. doi:10.3389/fviro.2022.863202.
- ↑ "Neurodevelopment: The Impact of Nutrition and Inflammation During Preconception and Pregnancy in Low-Resource Settings". Pediatrics 139 (Suppl 1): S38–S49. April 2017. doi:10.1542/peds.2016-2828F. PMID 28562247.
- ↑ "A Systematic Review and Meta-Analysis of Multiple Airborne Pollutants and Autism Spectrum Disorder". PLOS ONE 11 (9). 2016. doi:10.1371/journal.pone.0161851. PMID 27653281. Bibcode: 2016PLoSO..1161851L.
- ↑ Amaral, David G. (2017). "Examining the Causes of Autism". Cerebrum: The Dana Forum on Brain Science 2017: cer–01–17. PMID 28698772.
- ↑ 136.0 136.1 Gyawali, Shreeya; Patra, Bichitra Nanda (February 2019). "Trends in concept and nosology of autism spectrum disorder: A review". Asian Journal of Psychiatry 40: 92–99. doi:10.1016/j.ajp.2019.01.021. PMID 30776666.
- ↑ Donvan, John; Zucker, Caren (2017). In a Different Key: The Story of Autism. Crown. pp. 89–91. ISBN 978-0-307-98570-5. https://books.google.com/books?id=QB6-DQAAQBAJ&q=%22It+was+confounding.++If+Kanner+now+blamed+parents%2C+that+represented+a+significant+about-face+on+his+part.%22&pg=PA90.
- ↑ Waltz, Mitzi M. (1 April 2015). "Mothers and Autism: The Evolution of a Discourse of Blame" (in en). AMA Journal of Ethics 17 (4): 353–358. doi:10.1001/journalofethics.2015.17.4.mhst1-1504. PMID 25901704.
- ↑ Cleary, Michelle; West, Sancia; Mclean, Loyola (1 September 2022). "From 'Refrigerator Mothers' to Empowered Advocates: The Evolution of the Autism Parent". Issues in Mental Health Nursing 44 (1): 64–70. doi:10.1080/01612840.2022.2115594. PMID 36049183.
- ↑ 140.0 140.1 "Vaccines and autism: a tale of shifting hypotheses". Clinical Infectious Diseases 48 (4): 456–461. February 2009. doi:10.1086/596476. PMID 19128068.
- ↑ "MMR doctor Andrew Wakefield fixed data on autism". The Sunday Times. 8 February 2009. https://www.thetimes.co.uk/article/mmr-doctor-andrew-wakefield-fixed-data-on-autism-mgj82qsk50g.
- ↑ "Lancet retracts 'utterly false' MMR paper". The Guardian. 2 February 2010. https://www.theguardian.com/society/2010/feb/02/lancet-retracts-mmr-paper.
- ↑ "Influenza Vaccine". Adverse Effects of Vaccines: Evidence and Causality. Committee to Review Adverse Effects of Vaccines, Board on Population Health and Public Health Practice. Washington, D.C.: Institute of Medicine/National Academies Press. August 2011. doi:10.17226/13164. ISBN 978-0-309-21435-3. Bibcode: 2011nap..book13164I. https://nap.nationalacademies.org/read/13164/chapter/8. Retrieved 19 January 2019.
- ↑ "The vaccine-autism connection: a public health crisis caused by unethical medical practices and fraudulent science". The Annals of Pharmacotherapy 45 (10): 1302–1304. October 2011. doi:10.1345/aph.1Q318. PMID 21917556.
- ↑ "Wakefield's article linking MMR vaccine and autism was fraudulent". British Medical Journal 342. January 2011. doi:10.1136/bmj.c7452. PMID 21209060.
- ↑ McKee, Maggie (4 March 2004). "Controversial MMR and autism study retracted". New Scientist. https://www.newscientist.com/article/dn4743-controversial-mmr-and-autism-study-retracted/. Retrieved 21 October 2015.
- ↑ "General Medical Council, Fitness to Practise Panel Hearing, 24 May 2010, Andrew Wakefield, Determination of Serious Professional Misconduct". http://www.gmc-uk.org/Wakefield_SPM_and_SANCTION.pdf_32595267.pdf.
- ↑ 148.0 148.1 "The MMR Vaccine and Autism". Annual Review of Virology 6 (1): 585–600. September 2019. doi:10.1146/annurev-virology-092818-015515. PMID 30986133.
- ↑ 149.0 149.1 "Understanding Vaccines, Mercury and Thimerosal". https://www.fda.gov/media/83535/download.
- ↑ Dona, Asif (2006). "Immunizations and Autism: A Review of the Literature". Canadian Journal of Neurological Sciences 33 (4): 341–346. doi:10.1017/S031716710000528X. PMID 17168158.
- ↑ "Thimerosal questions and answers". 18 February 2021. https://www.fda.gov/vaccines-blood-biologics/vaccines/thimerosal-vaccines-questions-and-answers.
- ↑ "Autism overflows: increasing prevalence and proliferating theories". Neuropsychology Review 18 (4): 273–286. December 2008. doi:10.1007/s11065-008-9074-x. PMID 19015994.
- ↑ "87% of Flu Vaccine Doses have Reduced or "no" (only trace amounts of) Thimerosal". 16 September 2022. https://www.cdc.gov/flu/prevent/vaxsupply.htm.
- ↑ "Frequently Asked Questions about Thimerosal". Centers for Disease Control and Prevention. https://www.cdc.gov/vaccinesafety/concerns/thimerosal/faqs.html.
- ↑ "Vaccines are not associated with autism: an evidence-based meta-analysis of case-control and cohort studies". Vaccine 32 (29): 3623–3629. June 2014. doi:10.1016/j.vaccine.2014.04.085. PMID 24814559.
- ↑ Vaccines and autism:
- "Immunizations and autism: a review of the literature". The Canadian Journal of Neurological Sciences. Le Journal Canadien des Sciences Neurologiques 33 (4): 341–346. November 2006. doi:10.1017/s031716710000528x. PMID 17168158.
- "Vaccines and autism: a tale of shifting hypotheses". Clinical Infectious Diseases 48 (4): 456–461. February 2009. doi:10.1086/596476. PMID 19128068.
- "A broken trust: lessons from the vaccine--autism wars". PLOS Biology 7 (5). May 2009. doi:10.1371/journal.pbio.1000114. PMID 19478850.
- "Parents ask: Am I risking autism if I vaccinate my children?". Journal of Autism and Developmental Disorders 39 (6): 962–963. June 2009. doi:10.1007/s10803-009-0739-y. PMID 19363650.
- "The age-old struggle against the antivaccinationists". New England Journal of Medicine 364 (2): 97–99. January 2011. doi:10.1056/NEJMp1010594. PMID 21226573.
- ↑ "Measles outbreak in Dublin, 2000". The Pediatric Infectious Disease Journal 22 (7): 580–584. July 2003. doi:10.1097/00006454-200307000-00002. PMID 12867830.
- ↑ "Trump falsely claims Amish 'have essentially no autism'" (in en). Fact Check. https://factcheck.afp.com/doc.afp.com.76JJ7G3.
