Delirium tremens
Topic: Medicine
 From HandWiki - Reading time: 18 min
From HandWiki - Reading time: 18 min
| Delirium tremens | |
|---|---|
| Other names | Alcohol-induced delirium |
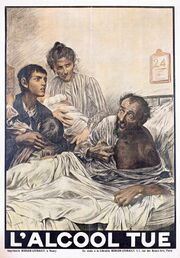 | |
| An alcoholic man with delirium tremens on his deathbed, surrounded by his concerned family. The text L'alcool tue means "Alcohol kills" in French. | |
| Specialty | Psychiatry, critical care medicine |
| Symptoms | Hallucinations, confusion, shaking, shivering, irregular heart rate, sweating[1][2][3] |
| Complications | Very high body temperature, seizures[2] |
| Usual onset | Rapid, 48-72 hours after last drink[2] |
| Duration | 1–8 days[2] |
| Causes | Abrupt cessation of alcohol intake in a state of alcohol dependence |
| Differential diagnosis | Benzodiazepine withdrawal syndrome, barbiturate withdrawal[4] |
| Treatment | Intensive care unit, benzodiazepines, thiamine[2] |
| Prognosis | Risk of death ~2% (treatment), 25% (no treatment)[5] |
| Frequency | ~4% of those withdrawing from alcohol[2] |
Delirium tremens (DTs; lit. mental disturbance with shaking) is a rapid onset of confusion caused by withdrawal from alcohol.[2] DT typically occurs 48–72 hours after the last use of alcohol and symptoms last 1–8 days.[2][6] Typical symptoms include nightmares, confusion, disorientation, heavy sweating, elevated heart rate, and elevated blood pressure.[6][1] Visual, auditory, and tactile hallucinations are also common.[2] DT can be fatal especially without treatment. Occasionally, a very high body temperature or seizures (colloquially known as "rum fits")[7][8] may result in death.[2] Other causes of death include respiratory failure and cardiac arrhythmias.[2]
Delirium tremens typically occurs only in people with a high intake of alcohol for prolonged periods of time, followed by sharply reduced intake.[9] A similar syndrome may occur with benzodiazepine and barbiturate withdrawal, however the term delirium tremens is reserved for alcohol withdrawal. In a person with delirium tremens, it is important to rule out other associated problems such as electrolyte abnormalities, pancreatitis, and alcoholic hepatitis.[2]
Prevention is by treating withdrawal symptoms using similarly acting compounds to taper off the use of the precipitating substance in a controlled fashion.[2] If delirium tremens occurs, aggressive treatment with benzodiazepines improves outcomes.[2] Treatment in a quiet intensive care unit with sufficient light is often recommended to re-orient the patient.[2] Benzodiazepines are the medication of choice with short acting compounds including lorazepam and oxazepam commonly used, which bypass the liver.[9] These medications are typically given in response to the patient's symptoms, rather than at regular intervals.[10] Nonbenzodiazepines are often used as adjuncts to manage the sleep disturbance associated with condition. The antipsychotic haloperidol may also be used[2] in order to combat the overactivity and possible excitotoxicity caused by the withdrawal from a GABA-ergic substance. Antipsychotics, however, are not used alone as they may increase the risk of seizure.[11] Thiamine (vitamin B1) is recommended to be given intramuscularly,[2] because long-term high alcohol intake and the associated nutritional deficit leads to a thiamine deficiency, which sometimes cannot be rectified by supplement pills alone.
Mortality without treatment historically has been between 15% and 40%.[5] With improvements in treatment over the years, currently death occurs in about 1% to 4% of cases.[2]
About half of people with alcoholism will develop withdrawal symptoms upon reducing their use.[2] Of these, 3% to 5% develop DTs or have seizures.[2]
The name delirium tremens was first used in 1813; however, the symptoms were well described since the 1700s.[9] The word "delirium" is Latin for "going off the furrow", a plowing metaphor for disordered thinking.[5] It is also called the shaking frenzy and Saunders-Sutton syndrome.[5] There are numerous nicknames for the condition, including "the DTs" and "seeing pink elephants".
