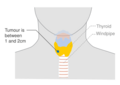
Thyroid cancer
Topic: Medicine
 From HandWiki - Reading time: 20 min
From HandWiki - Reading time: 20 min
| Thyroid cancer | |
|---|---|
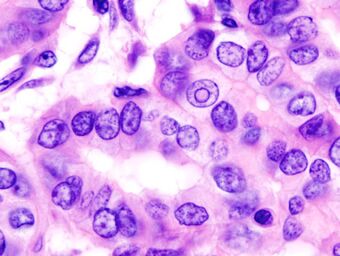 | |
| Micrograph of a papillary thyroid carcinoma demonstrating diagnostic features (nuclear clearing and overlapping nuclei). | |
| Specialty | Oncology |
| Symptoms | Swelling or lump in the neck[1] |
| Risk factors | Radiation exposure, enlarged thyroid, family history,[1][2] obesity[3] |
| Diagnostic method | Ultrasound, fine needle aspiration[1] |
| Differential diagnosis | Thyroid nodule, metastatic disease[1][4] |
| Treatment | Surgery, radiation therapy, chemotherapy, thyroid hormone, targeted therapy, watchful waiting[1] |
| Prognosis | Five year survival rates 98% (US)[5] |
| Frequency | 3.2 million (2015)[6] |
| Deaths | 31,900 (2015)[7] |
Thyroid cancer is cancer that develops from the tissues of the thyroid gland.[8][1] It is a disease in which cells grow abnormally and have the potential to spread to other parts of the body.[9][10] Symptoms can include swelling or a lump in the neck, difficulty swallowing or voice changes including hoarseness, or a feeling of something being in the throat due to mass effect from the tumor. However, most cases are asymptomatic.[1][11] Cancer can also occur in the thyroid after spread from other locations, in which case it is not classified as thyroid cancer.[4]
Risk factors include radiation exposure at a young age, having an enlarged thyroid, family history and obesity.[1][2][3] The four main types are papillary thyroid cancer, follicular thyroid cancer, medullary thyroid cancer, and anaplastic thyroid cancer.[4] Diagnosis is often based on ultrasound and fine needle aspiration.[1] Screening people without symptoms and at normal risk for the disease is not recommended.[11][12]
Treatment options may include surgery, radiation therapy including radioactive iodine, chemotherapy, thyroid hormone, targeted therapy, and watchful waiting.[1] Surgery may involve removing part or all of the thyroid.[4] Five-year survival rates are 98% in the United States.[5]
Globally as of 2015, 3.2 million people have thyroid cancer.[6] In 2012, 298,000 new cases occurred.[13] It most commonly is diagnosed between the ages of 20 and 65.[5] Women are affected more often than men.[5] Those of Asian descent are more commonly affected;[4] with a higher rate of mortality among Filipino females.[14] Rates have increased in the last few decades, which is believed to be due to better detection.[13] In 2015, it resulted in 31,900 deaths.[7]
Signs and symptoms
Most people with thyroid cancer do not have symptoms at the time of diagnosis and thyroid nodules are usually found incidentally on imaging of the neck.[11][15] Up to 65% of adults have small nodules in their thyroids, but typically under 10% of these nodules are found to be cancerous.[16] Sometimes, the first sign is an enlarged lymph node. Later symptoms that can be present are pain in the anterior region of the neck and changes in voice due to the close proximity of the recurrent laryngeal nerve[17] to the thyroid gland. These nodules and enlarged lymph nodes can also cause swelling in the neck and difficulty swallowing.
Thyroid cancer is usually found in a euthyroid patient, but symptoms of hyperthyroidism or hypothyroidism may be associated with a large or metastatic, well-differentiated tumor. Thyroid nodules are of particular concern when they are found in those under the age of 20. At this age, thyroid nodules are more likely to be malignant than benign.[18]
Causes
Thyroid cancers are thought to be related to a number of environmental and genetic predisposing factors, but significant uncertainty remains regarding their causes.[19]
Environmental exposure to ionising radiation from both natural background sources and artificial sources is suspected to play a significant role, and significantly increased rates of thyroid cancer occur in those exposed to mantlefield radiation for lymphoma, and those exposed to iodine-131 following the Chernobyl,[20] Fukushima, Kyshtym, and Windscale[21] nuclear disasters.[22] Thyroiditis and other thyroid diseases also predispose to thyroid cancer.[21][23]
Genetic causes include multiple endocrine neoplasia type 2, which markedly increases rates, particularly of the rarer medullary form of the disease.[24] Mutations in the genes for MenA and Men2B in multiple endocrine neoplasia is responsible for 25% of medullary thyroid cancers.[11] Hyperthyroidism is the overfunctioning of the thyroid gland causing an excessive amount of thyroid hormones to be released. These hormones contribute to one's metabolism, growth, brain development, body temperature, and reproductive function. This condition is also linked to Graves' Disease. A symptom of hyperthyroidism is a change in size of one's thyroid, which is associated with patients who have been found to have thyroid cancer. [90] There is also hypothyroidism, when there is an underfunction of the thyroid gland, which is associated with Hashimoto's thyroidosis. Hashimoto thyroidosis has a direct connection to an increased risk of thyroid cancer, along with multiple other cancer types.[89] Family relatives who have an issue with thyroids in their life will likely pass it down to their family. But the thyroid issues may present themselves in different ways. These ways can range from hypothyroidism, hyperthyroidism, Graves' Disease, Hashinoto's thyroidosis and cancer.