- ↑ Spencer, Saranac Hale (2023-07-21). "False Claim About Cause of Autism Highlighted on Pennsylvania Senate Panel" (in en-US). https://www.factcheck.org/2023/07/scicheck-false-claim-about-cause-of-autism-highlighted-on-pennsylvania-senate-panel/.
- ↑ "Anti-vaccine myth that Amish children don't have autism resurfaces - Public Health Communications Collaborative" (in en-US). 2023-06-28. https://publichealthcollaborative.org/alerts/anti-vaccine-myth-that-amish-children-dont-have-autism-resurfaces/.
- ↑ "Amish people do vaccinate - and autism exists in Amish communities – Full Fact" (in en). 2025-10-29. https://fullfact.org/health/amish-autism-vaccines/.
- ↑ 162.0 162.1 162.2 ICD-11.
- ↑ "The autistic spectrum". The Lancet 350 (9093): 1761–1766. December 1997. doi:10.1016/S0140-6736(97)09218-0. PMID 9413479.
- ↑ Clinical descriptions and diagnostic requirements for ICD-11 mental, behavioural and neurodevelopmental disorders. World Health Organization. 2024. ISBN 978-92-4-007726-3. https://www.who.int/publications/i/item/9789240077263.
- ↑ Sturmey, Peter; Dalfern, Samantha (1 December 2014). "The Effects of DSM5 Autism Diagnostic Criteria on Number of Individuals Diagnosed with Autism Spectrum Disorders: A Systematic Review". Review Journal of Autism and Developmental Disorders 1 (4): 249–252. doi:10.1007/s40489-014-0016-7.
- ↑ 166.0 166.1 Status on ICD-11: The WHO Launch (Report). CDC/NCHS. 18 July 2018. https://ncvhs.hhs.gov/wp-content/uploads/2018/08/ICD-11_WHO-v_7-17-2018.pdf. Retrieved 22 October 2021.
- ↑ "ICD vs. DSM". APA Monitor (American Psychological Association) 40 (9): p. 63. 2009. https://www.apa.org/monitor/2009/10/icd-dsm.
- ↑ "International surveys on the use of ICD-10 and related diagnostic systems". Psychopathology 35 (2–3): 72–75. 2002. doi:10.1159/000065122. PMID 12145487.
- ↑ "The classification of mental disorder: a simpler system for DSM–V and ICD–11". Advances in Psychiatric Treatment 16 (1): 14–19. January 2010. doi:10.1192/apt.bp.109.007120.
- ↑ "ICD-11 for Mortality and Morbidity Statistics". https://icd.who.int/browse/2025-01/mms/en#437815624.
- ↑ Waterhouse, Lynn; Mottron, Laurent (2 May 2023). "Editorial: Is autism a biological entity?". Frontiers in Psychiatry 14. doi:10.3389/fpsyt.2023.1180981. PMID 37200904.
- ↑ 172.0 172.1 Chawner, Samuel (2 September 2022). "Autism: A model of neurodevelopmental diversity informed by genomics". Frontiers in Psychiatry 13. doi:10.3389/fpsyt.2022.981691. PMID 36117659.
- ↑ "DSM" (in en). https://www.psychiatry.org/psychiatrists/practice/dsm.
- ↑ Grzadzinski, Rebecca; Huerta, Marisela; Lord, Catherine (15 May 2013). "DSM-5 and autism spectrum disorders (ASDs): an opportunity for identifying ASD subtypes". Molecular Autism 4 (1): 12. doi:10.1186/2040-2392-4-12. PMID 23675638. "Consequently, the fifth edition of the DSM (DSM-5) replaces the multi-categorical system with a single diagnostic dimension: ASD.".
- ↑ 175.0 175.1 Lai, Meng-Chuan; Lombardo, Michael V.; Chakrabarti, Bhismadev; Baron-Cohen, Simon (23 April 2013). "Subgrouping the Autism 'Spectrum': Reflections on DSM-5" (in en). PLOS Biology 11 (4). doi:10.1371/journal.pbio.1001544. PMID 23630456. "New in DSM-5 is the explicit recognition of the "spectrum" nature of autism, subsuming and replacing the DSM-IV Pervasive Developmental Disorder (PDD) categorical subgroups of "autistic disorder," "Asperger's disorder," "pervasive developmental disorder not otherwise specified," and "childhood disintegrative disorder" into a single umbrella term "Autism Spectrum Disorder" (ASD).".
- ↑ DSM-5-TR, "Autism spectrum disorder encompasses disorders previously referred to as early infantile autism, childhood autism, Kanner's autism, high-functioning autism, atypical autism, pervasive developmental disorder not otherwise specified, childhood disintegrative disorder, and Asperger's disorder".
- ↑ "How will DSM-5 affect autism diagnosis? A systematic literature review and meta-analysis". Journal of Autism and Developmental Disorders 44 (8): 1918–1932. August 2014. doi:10.1007/s10803-014-2065-2. PMID 24531932.
- ↑ "DSM-5 Diagnostic Criteria". U.S. Department of Health & Human Services Interagency Autism Coordinating Committee. https://iacc.hhs.gov/about-iacc/subcommittees/resources/dsm5-diagnostic-criteria.shtml#autism-spectrum-disorder.
- ↑ "WHO releases new International Classification of Diseases (ICD 11)". https://www.who.int/news/item/18-06-2018-who-releases-new-international-classification-of-diseases-(icd-11).
- ↑ 181.0 181.1 England, N. H. S.. "NHS England » Making information and the words we use accessible" (in en-US). https://www.england.nhs.uk/learning-disabilities/about/get-involved/involving-people/making-information-and-the-words-we-use-accessible/.
- ↑ "How to talk about autism" (in en). https://www.autism.org.uk/what-we-do/help-and-support/how-to-talk-about-autism.
- ↑ "The psychiatric management of autism in adults (CR228)" (in en). https://www.rcpsych.ac.uk/improving-care/campaigning-for-better-mental-health-policy/college-reports/2020-college-reports/cr228.
- ↑ 184.0 184.1 Chapman, Robert; Bovell, Virginia (2022). "Neurodiversity, Advocacy, Anti-Therapy". in Matson, Johnny L.; Sturmey, Peter. Handbook of Autism and Pervasive Developmental Disorder: Assessment, Diagnosis, and Treatment. Cham: Springer International Publishing. pp. 1519–1536. doi:10.1007/978-3-030-88538-0_67. ISBN 978-3-030-88538-0.
- ↑ Leadbitter, Kathy; Buckle, Karen Leneh; Ellis, Ceri; Dekker, Martijn (12 April 2021). "Autistic Self-Advocacy and the Neurodiversity Movement: Implications for Autism Early Intervention Research and Practice". Frontiers in Psychology 12. doi:10.3389/fpsyg.2021.635690. PMID 33912110.
- ↑ "Behavioural and developmental interventions for autism spectrum disorder: a clinical systematic review". PLOS ONE 3 (11). 2008. doi:10.1371/journal.pone.0003755. PMID 19015734. Bibcode: 2008PLoSO...3.3755O.