Signs and symptoms
The main symptoms of delirium tremens are nightmares, agitation, global confusion, disorientation, visual and auditory hallucinations,[12] tactile hallucinations, seizures, fever, high heart rate, high blood pressure, heavy sweating, and other signs of autonomic hyperactivity. These symptoms typically develop 48–72 hours after the last use of alcohol and symptoms typically last 1–8 days.[6]
The symptoms of alcohol withdrawal are often characterized using the Clinical Institute Withdrawal Assessment for Alcohol tool otherwise known as "CIWA Protocol" which includes symptoms like nausea, sweating, tremors, headache, agitation, tactile disturbances, and changes in vision or hearing. A score is given based on the severity of symptoms. A score of greater than 15 increases the likelihood of developing delirium. A systolic blood pressure of greater than 150 mmHg and pulse greater than 100 beats per minute are also signs of severe withdrawals.[13][14]
These symptoms are characteristically worse at night.[15] For example, in Finnish, this nightlike condition is called liskojen yö, lit. the night of the lizards, for its sweatiness, general unease, and hallucinations tending towards the unseemly and frightening. Although this term is not medically recognized, it describes visual and tactile hallucinations often including animals and insects that are common in DT.
In general, DT is considered the most severe manifestation of withdrawal from alcohol and can occur between the second and tenth days after the last drink.[12] It often overcomes the patient by surprise, because a brief period of uneventful sobriety of 1–2 days tends to precede it.

Other common symptoms include intense perceptual disturbance such as visions or feelings of insects, snakes, or rats. These may be hallucinations or illusions related to the environment, e.g., patterns on the wallpaper or in the peripheral vision that the patient falsely perceives as a resemblance to the morphology of an insect, and are also associated with tactile hallucinations such as sensations of something crawling on the subject—a phenomenon known as formication. Delirium tremens usually includes feelings of "impending doom". Anxiety and expecting imminent death are common DT symptoms.[16]
DT can sometimes be associated with severe, coarse tremors of the extremities mostly in the hands.[2] Secondary symptoms include anxiety, panic attacks, and paranoia.
DT should be distinguished from alcoholic hallucinosis, the latter of which occurs in approximately 20% of hospitalized alcoholics and does not carry a significant risk of mortality. In contrast, DT occurs in 3-5% of those hospitalized with alcohol withdrawal and has a 1-4% mortality rate. In the past, death rates reached up to 15-35% without treatment, but treatment has significantly improved survival.[13] The most common conditions leading to death in patients with DTs are respiratory failure and cardiac arrhythmias.[17]
Causes
There is no exact amount of alcohol that precipitates delirium tremens, but it is most common after abrupt stopping after heavy, prolonged periods of drinking. More than 20 drinks per day increases the risk of DT; however, it can occur with fewer drinks as well.[18] Withdrawal from other drugs like benzodiazepines or barbiturates may cause similar symptoms, but the term delirium tremens is reserved for alcohol withdrawal.[2]
Pathophysiology
Delirium tremens is a component of alcohol withdrawal hypothesized to be the result of compensatory changes in response to chronic heavy alcohol use. Alcohol binds to and activates GABA, causing depression of the central nervous system and sedation. This results in inhibition of neurons projecting into the nucleus accumbens, as well as inhibiting NMDA receptors. This combined with desensitization of alpha-2 adrenergic receptors, results in upregulation of these systems in chronic alcohol use.[19]
When alcohol use ceases, the unregulated mechanisms result in hyperexcitability of neurons as natural GABAergic systems are down-regulated and excitatory glutamatergic systems are upregulated. This combined with increased noradrenergic activity results in the symptoms of delirium tremens including seizures, tremors, anxiety, confusion, and hallucinations.[19]
Diagnosis
Diagnosis is mainly based on symptoms. According to the DSM-5, alcohol withdrawal is diagnosed after a cessation or reduction in heavy, prolonged alcohol use followed by the development of at least two of the following symptoms: autonomic hyperactivity (elevated heart rate, elevated blood pressure, etc.), increased hand tremor, insomnia, nausea/vomiting, hallucinations or illusions, psychomotor agitation, anxiety, and generalized seizures.[20] Scoring criteria including CIWA is useful to anticipate withdrawal and to estimate severity, but it is not used for diagnosis.[14] In a person with delirium tremens, it is important to rule out other associated problems, such as electrolyte abnormalities, pancreatitis, and alcoholic hepatitis.[2]
Treatment
The treatment of choice for delirium tremens is benzodiazepines. High doses may be necessary to prevent death.[21] The preferred treatment is giving these medications in response to the patient's symptoms, rather than at scheduled intervals.[10] Short acting benzodiazepines including lorazepam and oxazepam are commonly used as they are not processed by the liver, which can be dangerous in patients with alcoholism with significant liver disease.