The FDA requires a boxed warning in the package inserts of GLP-1 agonists due to the risk of thyroid C-cell tumors, including medullary thyroid cancer (MTC), with a warning that GLP-1 agonists are contraindicated in people with a family or personal history of MTC or multiple endocrine neoplasia type 2.[25] In mice, long-term use of GLP-1 agonists stimulates calcitonin secretion, leading to C-cell hypertrophy and an increased risk of thyroid cancer, but no increased secretion of calcitonin has been observed in humans.[26] A retrospective national cohort study in France found an increased risk of thyroid cancer (all and medullary) following 1-3 years of treatment with GLP-1 agonists for diabetes,[27] but this was not observed in randomized control trials,[28] as well as in other large retrospective studies,[29][30] including one with long-term use of GLP-1 agonists and over 10-years of follow-up.[31] A small study of patients with low-risk thyroid cancer undergoing active surveillance showed that GLP-1RA therapy did not affect tumor growth kinetics.[32]
Diagnosis
After a thyroid nodule is found during a physical examination or incidentially on imaging[33], a referral to an endocrinologist or a thyroidologist may occur. Most commonly, an ultrasound is performed to confirm the presence of a nodule and assess the status of the whole gland. Various radiological clinical criteria, including the thyroid imaging reporting and data system (TI-RADs) score, are used to characterize the risk of malignancy.[34] TI-RADS developed by the American College of Radiology (ACR) guides clinicians in deciding which nodules require fine-needle aspiration cytology (FNAC) and in planning follow-up. Various online tools have been developed to assist in applying these criteria to clinical practice.[35] On ultrasound, nodules that are hypoechogenic (solid consistency), having irregular borders, increased vascularity, calcifications, or being taller than wide on transverse views are associated with malignancy.[11] Biopsy or cytology are required if the ultrasound characteristics suggest malignancy. If ultrasound results are equivocal or unclear, or if the thyroid nodule is small (typically less than 1 cm), the nodule can be monitored over time with serial ultrasounds.[11] Ultrasound has a sensitivity of 64-77% and a specificity of 82-90% for the detection of thyroid cancer.[11] Measurement of thyroid stimulating hormone, free and/or total triiodothyronine (T3) and thyroxine (T4) levels, and antithyroid antibodies will help decide if a functional thyroid disease such as Hashimoto's thyroiditis is present, a known cause of a benign nodular goiter.[36] A thyroid scan, performed often in conjunction with a radioactive iodine uptake test may be used to determine whether a nodule is hyperactive[37] which may help to make a decision whether to perform a biopsy of the nodule.[38] Measurement of calcitonin is necessary to exclude the presence of medullary thyroid cancer. To achieve a definitive diagnosis, a fine needle aspiration cytology test may be performed and reported according to the Bethesda system.[39]
After diagnosis, to understand potential for spread of disease, or for follow up monitoring after surgery, a whole body I-131 or I-123 radioactive iodine scan may be performed.[40]
In adults without symptoms, screening for thyroid cancer is not recommended.[41]
Classification

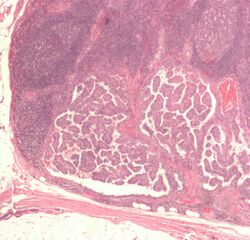
Thyroid cancers can be classified according to their histopathological characteristics.[43][44] These variants can be distinguished (distribution over various subtypes may show regional variation):
- Papillary thyroid cancer (75 to 85% of cases[45]) – is more often diagnosed in young females compared to other types of thyroid cancer and has an excellent prognosis. It may occur in women with familial adenomatous polyposis and in patients with Cowden syndrome. A follicular variant of papillary thyroid cancer also exists.[46]
- Newly reclassified variant: noninvasive follicular thyroid neoplasm with papillary-like nuclear features is considered an indolent tumor of limited biologic potential.
- Follicular thyroid cancer (10 to 20% of cases[45]) – occasionally seen in people with Cowden syndrome. Some include Hürthle cell carcinoma as a variant and others list it as a separate type.[4][47]
- Medullary thyroid cancer (5[45] to 8% of cases) – cancer of the parafollicular cells, often part of multiple endocrine neoplasia type 2.[48]
- Poorly differentiated thyroid cancer
- Anaplastic thyroid cancer (1 to 2%[49]) despite constituting only 1% of thyroid cancers, the type is responsible for 20% of thyroid cancer deaths.[11] It is characterized by a severe course with median survival of 6.5 months.[11]
- Others
- Thyroid lymphoma
- Squamous cell thyroid carcinoma
- Sarcoma of thyroid
- Hürthle cell carcinoma
The follicular and papillary types together can be classified as "differentiated thyroid cancer".[50] These types have a more favorable prognosis than the medullary and undifferentiated types.[51]
- Papillary microcarcinoma is a subset of papillary thyroid cancer defined as a nodule measuring less than or equal to 1 cm.[52] 43% of all thyroid cancers and 50% of new cases of papillary thyroid carcinoma are papillary microcarcinoma.[53][54] Management strategies for incidental papillary microcarcinoma on ultrasound (and confirmed on FNAB) range from total thyroidectomy with radioactive iodine ablation to lobectomy or observation alone. Harach et al. suggest using the term "occult papillary tumor" to avoid giving patients distress over having cancer. Woolner et al. first arbitrarily coined the term "occult papillary carcinoma", in 1960, to describe papillary carcinomas ≤ 1.5 cm in diameter.[55]
Staging
Cancer staging is the process of determining the extent of the development of a cancer. The TNM staging system is usually used to classify stages of cancers, but not of the brain.[56] The TNM system is broken into three key factors. The T part stands for the size of the tumor, and has it grown into any other body part near the body. The N is for if the cancer has grown into any lymph nodes nearby. And finally, the M stands for if the cancer has metastasized, and if the cancer has spread to any major organs in the body.