- ↑ 187.0 187.1 187.2 187.3 187.4 187.5 "Evidence Base Update for Autism Spectrum Disorder". Journal of Clinical Child and Adolescent Psychology (Taylor & Francis) 44 (6): 897–922. 2015. doi:10.1080/15374416.2015.1077448. PMID 26430947.
- ↑ "10 Facts about Autism Spectrum Disorder (ASD)". 4 November 2020. https://acf.gov/ecd/10-facts-about-asd.
- ↑ 189.0 189.1 189.2 189.3 "Management of children with autism spectrum disorders". Pediatrics 120 (5): 1162–1182. November 2007. doi:10.1542/peds.2007-2362. PMID 17967921.
- ↑ "Meta-analysis of Early Intensive Behavioral Intervention for children with autism". Journal of Clinical Child and Adolescent Psychology (Taylor & Francis) 38 (3): 439–450. May 2009. doi:10.1080/15374410902851739. PMID 19437303.
- ↑ "NIMH » Autism Spectrum Disorder". National Institutes of Health (US). https://www.nimh.nih.gov/health/publications/autism-spectrum-disorder.
- ↑ 192.0 192.1 192.2 "An update on pharmacotherapy for autism spectrum disorder in children and adolescents". Current Opinion in Psychiatry 28 (2): 91–101. March 2015. doi:10.1097/YCO.0000000000000132. PMID 25602248.
- ↑ Sandbank, Micheal; Bottema-Beutel, Kristen; LaPoint, Shannon Crowley; Feldman, Jacob I.; Barrett, D. Jonah; Caldwell, Nicolette; Dunham, Kacie; Crank, Jenna et al. (14 November 2023). "Autism intervention meta-analysis of early childhood studies (Project AIM): updated systematic review and secondary analysis". BMJ 383. doi:10.1136/bmj-2023-076733. PMID 37963634.
- ↑ "Cognitive Behavioral Therapy for Autism Spectrum Disorders: A Systematic Review". Pediatrics (American Academy of Pediatrics (AAP)) 147 (5). May 2021. doi:10.1542/peds.2020-049880. PMID 33888566.
- ↑ 195.0 195.1 "Communication interventions for autism spectrum disorder in minimally verbal children". The Cochrane Database of Systematic Reviews 2018 (11). November 2018. doi:10.1002/14651858.CD012324.pub2. PMID 30395694.
- ↑ "Quality of early intensive behavioral intervention as a predictor of children's outcome". Behavior Modification 45 (6): 911–928. November 2021. doi:10.1177/0145445520923998. PMID 32436396.
- ↑ 197.0 197.1 "Spoken language outcomes in limited language preschoolers with autism and global developmental delay: RCT of early intervention approaches". Autism Research 16 (6): 1236–1246. June 2023. doi:10.1002/aur.2932. PMID 37070270.
- ↑ Reichow, Brian; Hume, Kara; Barton, Erin E.; Boyd, Brian A. (2018). "Early intensive behavioral intervention (EIBI) for young children with autism spectrum disorders (ASD)". Cochrane Database of Systematic Reviews 5 (10). doi:10.1002/14651858.CD009260.pub3. PMID 29742275.
- ↑ Sandbank, Micheal; Bottema-Beutel, Kristen; LaPoint, Shannon Crowley; Feldman, Jacob I.; Barrett, D. Jonah; Caldwell, Nicolette; Dunham, Kacie; Crank, Jenna et al. (14 November 2023). "Autism intervention meta-analysis of early childhood studies (Project AIM): updated systematic review and secondary analysis". BMJ 383. doi:10.1136/bmj-2023-076733. PMID 37963634.
- ↑ 200.0 200.1 Sandoval-Norton, Aileen Herlinda; Shkedy, Gary; Shkedy, Dalia (1 January 2019). Rushby, Jacqueline Ann. ed. "How much compliance is too much compliance: Is long-term ABA therapy abuse?" (in en). Cogent Psychology 6 (1). doi:10.1080/23311908.2019.1641258.
- ↑ Shkedy, Gary; Shkedy, Dalia; Sandoval-Norton, Aileen H. (June 2021). "Long-term ABA Therapy Is Abusive: A Response to Gorycki, Ruppel, and Zane" (in en). Advances in Neurodevelopmental Disorders 5 (2): 126–134. doi:10.1007/s41252-021-00201-1.
- ↑ Anderson, Laura K (April 2023). "Autistic experiences of applied behavior analysis". Autism 27 (3): 737–750. doi:10.1177/13623613221118216. PMID 35999706.
- ↑ Kirkham, Patrick (1 April 2017). "'The line between intervention and abuse' – autism and applied behaviour analysis". History of the Human Sciences 30 (2): 107–126. doi:10.1177/0952695117702571.
- ↑ Bottema-Beutel, Kristen; Crowley, Shannon; Sandbank, Micheal; Woynaroski, Tiffany G. (2021). "Research Review: Conflicts of Interest (COIs) in autism early intervention research - a meta-analysis of COI influences on intervention effects". Journal of Child Psychology and Psychiatry, and Allied Disciplines 62 (1): 5–15. doi:10.1111/jcpp.13249. PMID 32353179.
- ↑ Gorycki, Kathryn A.; Ruppel, Paula R.; Zane, Thomas (31 December 2020). Navalta, Carryl P.. ed. "Is long-term ABA therapy abusive: A response to Sandoval-Norton and Shkedy". Cogent Psychology 7 (1). doi:10.1080/23311908.2020.1823615.
- ↑ "Evidence-based, parent-mediated interventions for young children with autism spectrum disorder: The case of restricted and repetitive behaviors" (in en-US). Autism 19 (6): 662–72. August 2015. doi:10.1177/1362361314545685. PMID 25186943.
- ↑ 207.0 207.1 207.2 207.3 Ducarre, Lucie Margot (10 July 2024). "Redefining the Right to Quality Education for Autistic Children Through a Neurodiverse Perspective". Scandinavian Journal of Disability Research 26 (1): 366–379. doi:10.16993/sjdr.1043.
- ↑ 208.0 208.1 Prosser, Rebecca; Birchwood, James (1 July 2024). "A systematic review identifying factors associated with emotionally based school non-attendance in autistic children and young people". Educational and Child Psychology 41 (1): 31–54. doi:10.53841/bpsecp.2024.41.1.31.
- ↑ 209.0 209.1 Mitchell, Fiona (14 December 2023). "Promoting inclusive practice for autistic learners: Universal design for learning". Kairaranga 24 (2): 30–51. doi:10.54322/j7wy5s57.
- ↑ McVey, Alana J.; Jones, Desiree R.; Waisman, T. C.; Raymaker, Dora M.; Nicolaidis, Christina; Maddox, Brenna B. (31 August 2023). "Mindshift in autism: a call to professionals in research, clinical, and educational settings" (in en). Frontiers in Psychiatry 14. doi:10.3389/fpsyt.2023.1251058. PMID 37720894.