In some cases, antipsychotics such as haloperidol may also be used to further control symptoms like agitation and confusion. Antipsychotics should never be used alone in delirium tremens as they may increase the risk of seizures.[11] Older drugs such as paraldehyde and clomethiazole were formerly the traditional treatment but have now largely been superseded by benzodiazepines.[22]
A number of hospitals are now switching to barbiturates, namely Phenobarbital, over treatment with Benzodiazepines. In a quality improvement study comparing outcomes before (154 patients) and after (100 patients) implementation, 67% of postimplementation patients were treated using the phenobarbital order set, which was associated with faster symptom resolution (4.2- to 5.0-point Clinical Institute Withdrawal Assessment of Alcohol Scale Revised score reduction from 24-96 hours), reduced AWS treatment duration (30.1 hours), shorter hospital stay (2.2 days), and no increase in adverse events.[23]
It can also be helpful to provide a well lit room to reorient the patient and reduce confusion.[24]
Alcoholic beverages were given in the past,[25] but this practice is no longer supported.[26][27]
High doses of thiamine, often by the intravenous route, is also recommended to prevent Wernicke's encephalopathy, as[2] low thiamine levels are very common in heavy alcohol use.
Society and culture
Film and TV
In the 1945 film The Lost Weekend, Ray Milland won the Academy Award for Best Actor for his depiction of a character who experiences delirium tremens after being hospitalized, hallucinating that he saw a bat fly in and eat a mouse poking through a wall.[28][29][30]
The M*A*S*H TV series episode "Bottoms Up" (season 9, episode 15, aired on March 2, 1981) featured a side story about a nurse (Capt. Helen Whitfield) who was found to be drinking heavily off-duty. By the culmination of the episode, after a confrontation by Maj. Margaret Houlihan, the character swears off alcohol and presumably quits immediately. At mealtime, roughly 48 hours later, Whitfield becomes hysterical upon being served food in the mess tent, claiming that things are crawling onto her from it. Margaret and Col. Sherman Potter subdue her. Potter, having recognized the symptoms of delirium tremens orders 5 ml of paraldehyde from a witnessing nurse.
During the filming of the 1975 film Monty Python and the Holy Grail, Graham Chapman developed delirium tremens due to the lack of alcohol on the set. It was particularly bad during the filming of the bridge of death scene where Chapman was visibly shaking, sweating and could not cross the bridge. His fellow Pythons were astonished as Chapman was an accomplished mountaineer.[31]
In the 1995 film Leaving Las Vegas, Nicolas Cage plays a suicidal alcoholic who rids himself of all his possessions and travels to Las Vegas to drink himself to death. During his travels, he experiences delirium tremens on a couch after waking up from a binge and crawls in pain to the refrigerator for more vodka. Cage's performance as Ben Sanderson in the film won the Academy Award for Best Actor in 1996.