After the TNM system has been determined, the number system is then used to describe the severity of the cancer. The stages range from one (I) to four (IV), typically with stage one being the lowest and least amount of cancer spread, and stage four being the highest with the most amount of cancer spread through the body.[57]
Thyroid cancer staging can be determined by either clinical staging which includes several different tests evaluate the extent of the cancer, or pathological staging which includes surgery.[57]
-
Stage M1 thyroid cancer
-
Stage N1a thyroid cancer
-
Stage N1b thyroid cancer
-
Stage T1a thyroid cancer
-
Stage T1b thyroid cancer
-
Stage T2 thyroid cancer
-
Stage T3 thyroid cancer
-
Stage T4a thyroid cancer
-
Stage T4b thyroid cancer
Metastases
Detection of differentiated thyroid cancer metastases may be detected by performing a full-body scintigraphy using iodine-131.[58][59]
Scintigraphy, also known as iodine-131 scan, is a noninvasive imaging test that uses small amounts of radioactive material to check how the thyroid is working.[60] The thyroid cells (both normal and cancerous) easily absorb the iodine and when shown through imaging the scintigraphy scan will detect the radiation emitted by the iodine-131, so if the cancer has spread/metastasized to other parts of the body, they may also absorb the iodine which will show up as hot spots on the scan.
Most patients with thyroid cancer usually have it contained within the thyroid when they are diagnosed. Usually 30% will have metastatic cancer, with the cancer usually being spread to the lymph nodes in the neck.[61] Most patients with thyroid cancer have good chances of survival, but that changes if the cancer is spread outside of the neck at the time of the diagnosis. While death is rare in cases of thyroid cancer, it significantly increases when the cancer has spread to outside of the neck such as the lungs and bones. Only about 1-4% of the patients have a chance of this kind of metastatic cancer.[61]
Spread
Thyroid cancer can spread directly, via lymphatics or blood. Direct spread occurs through infiltration of the surrounding tissues. The tumor infiltrates into infrahyoid muscles, trachea, oesophagus, recurrent laryngeal nerve, carotid sheath, etc. The tumor then becomes fixed. Anaplastic carcinoma spreads mostly by direct spread, while papillary carcinoma spreads so the least. Lymphatic spread is most common in papillary carcinoma. Cervical lymph nodes become palpable in papillary carcinoma even when the primary tumor is unpalpable. Deep cervical nodes, pretracheal, prelaryngeal, and paratracheal groups of lymph nodes are often affected. The lymph node affected is usually the same side as that of the location of the tumor. Blood spread is also possible in thyroid cancers, especially in follicular and anaplastic carcinoma. The tumor emboli do angioinvasion of lungs; end of long bones, skull, and vertebrae are affected. Pulsating metastases occur because of their increased vascularity.[62]
Treatment
Thyroidectomy and dissection of central neck compartment is the initial step in treatment of thyroid cancer in the majority of cases.[15] Thyroid-preserving operations may be applied in cases, when thyroid cancer exhibits low biological aggressiveness (e.g. well-differentiated cancer, no evidence of lymph-node metastases, low MIB-1 index, no major genetic alterations like BRAF mutations, RET/PTC rearrangements, p53 mutations etc.) in patients younger than 45 years.[63] If the diagnosis of well-differentiated thyroid cancer (e.g. papillary thyroid cancer) is established or suspected by FNA, then surgery is indicated.[63][64] Surgical resection is the preferred treatment for all biopsy confirmed thyroid cancers. In those with very low risk tumors (such as small papillary tumors without evidence of local or metastatic spread or concerning cytologic findings), patients at high surgical risk due to medical problems, those with short expected lifespans or patients with serious medical issues precluding surgery, an active surveillance approach, in which the tumor is monitored over time (such as with serial imaging) may be pursued.[65]
Post surgical monitoring for recurrence or metastasis may include routine ultrasound, CT scans, FDG-PET/CT, radioactive iodine whole body scans, and routine laboratory blood tests for changes in thyroglobulin, thyroglobulin antibodies, or calcitonin, depending on the subtype of thyroid cancer.[66][67][68]
Radioactive iodine-131 is used in people with papillary or follicular thyroid cancer for ablation of residual thyroid tissue after surgery and for the treatment of thyroid cancer.[69] Post-surgical radioactive iodine is recommended for those with high risk of cancer recurrence. Post-surgery radioactive iodine does not reduce recurrence in those with low risk thyroid cancer.[11] Patients with medullary, anaplastic, and most Hurthle-cell cancers do not benefit from this therapy.[15] External irradiation may be used when the cancer is unresectable, when it recurs after resection, or to relieve pain from bone metastasis.[15]
Sorafenib and lenvatinib are approved for advanced metastatic thyroid cancer.[70] Numerous agents are in phase II and III clinical trials.[70]
Prognosis
The prognosis of thyroid cancer is related to the type of cancer and the stage at the time of diagnosis. For the most common form of thyroid cancer, papillary, the overall prognosis is excellent with 97%, 95%, and 90% 10, 15 and 20 year overall survival respectively.[71] The 5 year survival of all thyroid cancers, with treatment, is 98%.[11]
Many small thyroid cancers (mostly papillary type) rarely grow or metastasize. Some have stated that thyroid cancers are overdiagnosed and will rarely cause symptoms, illness, or death, even without treatment.[72] Low grade thyroid cancer is very commonly seen during autopsy studies, with the person dying from other causes.[72] Increasingly, small thyroid nodules are discovered as incidental findings on imaging (CT scan, MRI, ultrasound) performed for another purpose. Few of these people with incidentally discovered, subclinical thyroid cancers will ever have any symptoms, and overtreatment may be present.[72]
Thyroid cancer is three times more common in women than in men.[73] The overall relative 5-year survival rate for thyroid cancer is 85% for females and 74% for males.[74]
The identification of some molecular or DNA abnormalities has led to the development of therapies that target these molecular defects. The first of these agents to negotiate the approval process is vandetanib, a tyrosine kinase inhibitor that targets the RET proto-oncogene, two subtypes of the vascular endothelial growth factor receptor, and the epidermal growth factor receptor.[75] For differentiated thyroid carcinoma, strategies are evolving to use selected types of targeted therapy to increase radioactive iodine uptake in papillary thyroid carcinomas that have lost the ability to concentrate iodide. This strategy would make possible the use of radioactive iodine therapy to treat "resistant" thyroid cancers.