- ↑ Clouder, Lynn; Karakus, Mehmet; Cinotti, Alessia; Ferreyra, María Virginia; Fierros, Genoveva Amador; Rojo, Patricia (1 October 2020). "Neurodiversity in higher education: a narrative synthesis". Higher Education 80 (4): 757–778. doi:10.1007/s10734-020-00513-6. https://pureportal.coventry.ac.uk/en/publications/15ff4edd-256a-4c58-8dfb-b39afa9277ca.
- ↑ Whelpley, Christopher E.; May, Cynthia P. (1 April 2023). "Seeing is Disliking: Evidence of Bias Against Individuals with Autism Spectrum Disorder in Traditional Job Interviews" (in en). Journal of Autism and Developmental Disorders 53 (4): 1363–1374. doi:10.1007/s10803-022-05432-2. PMID 35294714.
- ↑ 213.0 213.1 213.2 Smith, Theo (2021). Kirby, Amanda. ed. Neurodiversity at work: drive innovation, performance and productivity with a neurodiverse workforce. London, United Kingdom New York, NY New Delhi: Kogan Page. ISBN 978-1-3986-0026-3.
- ↑ Goldfarb, Yael; Gal, Eynat; Golan, Ofer (1 January 2022). "Implications of Employment Changes Caused by COVID-19 on Mental Health and Work-Related Psychological Need Satisfaction of Autistic Employees: A Mixed-Methods Longitudinal Study" (in en). Journal of Autism and Developmental Disorders 52 (1): 89–102. doi:10.1007/s10803-021-04902-3. PMID 33635422.
- ↑ Tomczak, Michał T.; Mpofu, Elias; Hutson, Nathan (2 September 2022). "Remote Work Support Needs of Employees with Autism Spectrum Disorder in Poland: Perspectives of Individuals with Autism and Their Coworkers". International Journal of Environmental Research and Public Health 19 (17). doi:10.3390/ijerph191710982. PMID 36078696.
- ↑ Dunne, Maureen (2024). The Neurodiversity Edge: The Essential Guide to Embracing Autism, ADHD, Dyslexia, and Other Neurological Differences for Any Organization (1st ed.). Newark: John Wiley & Sons. ISBN 978-1-394-19928-0.
- ↑ "Autism Spectrum Disorder: Primary Care Principles". American Family Physician 94 (12): 972–979. December 2016. PMID 28075089.
- ↑ Iffland, Michelle; Livingstone, Nuala; Jorgensen, Mikaela; Hazell, Philip; Gillies, Donna (9 October 2023). Cochrane Developmental, Psychosocial and Learning Problems Group. ed. "Pharmacological intervention for irritability, aggression, and self-injury in autism spectrum disorder (ASD)" (in en). The Cochrane Database of Systematic Reviews 2023 (10). doi:10.1002/14651858.CD011769.pub2. PMID 37811711.
- ↑ 219.0 219.1 "Pharmacological and dietary-supplement treatments for autism spectrum disorder: a systematic review and network meta-analysis". Molecular Autism 13 (1). 2022. doi:10.1186/s13229-022-00488-4. PMID 35246237.
- ↑ 220.0 220.1 "Pharmacologic treatments for the behavioral symptoms associated with autism spectrum disorders across the lifespan". Dialogues in Clinical Neuroscience 14 (3): 263–279. September 2012. doi:10.31887/DCNS.2012.14.3/cdoyle. PMID 23226952.
- ↑ "Pharmacological treatment options for autism spectrum disorders in children and adolescents". Harvard Review of Psychiatry 16 (2): 97–112. 2008. doi:10.1080/10673220802075852. PMID 18415882.
- ↑ England, N. H. S.. "NHS England » Stopping over medication of people with a learning disability and autistic people (STOMP) and supporting treatment and appropriate medication in paediatrics (STAMP)" (in en-US). https://www.england.nhs.uk/learning-disabilities/improving-health/stomp-stamp/.
- ↑ "Systematic review and guide to management of core and psychiatric symptoms in youth with autism". Acta Psychiatrica Scandinavica 138 (5): 379–400. November 2018. doi:10.1111/acps.12918. PMID 29904907.
- ↑ Yu, Yanjie; Chaulagain, Ashmita; Pedersen, Sindre Andre; Lydersen, Stian; Leventhal, Bennett L.; Szatmari, Peter; Aleksic, Branko; Ozaki, Norio et al. (12 March 2020). "Pharmacotherapy of restricted/repetitive behavior in autism spectrum disorder: a systematic review and meta-analysis". BMC Psychiatry 20 (1): 121. doi:10.1186/s12888-020-2477-9. PMID 32164636.
- ↑ King, Bryan H.; Rynkiewicz, Agnieszka; Janas-Kozik, Matgorzata; Tyszkiewicz-Nwafor, Marta (2020). "Medications to Treat Co-Occurring Psychiatric Conditions in Autism Spectrum Disorder". in White, Susan Williams (in en). The Oxford handbook of autism and co-occurring psychiatric conditions. Oxford library of psychology. New York, NY: Oxford University Press. pp. 371–387. ISBN 978-0-19-091076-1.
- ↑ "Chelation for autism spectrum disorder (ASD)". The Cochrane Database of Systematic Reviews (5). May 2015. doi:10.1002/14651858.CD010766. PMID 26106752.
- ↑ "Complementary and alternative medicine treatments for children with autism spectrum disorders". Child and Adolescent Psychiatric Clinics of North America 17 (4): 803–20, ix. October 2008. doi:10.1016/j.chc.2008.06.004. PMID 18775371.
- ↑ "Deaths resulting from hypocalcemia after administration of edetate disodium: 2003-2005". Pediatrics 118 (2): e534–e536. August 2006. doi:10.1542/peds.2006-0858. PMID 16882789.
- ↑ Commissioner, Office of the (24 March 2020). "FDA warns consumers about the dangerous and potentially life threatening side effects of Miracle Mineral Solution" (in en). https://www.fda.gov/news-events/press-announcements/fda-warns-consumers-about-dangerous-and-potentially-life-threatening-side-effects-miracle-mineral.
- ↑ "Treatments that are not recommended for autism" (in en). 8 March 2023. https://www.nhs.uk/conditions/autism/autism-and-everyday-life/treatments-that-are-not-recommended-for-autism/.
- ↑ Sakulchit, Teeranai; Ladish, Chris; Goldman, Ran D. (June 2017). "Hyperbaric oxygen therapy for children with autism spectrum disorder". Canadian Family Physician 63 (6): 446–448. PMID 28615394.
- ↑ "Are therapeutic diets an emerging additional choice in autism spectrum disorder management?". World Journal of Pediatrics 14 (3): 215–223. June 2018. doi:10.1007/s12519-018-0164-4. PMID 29846886. "Current literature knowledge provides evidence that ketogenic and casein/gluten-free diet may have their own place in our reserve for the therapeutic management of specific subsets of children with autism. ... More clinical studies about the effect of gluten/caseinfree diet in these patients are available. However, available data arise from studies with small sample size and are still controversial. In general, despite encouraging data, no definite proof still exists. Under this view, the use of therapeutic diets in children with autism should be restricted to specific subgroups, such as children with autism and epilepsy or specific inborn errors of metabolism (ketogenic diet), children with known food intolerance/allergy or even children with food intolerance markers (gluten- and casein-free diet). Their implementation should always be guided by health care practitioners.".