Literature

French writer Émile Zola's novel The Drinking Den (L'Assommoir) includes a character – Coupeau, the main character Gervaise's husband – who has delirium tremens by the end of the book.
In English Writer Mona Caird's feminist novel The Daughters of Danaus (1894), "[a]s for taking enfeeblement as a natural dispensation", the character Hadria "would as soon regard delirium tremens in that light."
American writer Mark Twain describes an episode of delirium tremens in his book The Adventures of Huckleberry Finn (1884). In chapter 6, Huck states about his father, "After supper pap took the jug, and said he had enough whisky there for two drunks and one delirium tremens. That was always his word." Subsequently, Pap Finn runs around with hallucinations of snakes and chases Huck around their cabin with a knife in an attempt to kill him, thinking Huck is the "Angel of Death".
One of the characters in Joseph Conrad's novel Lord Jim experiences "DTs of the worst kind" with symptoms that include seeing millions of pink frogs.
English author M. R. James mentions delirium tremens in his 1904 ghost story "'Oh, Whistle, and I'll Come to You, My Lad'". Professor Parkins while staying at the Globe Inn when in coastal Burnstow to "improve his game" of golf, despite being "a convinced disbeliever in what is called the 'supernatural'", when face to face with an entity in his "double-bed room" during the story's climax, is heard "uttering cry upon cry at the utmost pitch of his voice" though later "was somehow cleared of the ready suspicion of delirium tremens".
American writer Jack Kerouac details his experiences with delirium tremens in his book Big Sur.[32]
English author George Eliot provides a case involving delirium tremens in her novel Middlemarch (1871–72). Alcoholic scoundrel John Raffles, both an abusive stepfather of Joshua Riggs and blackmailing nemesis of financier Nicholas Bulstrode, dies, whose "death was due to delirium tremens" while at Peter Featherstone's Stone Court property. Housekeeper Mrs. Abel provides Raffles' final night of care per Bulstrode's instruction whose directions given to Abel stand adverse to Tertius Lydgate's orders.
Music
Irish singer-songwriter Christy Moore has a song on his 1985 album, Ordinary Man, called "Delirium Tremens" which is a satirical song, directed towards the leaders in Irish politics and culture. Some of the people mentioned in the song include Charles Haughey (former Fianna Fáil leader), Ruairi Quinn (at the time a Labour TD, later the party leader), Dick Spring (former Labour Party leader) and Roger Casement (who was captured bringing German guns to Ireland for the 1916 Easter Rising). English band Brotherly has a song called "DTs" on their album One Sweet Life. Fito Páez and Joaquín Sabina have a song called "Delirium Tremens" on their 1998 collaborative album, ''Enemigos Íntimos''.
Russian composer Modest Mussorgsky (1839-1881) died of delirium tremens.[33]
Popular culture

Nicknames for delirium tremens include "the DTs", "the shakes", "the oopizootics", "barrel-fever", "the blue horrors", "the rat's", "bottleache", "bats", "the drunken horrors", "seeing pink elephants", "gallon distemper", "quart mania", "janky jerks", "heebie jeebies", "pink spiders", and "riding the ghost train",[34] as well as "ork orks", "the zoots", "the 750 itch", and "pint paralysis". Another nickname is "the Brooklyn Boys", found in Eugene O'Neill's one-act play Hughie set in Times Square in the 1920s.[35] Delirium tremens was also given an alternate medical definition since at least the 1840s, being known as mania a potu, which translates to 'mania from drink'.[36]
The Belgian beer Delirium Tremens, introduced in 1988, is a direct reference and also uses a pink elephant as its logo to highlight one of the symptoms of delirium tremens.[37][38]
See also
- Alcohol dementia
- Alcohol detoxification
- Delusional parasitosis
- Excited delirium
- On the wagon
References
- ↑ 1.0 1.1 Healy, David (December 3, 2008). Psychiatric Drugs Explained. Elsevier Health Sciences. p. 237. ISBN 978-0-7020-2997-4. https://books.google.com/books?id=ikTJViYMPIEC&pg=PA237.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 Schuckit, MA (November 27, 2014). "Recognition and management of withdrawal delirium (delirium tremens).". The New England Journal of Medicine 371 (22): 2109–13. doi:10.1056/NEJMra1407298. PMID 25427113. http://www.escholarship.org/uc/item/08b9z9th.