Mitogen-activated protein kinase (MAPK) variants are the most common genetic variants seen in thyroid cancer.[11] The BRAF 600E genetic variant is seen in 60% of papillary thyroid cancers. It is associated with increased risks of cervical lymph node metastasis, blunted response to radioactive iodine, and increased rates of local recurrence.[11] RasGTPase mutations are seen in 13% of papillary and 25-50% of follicular cancers and are associated with increased risk of vascular invasion and higher response to radioactive iodine.[11]
Prognosis is better in younger people than older ones.[74]
Prognosis depends mainly on the type of cancer and cancer stage.[11]
| Thyroid cancer type |
5-year survival | 10-year survival | ||||
|---|---|---|---|---|---|---|
| Stage I | Stage II | Stage III | Stage IV | Overall | Overall | |
| Papillary | 100%[76] | 100%[76] | 93%[76] | 51%[76] | 96%[77] or 97%[78] | 93%[77] |
| Follicular | 100%[76] | 100%[76] | 71%[76] | 50%[76] | 91%[77] | 85%[77] |
| Medullary | ||||||
| Anaplastic | (always stage IV)[76] | 7%[76] | 7%[76] or 14%[77] | (no data) | ||
Epidemiology
Thyroid cancer, in 2010, resulted in 36,000 deaths globally up from 24,000 in 1990.[79] Obesity may be associated with a higher incidence of thyroid cancer, but this relationship remains the subject of much debate.[80]
Thyroid cancer accounts for less than 1% of cancer cases and deaths in the UK. Around 2,700 people were diagnosed with thyroid cancer in the UK in 2011, and around 370 people died from the disease in 2012.[81]
However, in South Korea, thyroid cancer was the 5th most prevalent cancer, which accounted for 7.7% of new cancer cases in 2020.[82] This is most likely due to the increased use of ultrasounds in South Korea to look for thyroid cancer, even in asymptomatic patients.[83]
The incidence of thyroid cancer in the United States increased by 313% from a 1974-1977 incidence of 4.6 cases per 100,000 people to 14.4 cases per 100,000 people in 2010-13.[84] This increase is thought to be due to more widespread use of head and neck imaging (which may incidentally detect thyroid masses) as well as increased use of fine needle aspiration biopsies.[11]
Thyroid cancer tends to be seen more in females, possibly due to higher levels of estrogen. High levels of radiation in the neck can also increase the chance of getting thyroid cancer. Additionally, certain heritable genes can cause a higher likelihood.[85]
Notable cases
- Callum Ainley, English footballer[86]
- Ann-Katrin Berger, German women footballer
- Emre Can, German footballer[87]
- Jerry Dipoto, former Major League Baseball pitcher[88]
- Roger Ebert, American film critic
- Jennifer Grey, American actress
- Uhm Jung-hwa, South Korean singer, actress and dancer [89]
- Lee Moon-sae, South Korean ballad singer[90]
- Joe Piscopo, American actor
- William Rehnquist, Chief Justice of the United States (1986–2005) died September 3, 2005, from anaplastic thyroid cancer[91]
- Katee Sackhoff, American actress
- Karen Smyers, American swimmer
- Daniel Snyder, American owner of the Washington Football Team[92]
- Rod Stewart, British singer
- Scott Thompson, American businessman
- Sofía Vergara, American actress
- Julia Volkova, Russian singer
- April Winchell, American actress
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 "Thyroid Cancer Treatment" (in en). 27 Apr 2017. https://www.cancer.gov/types/thyroid/patient/thyroid-treatment-pdq#section/all.
- ↑ 2.0 2.1 "Thyroid cancer". Annual Review of Medicine 65: 125–137. 2014. doi:10.1146/annurev-med-061512-105739. PMID 24274180.
- ↑ 3.0 3.1 "Body Mass Index and Thyroid Cancer Risk: A Pooled Analysis of Half a Million Men and Women in the Asia Cohort Consortium". Thyroid 32 (3): 306–314. 2022. doi:10.1089/thy.2021.0445. PMID 34915752.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 "Thyroid Cancer Treatment" (in en). 12 May 2017. https://www.cancer.gov/types/thyroid/hp/thyroid-treatment-pdq#section/all.
- ↑ 5.0 5.1 5.2 5.3 "Cancer of the Thyroid - Cancer Stat Facts" (in en). https://seer.cancer.gov/statfacts/html/thyro.html.
- ↑ 6.0 6.1 Vos, Theo et al. (October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMID 27733282.
- ↑ 7.0 7.1 Wang, Haidong et al. (October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMID 27733281.