- ↑ "Evidence of the gluten-free and casein-free diet in autism spectrum disorders: a systematic review". Journal of Child Neurology 29 (12): 1718–1727. December 2014. doi:10.1177/0883073814531330. PMID 24789114.
- ↑ "Gluten- and casein-free diets for autistic spectrum disorder". The Cochrane Database of Systematic Reviews (2). April 2008. doi:10.1002/14651858.CD003498.pub3. PMID 18425890. "Knivsberg 2002 "monitoring of the compliance with diet was not carried out" ... "several reports of children 'sneaking food' from siblings or classmates"".
- ↑ "Characterizing the Interplay Between Autism Spectrum Disorder and Comorbid Medical Conditions: An Integrative Review". Frontiers in Psychiatry 9. 2019. doi:10.3389/fpsyt.2018.00751. PMID 30733689.
- ↑ "Interventions to address health outcomes among autistic adults: A systematic review". Autism 24 (6): 1345–1359. August 2020. doi:10.1177/1362361320913664. PMID 32390461.
- ↑ "Music therapy for autistic people". The Cochrane Database of Systematic Reviews 2022 (5). May 2022. doi:10.1002/14651858.CD004381.pub4. PMID 35532041.
- ↑ Xiao, Ningkun; Bagayi, Vaishnavi; Yang, Dandan; Huang, Xinlin; Zhong, Lei; Kiselev, Sergey; Bolkov, Mikhail A.; Tuzankina, Irina A. et al. (2024). "Effectiveness of animal-assisted activities and therapies for autism spectrum disorder: a systematic review and meta-analysis". Frontiers in Veterinary Science 11. doi:10.3389/fvets.2024.1403527. PMID 38895710.
- ↑ Handbook of Autism and Pervasive Developmental Disorders: Volume Two: Assessment, Interventions, and Policy. 2 (4th ed.). Hoboken, New Jersey: John Wiley & Sons. 2014. p. 301. ISBN 978-1-118-28220-5. OCLC 946133861. https://books.google.com/books?id=4yzqAgAAQBAJ&pg=PA301. Retrieved 1 March 2019.
- ↑ Papadopoulos, Chris; Lodder, Annemarie; Constantinou, Georgina; Randhawa, Gurch (1 April 2019). "Systematic Review of the Relationship Between Autism Stigma and Informal Caregiver Mental Health" (in en). Journal of Autism and Developmental Disorders 49 (4): 1665–1685. doi:10.1007/s10803-018-3835-z. PMID 30569408.
- ↑ Tafolla, Maira; Singer, Hannah; Lord, Catherine (2025-05-07). "Autism Spectrum Disorder Across the Lifespan" (in en). Annual Review of Clinical Psychology 21: 193–220. doi:10.1146/annurev-clinpsy-081423-031110. ISSN 1548-5943. https://www.annualreviews.org/content/journals/10.1146/annurev-clinpsy-081423-031110.
- ↑ 242.0 242.1 Brignell, Amanda; Harwood, Rachael C; May, Tamara; Woolfenden, Susan; Montgomery, Alicia; Iorio, Alfonso; Williams, Katrina (2022-09-28). "Overall prognosis of preschool autism spectrum disorder diagnoses". Cochrane Database of Systematic Reviews 2022 (9). doi:10.1002/14651858.cd012749.pub2. ISSN 1465-1858. https://doi.org/10.1002/14651858.cd012749.pub2.
- ↑ "Asperger syndrome". European Child & Adolescent Psychiatry 18 (1): 2–11. June 2008. doi:10.1007/s00787-008-0701-0. PMID 18563474. https://hal.science/hal-00478064.
- ↑ Kapp, Steven K.; Ne'eman, Ari (2020). "Lobbying Autism's Diagnostic Revision in the DSM-5". in Kapp, Steven K. (in en). Autistic Community and the Neurodiversity Movement: Stories from the Frontline. Singapore: Springer. pp. 167–194. doi:10.1007/978-981-13-8437-0_13. ISBN 978-981-13-8437-0.
- ↑ "Parent and family impact of autism spectrum disorders: a review and proposed model for intervention evaluation". Clinical Child and Family Psychology Review 15 (3): 247–77. September 2012. doi:10.1007/s10567-012-0119-6. PMID 22869324.
- ↑ "Diagnosis and epidemiology of autism spectrum disorders". Canadian Journal of Psychiatry 48 (8): 517–525. September 2003. doi:10.1177/070674370304800803. PMID 14574827.
- ↑ 247.0 247.1 247.2 247.3 247.4 247.5 247.6 247.7 Newell, Victoria; Phillips, Lucy; Jones, Chris; Townsend, Ellen; Richards, Caroline; Cassidy, Sarah (15 March 2023). "A systematic review and meta-analysis of suicidality in autistic and possibly autistic people without co-occurring intellectual disability". Molecular Autism 14 (1): 12. doi:10.1186/s13229-023-00544-7. PMID 36922899.
- ↑ Trundle, Grace; Jones, Katy A.; Ropar, Danielle; Egan, Vincent (October 2023). "Prevalence of Victimisation in Autistic Individuals: A Systematic Review and Meta-Analysis". Trauma, Violence & Abuse 24 (4): 2282–2296. doi:10.1177/15248380221093689. PMID 35524162.
- ↑ Hudson, Chloe C; Hall, Layla; Harkness, Kate L (2019). "Prevalence of Depressive Disorders in Individuals with Autism Spectrum Disorder: a Meta-Analysis". Journal of Abnormal Child Psychology 47 (1): 165–175. doi:10.1007/s10802-018-0402-1. PMID 29497980.
- ↑ 250.0 250.1 O'Halloran, L.; Coey, P.; Wilson, C. (April 2022). "Suicidality in autistic youth: A systematic review and meta-analysis". Clinical Psychology Review 93. doi:10.1016/j.cpr.2022.102144. PMID 35290800.
- ↑ 251.0 251.1 Huntjens, Anne; Landlust, Annemiek; Wissenburg, Sophie; van der Gaag, Mark (March 2024). "The Prevalence of Suicidal Behavior in Autism Spectrum Disorder". Crisis 45 (2): 144–153. doi:10.1027/0227-5910/a000922. PMID 37668055.
- ↑ 252.0 252.1 Santomauro, Damian F.; Hedley, Darren; Sahin, Ensu; Brugha, Traolach S.; Naghavi, Mohsen; Vos, Theo; Whiteford, Harvey A.; Ferrari, Alize J. et al. (November 2024). "The global burden of suicide mortality among people on the autism spectrum: A systematic review, meta-analysis, and extension of estimates from the Global Burden of Disease Study 2021". Psychiatry Research 341. doi:10.1016/j.psychres.2024.116150. PMID 39197224.
- ↑ "New developments in autism". Psychiatric Clinics of North America 32 (1): 1–14. March 2009. doi:10.1016/j.psc.2008.10.004. PMID 19248913.