- ↑ Royuela Rico, Ángel (February 2024). "First Description of Delirium Tremens was Made by Diego de Torres Villarroel in 1737". Actas Españolas de Psiquiatría 52 (1): 70–71. ISSN 1578-2735. PMID 38454891.
- ↑ Posner, Jerome B. (2007). Plum and Posner's Diagnosis of Stupor and Coma. (4 ed.). Oxford: Oxford University Press, USA. p. 283. ISBN 978-0-19-804336-2. https://books.google.com/books?id=Otivdh2ZoVwC&pg=PA283.
- ↑ 5.0 5.1 5.2 5.3 Blom, Jan Dirk (2010). A dictionary of hallucinations (. ed.). New York: Springer. p. 136. ISBN 978-1-4419-1223-7. https://books.google.com/books?id=KJtQptBcZloC&pg=PA136.
- ↑ 6.0 6.1 6.2 Kaye, Alan D; Staser, Amanda N; Mccollins, Tiombee S; Zheng, Jackson; Berry, Fouad A; Burroughs, Caroline R; Heisler, Michael; Mouhaffel, Aya et al. (April 4, 2024). "Delirium Tremens: A Review of Clinical Studies" (in en). Cureus 16 (4). doi:10.7759/cureus.57601. ISSN 2168-8184. PMID 38707114.
- ↑ "rum fits". Farlex, Inc.. https://medical-dictionary.thefreedictionary.com/rum+fits.
- ↑ Rhinehart, John W. (1961). "Factors determining "rum fits"" (in en). American Journal of Psychiatry 118 (3): 251–252. doi:10.1176/ajp.118.3.251. ISSN 0002-953X. PMID 13741146. https://ajp.psychiatryonline.org/doi/10.1176/ajp.118.3.251. Retrieved February 1, 2023.
- ↑ 9.0 9.1 9.2 Stern, TA; Gross, AF; Stern, TW; Nejad, SH; Maldonado, JR (2010). "Current approaches to the recognition and treatment of alcohol withdrawal and delirium tremens: "old wine in new bottles" or "new wine in old bottles"". Primary Care Companion to the Journal of Clinical Psychiatry 12 (3). doi:10.4088/PCC.10r00991ecr. PMID 20944765.
- ↑ 10.0 10.1 Haber, Paul S. (January 16, 2025). Ropper, Allan H.. ed. "Identification and Treatment of Alcohol Use Disorder" (in en). New England Journal of Medicine 392 (3): 258–266. doi:10.1056/NEJMra2306511. ISSN 0028-4793. PMID 39813644. http://www.nejm.org/doi/10.1056/NEJMra2306511.
- ↑ 11.0 11.1 Alvanzo, AnikaExpression error: Unrecognized word "et". (23 January 2020). Clinical Practice Guideline on Alcohol Withdrawal Management (Report). American Society of Addiction Medicine. https://downloads.asam.org/sitefinity-production-blobs/docs/default-source/quality-science/the_asam_clinical_practice_guideline_on_alcohol-1.pdf?sfvrsn=ba255c2_0.
- ↑ 12.0 12.1 Delirium Tremens (DTs)~clinical at eMedicine
- ↑ 13.0 13.1 Schuckit, Marc A. (November 27, 2014). Longo, Dan L.. ed. "Recognition and Management of Withdrawal Delirium (Delirium Tremens)" (in en). New England Journal of Medicine 371 (22): 2109–2113. doi:10.1056/NEJMra1407298. ISSN 0028-4793. PMID 25427113. http://www.nejm.org/doi/10.1056/NEJMra1407298.