- ↑ Mehanna, Hisham (2024). "Evaluation of US Elastography in Thyroid Nodule Diagnosis: The ElaTION Randomized Control Trial". Radiology 313 (1). doi:10.1148/radiol.240705.
- ↑ "Cancer Fact sheet N°297". February 2014. https://www.who.int/mediacentre/factsheets/fs297/en/.
- ↑ "Defining Cancer". 2007-09-17. http://www.cancer.gov/cancertopics/cancerlibrary/what-is-cancer.
- ↑ 11.00 11.01 11.02 11.03 11.04 11.05 11.06 11.07 11.08 11.09 11.10 11.11 11.12 11.13 11.14 11.15 Boucai, Laura; Zafereo, Mark; Cabanillas, Maria E. (6 February 2024). "Thyroid Cancer: A Review". JAMA 331 (5): 425–435. doi:10.1001/jama.2023.26348. PMID 38319329.
- ↑ "Screening for Thyroid Cancer: US Preventive Services Task Force Recommendation Statement". JAMA 317 (18): 1882–1887. May 2017. doi:10.1001/jama.2017.4011. PMID 28492905.
- ↑ 13.0 13.1 World Cancer Report 2014.. World Health Organization. 2014. pp. Chapter 5.15. ISBN 978-92-832-0429-9.
- ↑ Paz-Pacheco, Elizabeth; Juan, Mari Des San (2 March 2023). "Incidence, Recurrence and Mortality Among Filipinos With Differentiated Thyroid Cancer: A Systematic Review". Journal of the ASEAN Federation of Endocrine Societies 38 (1): 100–107. doi:10.15605/jafes.038.01.14. PMID 37252408.
Nguyen, Michelle Linh T.; Hu, Jiaqi; Hastings, Kattherine G.; Daza, Eric J; Cullen, Mark R.; Orloff, Lisa A.; Palaniappan, Latha P. (7 September 2017). "Thyroid cancer mortality higher in Filipinos in United States: an analysis using national mortality records from 2003–2012". Cancer 123 (24): 4860–4867. doi:10.1002/cncr.30958. PMID 28881423.
Lee, Alice W.; Mendoza, Roy A.; Aman, Shehla; Jsu, Robert; Liu, Lihua (February 2022). "Thyroid cancer incidence disparities among ethnic Asian American populations, 1990–2014". Annals of Epidemiology 66: 28–36. doi:10.1016/j.annepidem.2021.11.002. PMID 34774744. - ↑ 15.0 15.1 15.2 15.3 "Thyroid and Parathyroid Cancers". Cancer Management: A Multidisciplinary Approach (11th ed.). Lawrence, Kansas: CMP Media. 2008. ISBN 978-1-891483-62-2. http://www.cancernetwork.com/cancer-management-11/chapter05/article/10165/1402668.
- ↑ "The Diagnosis and Management of Thyroid Nodules: A Review". JAMA 319 (9): 914–924. March 2018. doi:10.1001/jama.2018.0898. PMID 29509871.
- ↑ "Thyroid Cancer" (in en). 2021-02-01. https://www.cancer.columbia.edu/cancer-types-care/types/thyroid-cancer/about-thyroid-cancer.
- ↑ Grani, Giorgio; Sponziello, Marialuisa; Filetti, Sebastiano; Durante, Cosimo (2024-08-16). "Thyroid nodules: diagnosis and management" (in en). Nature Reviews Endocrinology 20 (12): 715–728. doi:10.1038/s41574-024-01025-4. ISSN 1759-5029. PMID 39152228. https://www.nature.com/articles/s41574-024-01025-4.
- ↑ "Thyroid Cancer Overview - Signaling Pathway. Diagnosis. Targeted Therapy - Creative Biolabs". https://www.creativebiolabs.net/thyroid-cancer-overview-signaling-pathway-diagnosis-targeted-therapy.htm.
- ↑ "Radioactive I-131 from Fallout". National Cancer Institute. http://www.cancer.gov/cancertopics/causes/i131.
- ↑ 21.0 21.1 "Thyroid cancer epidemiology in England and Wales: time trends and geographical distribution". British Journal of Cancer 67 (2): 330–340. February 1993. doi:10.1038/bjc.1993.61. PMID 8431362.
- ↑ "Experts link higher incidence of children's cancer to Fukushima radiation". 12 October 2015. http://www.sciencealert.com/experts-link-higher-incidence-of-children-s-cancer-to-fukushima-radiation.
- ↑ "Thyroid cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up". Annals of Oncology 21 (Suppl 5): v214–v219. May 2010. doi:10.1093/annonc/mdq190. PMID 20555084.
- ↑ "Genetics of Endocrine and Neuroendocrine Neoplasias". National Cancer Institute. 1980-01-01. http://www.cancer.gov/cancertopics/pdq/genetics/medullarythyroid/HealthProfessional.
- ↑ Nachawi, Noura; Rao, Pratibha PR; Makin, Vinni (2022). "The role of GLP-1 receptor agonists in managing type 2 diabetes". Cleveland Clinic Journal of Medicine 89 (8): 457–464. doi:10.3949/ccjm.89a.21110. PMID 35914933.
- ↑ Yu, Minzhi; Benjamin, Mason M.; Srinivasan, Santhanakrishnan et al. (2018). "Battle of GLP-1 delivery technologies". Advanced Drug Delivery Reviews 130: 113–130. doi:10.1016/j.addr.2018.07.009. PMID 30009885.
- ↑ Bezin, Julien; Gouverneur, Amandine; Pénichon, Marine; Mathieu, Clément; Garrel, Renaud; Hillaire-Buys, Dominique; Pariente, Antoine; Faillie, Jean-Luc (2023-02-01). "GLP-1 Receptor Agonists and the Risk of Thyroid Cancer". Diabetes Care 46 (2): 384–390. doi:10.2337/dc22-1148. ISSN 1935-5548. PMID 36356111.