- ↑ Graham Holmes, Laura; Ames, Jennifer L.; Massolo, Maria L.; Nunez, Denise M.; Croen, Lisa A. (1 April 2022). "Improving the Sexual and Reproductive Health and Health Care of Autistic People". Pediatrics 149 (Supplement 4): e2020049437J. doi:10.1542/peds.2020-049437J. PMID 35363286.
- ↑ Caldwell-Harris, Catherine; Murphy, Caitlin Fox; Velazquez, Tessa; McNamara, Patrick (2011). "Religious Belief Systems of Persons with High Functioning Autism". Proceedings of the Annual Meeting of the Cognitive Science Society 33 (33). https://escholarship.org/uc/item/6zh3j3pr.
- ↑ "Autism". The Lancet 374 (9701): 1627–1638. November 2009. doi:10.1016/S0140-6736(09)61376-3. PMID 19819542. (Erratum: doi:10.1016/S0140-6736(11)61666-8)
- ↑ "Mental health of adults with autism spectrum disorders and intellectual disability". Current Opinion in Psychiatry 23 (5): 421–6. September 2010. doi:10.1097/YCO.0b013e32833cfc18. PMID 20613532.
- ↑ Helverschou, Sissel Berge; Bakken, Trine Lise; Martinsen, Harald (2011). "Psychiatric Disorders in People with Autism Spectrum Disorders: Phenomenology and Recognition". International Handbook of Autism and Pervasive Developmental Disorders. pp. 53–74. doi:10.1007/978-1-4419-8065-6_5. ISBN 978-1-4419-8064-9. OCLC 746203105.
- ↑ White, Susan W. (2020) (in en). The Oxford Handbook of Autism and Co-Occurring Psychiatric Conditions. Oxford Library of Psychology Series. Brenna Maddox, Carla Mazefsky (1st ed.). Oxford: Oxford University Press, Incorporated. p. 8. ISBN 978-0-19-091076-1.
- ↑ 260.0 260.1 260.2 260.3 Lai, Meng-Chuan; Kassee, Caroline; Besney, Richard; Bonato, Sarah; Hull, Laura; Mandy, William; Szatmari, Peter; Ameis, Stephanie H. (1 October 2019). "Prevalence of co-occurring mental health diagnoses in the autism population: a systematic review and meta-analysis" (in English). The Lancet Psychiatry 6 (10): 819–829. doi:10.1016/S2215-0366(19)30289-5. PMID 31447415.
- ↑ "Shared heritability of attention-deficit/hyperactivity disorder and autism spectrum disorder". European Child & Adolescent Psychiatry 19 (3): 281–95. March 2010. doi:10.1007/s00787-010-0092-x. PMID 20148275.
- ↑ Liu, Xian; Sun, Xin; Sun, Caihong; Zou, Mingyang; Chen, Yiru; Huang, Junping; Wu, Lijie; Chen, Wen-Xiong (2022). "Prevalence of epilepsy in autism spectrum disorders: A systematic review and meta-analysis". Autism: The International Journal of Research and Practice 26 (1): 33–50. doi:10.1177/13623613211045029. PMID 34510916.
- ↑ "The role of epilepsy and epileptiform EEGs in autism spectrum disorders". Pediatric Research 65 (6): 599–606. June 2009. doi:10.1203/PDR.0b013e31819e7168. PMID 19454962.
- ↑ Sala, G.; Hooley, M.; Attwood, T. (2019). "Autism and Intellectual Disability: A Systematic Review of Sexuality and Relationship Education". Sexuality and Disability 37 (3): 353–382. doi:10.1007/s11195-019-09577-4.
- ↑ "Anxiety in children and adolescents with autism spectrum disorders". Clinical Psychology Review 29 (3): 216–229. April 2009. doi:10.1016/j.cpr.2009.01.003. PMID 19223098.
- ↑ "Cluster A - Schizoid Personality Disorder and Substance Use Disorders". Integrated Treatment for Co-Occurring Disorders: Personality Disorders and Addiction. Routledge. 2008. pp. 31–32. ISBN 978-0-7890-3693-3. https://books.google.com/books?id=O5HY1xcfjEcC&pg=PA31.
- ↑ Yasuda, Yuka; Matsumoto, Junya; Miura, Kenichiro; Hasegawa, Naomi; Hashimoto, Ryota (2023). "Genetics of autism spectrum disorders and future direction". Journal of Human Genetics 68 (3): 193–197. doi:10.1038/s10038-022-01076-3. PMID 36038624.
- ↑ 268.0 268.1 "Serotonin as a link between the gut-brain-microbiome axis in autism spectrum disorders". Pharmacological Research 132: 1–6. June 2018. doi:10.1016/j.phrs.2018.03.020. PMID 29614380.
- ↑ McElhanon, Barbara O.; McCracken, Courtney; Karpen, Saul; Sharp, William G. (May 2014). "Gastrointestinal symptoms in autism spectrum disorder: a meta-analysis". Pediatrics 133 (5): 872–883. doi:10.1542/peds.2013-3995. PMID 24777214.
- ↑ 270.0 270.1 James, David M.; Davidson, Elizabeth A.; Yanes, Julio; Moshiree, Baharak; Dallman, Julia E. (2021). "The Gut-Brain-Microbiome Axis and Its Link to Autism: Emerging Insights and the Potential of Zebrafish Models". Frontiers in Cell and Developmental Biology 9. doi:10.3389/fcell.2021.662916. PMID 33937265.
- ↑ "The bowel and beyond: the enteric nervous system in neurological disorders". Nature Reviews. Gastroenterology & Hepatology 13 (9): 517–528. September 2016. doi:10.1038/nrgastro.2016.107. PMID 27435372. "immune dysregulation, GI inflammation, malfunction of the ANS, genetic and metabolic activity of the microbiome, and dietary metabolites may contribute to brain dysfunction and neuroinflammation depending upon individual genetic vulnerability".
- ↑ Sotelo-Orozco, Jennie; Hertz-Picciotto, Irva (2025-07-01). "The Association Between Gastrointestinal Issues and Psychometric Scores in Children with Autism Spectrum Disorder, Developmental Delays, Down Syndrome, and Typical Development". Journal of Autism and Developmental Disorders 55 (7): 2452–2462. doi:10.1007/s10803-024-06387-2. PMID 38739245.
- ↑ Research. "Autistic children more likely to experience persistent gastrointestinal problems" (in en). https://health.ucdavis.edu/research/news/headlines/autistic-children-more-likely-to-experience-persistent-stomach-problems/2025/09.
- ↑ Holingue, Calliope; Newill, Carol; Lee, Li-Ching; Pasricha, Pankaj J.; Daniele Fallin, M. (January 2018). "Gastrointestinal symptoms in autism spectrum disorder: A review of the literature on ascertainment and prevalence". Autism Research 11 (1): 24–36. doi:10.1002/aur.1854. PMID 28856868.
- ↑ "Sleep problems in autism spectrum disorders: prevalence, nature, & possible biopsychosocial aetiologies". Sleep Medicine Reviews 13 (6): 403–411. December 2009. doi:10.1016/j.smrv.2009.02.003. PMID 19398354.