- ↑ 14.0 14.1 Williams, D. (March 1, 2001). "A comparison of rating scales for the alcohol-withdrawal syndrome". Alcohol and Alcoholism 36 (2): 104–108. doi:10.1093/alcalc/36.2.104. PMID 11259205. https://academic.oup.com/alcalc/article-lookup/doi/10.1093/alcalc/36.2.104.
- ↑ Gelder et al, 2005 p188 Psychiatry 3rd Ed. Oxford: New York.
- ↑ "Delirium tremens: MedlinePlus Medical Encyclopedia" (in en). https://medlineplus.gov/ency/article/000766.htm.
- ↑ Delirium Tremens (DTs): Prognosis at eMedicine
- ↑ Sørensen, H. J.; Holst, C.; Knop, J.; Mortensen, E. L.; Tolstrup, J. S.; Becker, U. (2019). "Alcohol and delirium tremens: effects of average number of drinks per day and beverage type" (in en). Acta Psychiatrica Scandinavica 139 (6): 518–525. doi:10.1111/acps.13006. ISSN 1600-0447. PMID 30697683. https://onlinelibrary.wiley.com/doi/abs/10.1111/acps.13006.
- ↑ 19.0 19.1 Stern, Theodore A.; Gross, Anne F.; Stern, Thomas W.; Nejad, Shamim H.; Maldonado, Jose R. (January 1, 2010). "Current Approaches to the Recognition and Treatment of Alcohol Withdrawal and Delirium Tremens: "Old Wine in New Bottles" or "New Wine in Old Bottles"". Primary Care Companion to the Journal of Clinical Psychiatry 12 (3). doi:10.4088/PCC.10r00991ecr. ISSN 1523-5998. PMID 20944765.
- ↑ Jeste, Dilip V.Expression error: Unrecognized word "et". (2022). Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
- ↑ "Prolonged delirium tremens requiring massive doses of medication". J Am Board Fam Pract 6 (5): 502–4. 1993. PMID 8213241.
- ↑ Grover, Sandeep; Ghosh, Abhishek (December 2018). "Delirium Tremens: Assessment and Management" (in en). Journal of Clinical and Experimental Hepatology 8 (4): 460–470. doi:10.1016/j.jceh.2018.04.012. PMID 30564004.
- ↑ Wolpaw, Benjamin J.; Oren, Hannah; Quinnan-Hostein, Laura; Bradley, Katharine A.; Johnson, Nicholas J.; Hallgren, Kevin A.; Gupta, Ayushi; Kim, H. Nina et al. (2025-08-01). "Hospital-Wide Implementation, Clinical Outcomes, and Safety of Phenobarbital for Alcohol Withdrawal". JAMA Network Open 8 (8): e2528694. doi:10.1001/jamanetworkopen.2025.28694. ISSN 2574-3805. PMID 40853658.
 This article incorporates text available under the CC BY 4.0 license.
This article incorporates text available under the CC BY 4.0 license.
- ↑ NCLEX-RN in a Flash. Jones & Bartlett Learning. 2009. ISBN 978-0-7637-6197-4. https://books.google.com/books?id=3xbmHrT89C8C&pg=PT316.
- ↑ "Alcohol prescription by surgeons in the prevention and treatment of delirium tremens: Historic and current practice". General Hospital Psychiatry 24 (4): 257–259. 2002. doi:10.1016/S0163-8343(02)00188-3. PMID 12100836.
- ↑ "Use of alcoholic beverages in VA medical centers". Substance Abuse Treatment, Prevention, and Policy 1. 2006. doi:10.1186/1747-597X-1-30. PMID 17052353.