- ↑ Vilsbøll, Tina; Stellfeld, Michael; Aroda, Vanita R.; Dandanell, Sune; David, Jens-Peter; Kristiansen, Ceyda T. P.; Rasmussen, Søren; Roberts, Fiona L. et al. (2025-11-25). "Assessment of thyroid cancer risk associated with glucagon-like peptide 1 receptor agonist use". Diabetes, Obesity and Metabolism n/a (n/a). doi:10.1111/dom.70291. ISSN 1462-8902. https://dom-pubs.pericles-prod.literatumonline.com/doi/10.1111/dom.70291.
- ↑ Morales, Daniel R.; Bu, Fan; Viernes, Benjamin; DuVall, Scott L.; Matheny, Michael E.; Simon, Katherine R.; Falconer, Thomas; Richter, Lauren R. et al. (2025-08-01). "Risk of Thyroid Tumors With GLP-1 Receptor Agonists: A Retrospective Cohort Study" (in en). Diabetes Care 48 (8): 1386–1394. doi:10.2337/dc25-0154. ISSN 0149-5992. PMID 40465422. PMC 12281980. https://diabetesjournals.org/care/article/48/8/1386/160553/Risk-of-Thyroid-Tumors-With-GLP-1-Receptor.
- ↑ Baxter, Sarah M.; Lund, Lars Christian; Andersen, Jacob H.; Brix, Thomas H.; Hegedüs, Laszlo; Hsieh, Miyuki Hsing-Chun; Su, Chris Tzu-Ting; Cheng, Michael Chun-Yuan et al. (January 2025). "Glucagon-Like Peptide 1 Receptor Agonists and Risk of Thyroid Cancer: An International Multisite Cohort Study". Thyroid 35 (1): 69–78. doi:10.1089/thy.2024.0387. ISSN 1050-7256. PMID 39772758. https://www.liebertpub.com/doi/10.1089/thy.2024.0387.
- ↑ Pollack, Rena; Stokar, Joshua (2025). "Long-Term Glucagon-Like Peptide 1 Receptor Agonist Use Is Not Associated With Increased Risk of Thyroid Cancer in Adults With Type 2 Diabetes" (in en). Diabetes/Metabolism Research and Reviews 41 (8). doi:10.1002/dmrr.70104. ISSN 1520-7560. PMID 41182904.
- ↑ Patrizio, Armando; Newman, Samantha K; Tuttle, R Michael; Boucai, Laura (2025-11-14). "Effect of GLP-1 receptor agonists on patients with thyroid carcinomas undergoing active surveillance" (in en). Journal of the Endocrine Society. doi:10.1210/jendso/bvaf182. ISSN 2472-1972.
- ↑ Mehanna, Hisham (2024). "Evaluation of US Elastography in Thyroid Nodule Diagnosis: The ElaTION Randomized Control Trial". Radiology 313 (1). doi:10.1148/radiol.24070.
- ↑ "Ultrasound imaging classifications of thyroid nodules for malignancy risk stratification and clinical management: state of the art". Gland Surgery 8 (Suppl 3): S233–S244. September 2019. doi:10.21037/gs.2019.07.01. PMID 31559190.
- ↑ "TIRADS calculator with free report generator!" (in en-US). 2024-06-18. https://radathand.com/radiology-calculators/body-imaging/tirads-calculator/.
- ↑ "Diagnosis and treatment of the solitary thyroid nodule. Results of a European survey". Clinical Endocrinology 50 (3): 357–363. March 1999. doi:10.1046/j.1365-2265.1999.00663.x. PMID 10435062.
- ↑ "Thyroid scan: MedlinePlus Medical Encyclopedia" (in en). https://medlineplus.gov/ency/article/003829.htm.
- ↑ "Vol 7 Issue 6 p.3-4" (in en-US). https://www.thyroid.org/patient-thyroid-information/ct-for-patients/vol-7-issue-6/vol-7-issue-6-p-3-4/.
- ↑ "The bethesda system for reporting thyroid cytopathology: interpretation and guidelines in surgical treatment". Indian Journal of Otolaryngology and Head and Neck Surgery 64 (4): 305–311. December 2012. doi:10.1007/s12070-011-0289-4. PMID 24294568.
- ↑ "I-123 diagnostic thyroid tumor whole-body scanning with imaging at 6, 24, and 48 hours". Clinical Nuclear Medicine 27 (1): 1–8. January 2002. doi:10.1097/00003072-200201000-00001. PMID 11805475.
- ↑ "Screening for Thyroid Cancer: US Preventive Services Task Force Recommendation Statement". JAMA 317 (18): 1882–1887. May 2017. doi:10.1001/jama.2017.4011. PMID 28492905.
- ↑ "Demographic and histological subtypes of Hurthle cell tumours of the thyroid in a South African setting". South African Journal of Surgery. Suid-Afrikaanse Tydskrif vir Chirurgie 56 (3): 20–23. September 2018. doi:10.17159/2078-5151/2018/v56n3a2557. PMID 30264938.
- ↑ "Thyroid Cancer Treatment". National Cancer Institute. 1980-01-01. http://www.cancer.gov/cancertopics/pdq/treatment/thyroid/HealthProfessional/page2.
- ↑ "Thyroid cancer". National Cancer Institute. http://cancerweb.ncl.ac.uk/cancernet/101252.html#2_CELLULARCLASSIFICATION.