- ↑ Kangarani-Farahani, Melika; Malik, Myrah Anum; Zwicker, Jill G. (1 May 2024). "Motor Impairments in Children with Autism Spectrum Disorder: A Systematic Review and Meta-analysis". Journal of Autism and Developmental Disorders 54 (5): 1977–1997. doi:10.1007/s10803-023-05948-1. PMID 36949273.
- ↑ Baeza-Velasco, Carolina; Vergne, Judith; Poli, Marianna; Kalisch, Larissa; Calati, Raffaella (1 August 2025). "Autism in the context of joint hypermobility, hypermobility spectrum disorders, and Ehlers–Danlos syndromes: A systematic review and prevalence meta-analyses". Autism 29 (8): 1939–1958. doi:10.1177/13623613251328059. PMID 40145613.
- ↑ "Gender dysphoria and autism spectrum disorder: A narrative review". International Review of Psychiatry 28 (1): 70–80. 2016. doi:10.3109/09540261.2015.1111199. PMID 26753812.
- ↑ "Gender Dysphoria and Autism Spectrum Disorder: A Systematic Review of the Literature". Sexual Medicine Reviews 4 (1): 3–14. January 2016. doi:10.1016/j.sxmr.2015.10.003. PMID 27872002. https://dspace.lboro.ac.uk/2134/20811.
- ↑ "Epidemiology of pervasive developmental disorders". Pediatric Research 65 (6): 591–598. June 2009. doi:10.1203/PDR.0b013e31819e7203. PMID 19218885.
- ↑ "The epidemiology of autistic spectrum disorders: is the prevalence rising?". Developmental Disabilities Research Reviews 8 (3): 151–161. 2002. doi:10.1002/mrdd.10029. PMID 12216059.
- ↑ "Three Reasons Not to Believe in an Autism Epidemic". Current Directions in Psychological Science 14 (2): 55–58. April 2005. doi:10.1111/j.0963-7214.2005.00334.x. PMID 25404790.
- ↑ Fletcher-Watson, Sue; Happé, Francesca (2019) (in en). Autism: A New Introduction to Psychological Theory and Current Debate (2nd ed.). Milton: Taylor & Francis Group. p. 42. ISBN 978-1-138-10612-3.
- ↑ "Incidence of autism spectrum disorders: changes over time and their meaning". Acta Paediatrica 94 (1): 2–15. January 2005. doi:10.1111/j.1651-2227.2005.tb01779.x. PMID 15858952.
- ↑ 285.0 285.1 CDC (18 April 2025). "Data and Statistics on Autism Spectrum Disorder" (in en-us). https://www.cdc.gov/autism/data-research/index.html.
- ↑ "The epidemiology of autism spectrum disorders". Annual Review of Public Health 28 (1): 235–58. 2007. doi:10.1146/annurev.publhealth.28.021406.144007. PMID 17367287. Bibcode: 2007ARPH...28..235N.
- ↑ "Autism risk factors: genes, environment, and gene-environment interactions". Dialogues in Clinical Neuroscience 14 (3): 281–292. September 2012. doi:10.31887/DCNS.2012.14.3/pchaste. PMID 23226953.
- ↑ Lockwood Estrin, Georgia; Milner, Victoria; Spain, Debbie; Happé, Francesca; Colvert, Emma (1 December 2021). "Barriers to Autism Spectrum Disorder Diagnosis for Young Women and Girls: a Systematic Review". Review Journal of Autism and Developmental Disorders 8 (4): 454–470. doi:10.1007/s40489-020-00225-8. PMID 34868805.
- ↑ Evans, Bonnie (2013). "How Autism became Autism". History of the Human Sciences 26 (3): 3–31. doi:10.1177/0952695113484320. PMID 24014081.
- ↑ "Autism | Definition, Symptoms, Neuropathology, & Diagnosis | Britannica" (in en). 21 June 2025. https://www.britannica.com/science/autism. "The term autism (from the Greek autos, meaning "self") was coined in 1911 by Swiss psychiatrist Eugen Bleuler, who used it to describe withdrawal into one's inner world, a phenomenon he observed in individuals with schizophrenia."
- ↑ Vicedo, Marga (17 January 2024). "Moving beyond the search for the first discoverer of autism". Frontiers in Psychiatry 15: 02. doi:10.3389/fpsyt.2024.1266486. PMID 38299189.
- ↑ Sher, David Ariel; Gibson, Jenny L. (1 March 2023). "Pioneering, prodigious and perspicacious: Grunya Efimovna Sukhareva's life and contribution to conceptualising autism and schizophrenia". European Child & Adolescent Psychiatry 32 (3): 475–490. doi:10.1007/s00787-021-01875-7. PMID 34562153.
- ↑ Simmonds, Charlotte (2019). G. E. Sukhareva's place in the history of autism research: Context, reception, translation (Thesis). doi:10.26686/wgtn.17136701.
- ↑ 294.0 294.1 "Greta Thunberg: 'I really see the value of friendship. Apart from the climate, almost nothing else matters'" (in en). The Guardian. 25 September 2021. https://www.theguardian.com/environment/ng-interactive/2021/sep/25/greta-thunberg-i-really-see-the-value-of-friendship-apart-from-the-climate-almost-nothing-else-matters.
- ↑ "Autism Movement Seeks Acceptance, Not Cures". NPR. 26 June 2006. https://www.npr.org/templates/story/story.php?storyId=5488463.
- ↑ "Autistic and proud of it". New Scientist (Reed Elsevier). https://www.newscientist.com/article/mg18625041-500-autistic-and-proud-of-it/. Retrieved 10 November 2015.
- ↑ 297.0 297.1 297.2 297.3 Solomon, Andrew (25 May 2008). "The autism rights movement". New York Magazine. https://nymag.com/news/features/47225/.
- ↑ The Economic World. New York city: Chronicle Publishing Company. 1917. p. 366.
- ↑ 299.0 299.1 299.2 299.3 "Fieldwork on another planet: social science perspectives on the autism spectrum". BioSocieties 3 (3): 325–341. 2008. doi:10.1017/S1745855208006236.
- ↑ "Results and Analysis of the Autistic Not Weird 2022 Autism Survey - Autistic Not Weird" (in en-GB). 23 March 2022. https://autisticnotweird.com/autismsurvey/.
- ↑ "World Autism Awareness Day, 2 April". United Nations. https://www.un.org/en/events/autismday/.
- ↑ "Autistic Pride Day 2015: A Message to the Autistic Community". 18 June 2015. http://autisticadvocacy.org/2015/06/autistic-pride-day-2015-a-message-to-the-autistic-community/.
- ↑ "Autism Sunday – Home". 2010. http://www.autismsunday.co.uk/.
- ↑ "About Autreat". Autreat.com. 2013. http://www.autreat.com/autreat.html.
- ↑ Silberman, Steve (6 May 2019). "Greta Thunberg became a climate activist not in spite of her autism, but because of it" (in en-US). https://www.vox.com/first-person/2019/5/6/18531551/greta-thunberg-autism-aspergers.