- ↑ Fuster, Daniel; Samet, Jeffrey H. (September 27, 2018). Longo, Dan L.. ed. "Alcohol Use in Patients with Chronic Liver Disease" (in en). New England Journal of Medicine 379 (13): 1251–1261. doi:10.1056/NEJMra1715733. ISSN 0028-4793. PMID 30257164. http://www.nejm.org/doi/10.1056/NEJMra1715733.
- ↑ Bailey, Blake. "Weekend in the Sun; Hollywood went wild over Charles Jackson and his 1944 best-seller, The Lost Weekend. Jackson reciprocated, thrilled that the celebrated Billy Wilder wanted to direct his dark, autobiographical novel of addiction. But would the result—a cinematic classic—destroy his literary achievement?" , Vanity Fair (magazine), February 28, 2013. Accessed February 15, 2017. "That summer, Hollywood columns had buzzed with rumors about who would play Don Birnam, the genteel alcoholic who ends up howling with delirium tremens. The role had been turned down by everyone from Cary Grant to Gary Cooper before the Welshman Ray Milland took it, refusing to heed an all but universal warning that he was committing 'career suicide.'"
- ↑ Cameron, Kate. 'The Lost Weekend' effectively portrays the damage caused by alcoholism on screen. , New York Daily News, January 2, 1945, reprinted February 17, 2015. Accessed February 15, 2017. "If you read the book, which was a best-seller last year, you know that Jackson did a remarkable job of recording the actions of Birnam, during a weekend binge of monumental proportions, and in setting down in graphic prose the effects produced on him by liquor. In adapting the book to the screen, Brackett and Wilder have accomplished an equally remarkable feat of projecting a case of delirium tremens on screen."
- ↑ Armstrong, Richard. Billy Wilder, American Film Realist , p. 41. McFarland & Company, 2004. ISBN 9780786421190. Accessed February 15, 2017. "Finally, Don's hallucination in which a wheeling bat devours a mouse places The Lost Weekend in a direct line of descent from the Gothicism of the '30s Universal horror cycle."
- ↑ Chapman, Graham (April 20, 1982). "Late Show with David Letterman, episode #1.46" (in en) (video). NBC. https://www.youtube.com/watch?v=984De23H7f4.
- ↑ "Big Sur Introduction | Shmoop". https://www.shmoop.com/study-guides/literature/big-sur-kerouac.
- ↑ "Алкогольная трагедия легендарного композитора Мусоргского". https://sobesednik.ru/skandaly/20130616-alkogolnaya-tragediya-legendarnogo-kompozitora-musorgskogo.
- ↑ Baldwin, Dan (2002). Just the FAQ's, Please, About Alcohol and Drug Abuse: Frequently Asked Questions from Families. America Star Books. pp. Chapter four. ISBN 978-1-61102-870-6. https://books.google.com/books?id=h-unAwAAQBAJ&pg=PT51.
- ↑ Paulson, Michael, "Gambling on O'Neill: Forest Whitaker Makes His Broadway Debut in 'Hughie'" , New York Times, February 3, 2016. Retrieved February 3, 2016.
- ↑ Lewis, Ellis (February 17, 2012). Report of The Trial and Conviction of John Haggerty, for The Murder of Melchoir Fordney, Late of The City of Lancaster, Pennsylvania. Gale, Making of Modern Law. p. 63. ISBN 978-1-275-31136-7.
- ↑ Belgian, Beers (May 29, 2020). "The Pink Elephant beer: Delirium Tremens" (in en). https://belgianbeers.co.uk/2020/05/29/the-pink-elephant-beer-delirium-tremens/.
- ↑ Thomas, Andrew (December 8, 2017). "11 Things You Should Know About Delirium Tremens". https://vinepair.com/articles/delirium-tremens/.
External links
- Why Does Alcohol Cause the Shakes? | Alcohol Withdrawal Syndrome Tremors | Dr Peter MCcann MCC, MBBS | Castle Craig Hospital
| Classification | |
|---|---|
| External resources |
 |
 KSF
KSF