- ↑ 45.0 45.1 45.2 Chapter 20 in: Robbins Basic Pathology. Philadelphia: Saunders. 2007. ISBN 978-1-4160-2973-1. 8th edition.
- ↑ "Follicular variant of papillary thyroid carcinoma is a unique clinical entity: a population-based study of 10,740 cases". Thyroid 23 (10): 1263–1268. October 2013. doi:10.1089/thy.2012.0453. PMID 23477346.
- ↑ "Follicular thyroid cancer and Hürthle cell carcinoma: challenges in diagnosis, treatment, and clinical management". The Lancet. Diabetes & Endocrinology 6 (6): 500–514. June 2018. doi:10.1016/S2213-8587(17)30325-X. PMID 29102432.
- ↑ "New therapeutic approaches to treat medullary thyroid carcinoma". Nature Clinical Practice. Endocrinology & Metabolism 4 (1): 22–32. January 2008. doi:10.1038/ncpendmet0717. PMID 18084343.
- ↑ "Anaplastic Thyroid Cancer". https://columbiasurgery.org/conditions-and-treatments/anaplastic-thyroid-cancer.
- ↑ "Thyroid cancer review 2: management of differentiated thyroid cancers". International Journal of Clinical Practice 59 (12): 1459–1463. December 2005. doi:10.1111/j.1368-5031.2005.00672.x. PMID 16351679. http://www.medscape.com/viewarticle/518396.
- ↑ "Thyroid cancer review 3: management of medullary and undifferentiated thyroid cancer". International Journal of Clinical Practice 60 (1): 80–84. January 2006. doi:10.1111/j.1742-1241.2005.00673.x. PMID 16409432.
- ↑ "TNM classification of thyroid carcinoma". World Journal of Surgery 31 (5): 879–887. May 2007. doi:10.1007/s00268-006-0864-0. PMID 17308849.
- ↑ "Thyroid Papillary Microcarcinoma: Etiology, Clinical Manifestations, Diagnosis, Follow-up, Histopathology and Prognosis". Iranian Journal of Pathology 11 (1): 1–19. 2016. PMID 26870138.
- ↑ "The most commonly occurring papillary thyroid cancer in the United States is now a microcarcinoma in a patient older than 45 years". Thyroid 21 (3): 231–236. March 2011. doi:10.1089/thy.2010.0137. PMID 21268762.
- ↑ "Occult papillary carcinoma of the thyroid gland: a study of 140 cases observed in a 30-year period". The Journal of Clinical Endocrinology and Metabolism 20: 89–105. January 1960. doi:10.1210/jcem-20-1-89. PMID 13845950.
- ↑ "Cancer Staging - NCI" (in en). 2015-03-09. https://www.cancer.gov/about-cancer/diagnosis-staging/staging.
- ↑ 57.0 57.1 "Thyroid Cancer Stages | Stages of Thyroid Cancer" (in en). https://www.cancer.org/cancer/types/thyroid-cancer/detection-diagnosis-staging/staging.html.
- ↑ "Bone metastases of differentiated thyroid cancer: impact of early 131I-based detection on outcome". Endocrine-Related Cancer 14 (3): 799–807. September 2007. doi:10.1677/ERC-07-0120. PMID 17914109.
- ↑ "Detection and treatment of lung metastases of differentiated thyroid carcinoma in patients with normal chest X-rays". Journal of Nuclear Medicine 29 (11): 1790–1794. November 1988. PMID 3183748.
- ↑ Yavuz, Sahzene; Puckett, Yana (2025), "Iodine-131 Uptake Study", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 32644709, http://www.ncbi.nlm.nih.gov/books/NBK559283/, retrieved 2025-11-30
- ↑ 61.0 61.1 "Vol 8 Issue 4 p.11" (in en-US). https://www.thyroid.org/patient-thyroid-information/ct-for-patients/volume-8-issue-4/vol-8-issue-4-p-11/.
- ↑ A concise textbook of surgery (5th ed.). Calcutta: Dr S. Das. 2008. ISBN 978-81-905681-2-8.
- ↑ 63.0 63.1 "Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer". Thyroid 19 (11): 1167–1214. November 2009. doi:10.1089/thy.2009.0110. PMID 19860577.
- ↑ British Thyroid Association, Royal College of Physicians, Perros P (2007). Guidelines for the management of thyroid cancer. 2nd edition. Report of the Thyroid Cancer Guidelines Update Group. Royal College of Physicians. p. 16. ISBN 978-1-86016-309-8. http://www.british-thyroid-association.org/news/Docs/Thyroid_cancer_guidelines_2007.pdf. Retrieved 12 July 2013.
- ↑ Haugen, Bryan R.; Alexander, Erik K.; Bible, Keith C.; Doherty, Gerard M.; Mandel, Susan J.; Nikiforov, Yuri E.; Pacini, Furio; Randolph, Gregory W. et al. (January 2016). "2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer". Thyroid 26 (1): 1–133. doi:10.1089/thy.2015.0020. PMID 26462967.
- ↑ "2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer". Thyroid 26 (1): 1–133. January 2016. doi:10.1089/thy.2015.0020. PMID 26462967.
- ↑ "Revised American Thyroid Association guidelines for the management of medullary thyroid carcinoma". Thyroid 25 (6): 567–610. June 2015. doi:10.1089/thy.2014.0335. PMID 25810047.
- ↑ "American Thyroid Association guidelines for management of patients with anaplastic thyroid cancer". Thyroid 22 (11): 1104–1139. November 2012. doi:10.1089/thy.2012.0302. PMID 23130564.