- ↑ Ryan, Maggie (12 April 2024). "These 12 Celebrities With Autism Are Opening Up About Life on the Spectrum" (in en-US). https://www.sheknows.com/health-and-wellness/slideshow/2992980/celebrities-with-autism/.
- ↑ Gates, Bill (25 January 2025). "Essay | Exclusive | Bill Gates: I Coded While I Hiked as a Teenager. Was I on the Spectrum? Probably." (in en-US). https://www.wsj.com/arts-culture/bill-gates-memoir-410d7ff5.
- ↑ 308.0 308.1 "Översyn av körkortskrav vid autism och adhd" (in sv). https://www.autism.se/aktuellt/oversyn-av-korkortskrav-vid-autism-och-adhd/.
- ↑ "Personer med ADHD och autism nekades möjlighet att prövas för militärtjänst" (in sv). https://www.do.se/rattsfall-beslut-lagar-stodmaterial/tvister-domar-tillsynsbeslut/ovrigt/personer-med-adhd-och-autism-nekades-mojlighet-att-provas-for-militartjanst.
- ↑ 310.0 310.1 Rowsell, Juliette (6 December 2023). "Police officer rejected from firearms training because of autism diagnosis was discriminated against, tribunal rules" (in en). https://www.peoplemanagement.co.uk/article/1850180.
- ↑ Donvan, John etc.. "People with autism navigate roadblocks to serving in the military" (in en). https://abcnews.go.com/US/people-autism-navigate-roadblocks-serving-military/story?id=109748037.
- ↑ 312.0 312.1 312.2 Cleary, Michelle; West, Sancia; Kornhaber, Rachel; Hungerford, Catherine (2 September 2023). "Autism, Discrimination and Masking: Disrupting a Recipe for Trauma". Issues in Mental Health Nursing 44 (9): 799–808. doi:10.1080/01612840.2023.2239916. PMID 37616302.
- ↑ "Annual Research Review: Shifting from 'normal science' to neurodiversity in autism science". Journal of Child Psychology and Psychiatry, and Allied Disciplines 63 (4): 381–396. April 2022. doi:10.1111/jcpp.13534. OCLC 01307942. PMID 34730840.
- ↑ "'Surplus suffering': differences between organizational understandings of Asperger's syndrome and those people who claim the 'disorder'". Disability & Society 22 (7): 761–76. 2007. doi:10.1080/09687590701659618.
- ↑ Baron-Cohen, Simon (August 2002). "Is Asperger Syndrome Necessarily Viewed as a Disability?". Focus on Autism and Other Developmental Disabilities 17 (3): 186–191. doi:10.1177/10883576020170030801.
- ↑ Baron-Cohen, Simon (September 2000). "Is Asperger syndrome/high-functioning autism necessarily a disability?". Development and Psychopathology 12 (3): 489–500. doi:10.1017/S0954579400003126. PMID 11014749.
- ↑ 317.0 317.1 "Autism spectrum disorder: difference or disability?" (in en). The Lancet Neurology 15 (11): 1126. 1 October 2016. doi:10.1016/S1474-4422(16)30002-3.
- ↑ "A medical condition or just a difference? The question roils autism community." (in en-US). The Washington Post. https://www.washingtonpost.com/national/health-science/a-medical-condition-or-just-a-difference-the-question-roils-autism-community/2019/05/03/87e26f7e-6845-11e9-8985-4cf30147bdca_story.html.
- ↑ 319.0 319.1 319.2 319.3 Jaarsma, Pier; Welin, Stellan (1 March 2012). "Autism as a Natural Human Variation: Reflections on the Claims of the Neurodiversity Movement" (in en). Health Care Analysis 20 (1): 20–30. doi:10.1007/s10728-011-0169-9. PMID 21311979. http://urn.kb.se/resolve?urn=urn:nbn:se:liu:diva-72172.
- ↑ "Second edition overview | Assessment and Diagnosis Guideline" (in en). https://www.autismcrc.com.au/best-practice/assessment-and-diagnosis/second-edition.
- ↑ "Autism" (in EN). 27 February 2025. https://www.nih.gov/nih-style-guide/autism.
- ↑ Hill, Amelia (31 July 2023). "Autism could be seen as part of personality for some diagnosed, experts say". The Guardian. https://www.theguardian.com/society/2023/jul/31/autism-could-be-seen-as-part-of-personality-for-some-diagnosed-experts-say.
- ↑ 323.0 323.1 "Should Autism Be Cured or Is "Curing" Offensive?". 10 July 2016. https://bigthink.com/paul-ratner/should-autism-be-cured-or-is-curing-offfensive.
- ↑ "Neurodiversity". Contexts 11 (3): 12–13. August 2012. doi:10.1177/1536504212456175.
- ↑ "Biocertification and Neurodiversity the Role and Implications of Self-Diagnosis in Autistic Communities". Neuroethics 9: 23–36. April 2016. doi:10.1007/s12152-016-9247-x.
Sources
- "Neurodevelopmental Disorders". Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR). Washington, DC: American Psychiatric Association. 18 March 2022. ISBN 978-0-89042-577-0.
- "6A02 Autism spectrum disorder". International Classification of Diseases 11th Revision (ICD-11). World Health Organization. February 2022. 6A02. https://icd.who.int/browse11/l-m/en#/http://id.who.int/icd/entity/437815624. Retrieved 14 May 2022.
Further reading
- Grandin, Temple (2013). The Autistic Brain: Thinking Across the Spectrum. Mariner Books. ISBN 978-0-544-22773-6.
- Silberman, Steve (2015). NeuroTribes: The Legacy of Autism and the Future of Neurodiversity. Avery. ISBN 978-1-58333-467-6.
- Prizant, Barry M; Fields-Meyer, Tom (2015). Uniquely Human: A Different Way of Seeing Autism. Simon & Schuster. ISBN 978-1-4767-7624-8.
- Baron-Cohen, Simon (2020). The Pattern Seekers: How Autism Drives Human Invention. Basic Books. ISBN 978-1-5416-4713-8.
- Higashida, Naoki (2013). The Reason I Jump: The Inner Voice of a Thirteen-Year-Old Boy with Autism. Random House. ISBN 978-0-8129-8515-3.
- Marble, John (2025). Autism For Dummies. For Dummies. ISBN 978-1-394-30100-3.
- Price, Devon (2022). Unmasking Autism: Discovering the New Faces of Neurodiversity. Harmony. ISBN 978-0-593-23523-2.
- Garcia, Eric (2021). We're Not Broken: Changing the Autism Conversation. Mariner Books. ISBN 978-0-358-69714-5.
- Ballou, Emily Paige (2021). Sincerely, Your Autistic Child: What People on the Autism Spectrum Wish Their Parents Knew About Growing Up, Acceptance, and Identity. Beacon Press. ISBN 978-0-8070-2568-0.
- Pang, Camilla (2020). Explaining Humans: What Science Can Teach Us About Life, Love and Relationships. Penguin Books. ISBN 978-0-241-40960-2.
External links
| Library resources about Autism |
| Classification | |
|---|---|
| External resources |
Template:Nonverbal communication
 |
 KSF
KSF