- ↑ "Guidelines for the management of thyroid cancer". Clinical Endocrinology 81 (Suppl 1): 1–122. July 2014. doi:10.1111/cen.12515. PMID 24989897.
- ↑ 70.0 70.1 "Recent advances in managing differentiated thyroid cancer". F1000Research 7: 86. 2018-01-18. doi:10.12688/f1000research.12811.1. PMID 29399330.
- ↑ Ito, Yasuhiro; Miyauchi, Akira; Kihara, Minoru; Fukushima, Mitsuhiro; Higashiyama, Takuya; Miya, Akihiro (March 2018). "Overall Survival of Papillary Thyroid Carcinoma Patients: A Single-Institution Long-Term Follow-Up of 5897 Patients". World Journal of Surgery 42 (3): 615–622. doi:10.1007/s00268-018-4479-z. PMID 29349484.
- ↑ 72.0 72.1 72.2 Overdiagnosed: Making People Sick in the Pursuit of Health. [Malaysia?]: Beacon Press. 2011. pp. 61–34. ISBN 978-0-8070-2200-9.
- ↑ "Thyroid Cancer". MedicineNet.com. http://www.medicinenet.com/thyroid_cancer/article.htm.
- ↑ 74.0 74.1 Numbers from EUROCARE, from Page 10 in: Thyroid cancer. Berlin: Springer. 2005. ISBN 978-3-540-22309-2.
- ↑ "FDA approves new treatment for rare form of thyroid cancer" (Press release). U.S. Food and Drug Administration. 6 April 2011. Archived from the original on 10 April 2011. Retrieved 7 April 2011.
- ↑ 76.00 76.01 76.02 76.03 76.04 76.05 76.06 76.07 76.08 76.09 76.10 cancer.org Thyroid Cancer By the American Cancer Society. In turn citing: AJCC Cancer Staging Manual (7th ed).
- ↑ 77.0 77.1 77.2 77.3 77.4 Numbers from National Cancer Database in the US, from Page 10 in: Thyroid cancer. Berlin: Springer. 2005. ISBN 978-3-540-22309-2. (Note:Book also states that the 14% 10-year survival for anaplastic thyroid cancer was overestimated)
- ↑ Rounded up to nearest natural number from 96.7% as given by "Thyroid, Papillary Carcinoma". eMedicine. 28 September 2010. http://emedicine.medscape.com/article/282276-overview.
- ↑ "Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010". Lancet 380 (9859): 2095–2128. December 2012. doi:10.1016/S0140-6736(12)61728-0. PMID 23245604. PMC 10790329. http://www.cobiss.si/scripts/cobiss?command=DISPLAY&base=cobib&rid=1537267652&fmt=11.
- ↑ "Mechanisms in endocrinology: the crosstalk between thyroid gland and adipose tissue: signal integration in health and disease". European Journal of Endocrinology 171 (4): R137–R152. October 2014. doi:10.1530/eje-14-0067. PMID 25214234. http://eje-online.org/content/171/4/R137.long.
- ↑ "Thyroid cancer statistics". http://www.cancerresearchuk.org/cancer-info/cancerstats/types/thyroid/.
- ↑ "Republic of Korea Cancer Rates". Global Cancer Observatory (GCO). World Health Organization. 2020. https://gco.iarc.fr/today/data/factsheets/populations/410-korea-republic-of-fact-sheets.pdf.
- ↑ "Vol 10 Issue 2 p.10-11" (in en-US). https://www.thyroid.org/patient-thyroid-information/ct-for-patients/february-2017/vol-10-issue-2-p-10-11/.
- ↑ Lim, Hyeyeun; Devesa, Susan S.; Sosa, Julie A.; Check, David; Kitahara, Cari M. (4 April 2017). "Trends in Thyroid Cancer Incidence and Mortality in the United States, 1974-2013". JAMA 317 (13): 1338–1348. doi:10.1001/jama.2017.2719. PMID 28362912.
- ↑ "Thyroid cancer - Symptoms and causes" (in en). https://www.mayoclinic.org/diseases-conditions/thyroid-cancer/symptoms-causes/syc-20354161.
- ↑ "Callum Ainley: Grimsby Town midfielder diagnosed with thyroid cancer". BBC Sport. 16 January 2024. https://www.bbc.co.uk/sport/football/67987683.
- ↑ Hunsley, James (27 January 2023). "'I am so grateful' - ex-Liverpool midfielder Emre Can opens up on battle with cancer". Goal.com. https://www.goal.com/en/news/ex-liverpool-midfielder-emre-can-battle-thyroid-cancer-juventus/bltafd65cb286ab51.
- ↑ Bamberger, Michael (27 May 2002). "Survivors". Sports Illustrated. http://sportsillustrated.cnn.com/vault/article/magazine/MAG1025858/index.htm. Retrieved 11 August 2013.
- ↑ "Uhm Jung-hwa had Thyroid cancer op". The Korean Herald. 20 October 2010. http://www.koreaherald.com/view.php?ud=20101020000759.
- ↑ "Lee Moon-se risks cancer relapse to keep singing". The Korean Herald. 31 March 2015. http://m.kpopherald.com/view.php?ud=201503311319126591959_2.
- ↑ "Rehnquist Eulogies Look Beyond Bench". The Washington Post. 8 September 2005. https://www.washingtonpost.com/wp-dyn/content/article/2005/09/07/AR2005090701791.html.
- ↑ "Celebrities with Thyroid problems". Alexander Shifrin. http://www.shifrinmd.com/celebrities-with-thyroid-problems-2.html.
External links
| Classification | |
|---|---|
| External resources |
Template:Endocrine gland neoplasia
 |
 KSF
KSF