Viral hemorrhagic fever
Topic: Medicine
 From HandWiki - Reading time: 11 min
From HandWiki - Reading time: 11 min
This article needs more medical references for verification or relies too heavily on primary sources. (July 2020) |
| Viral hemorrhagic fever | |
|---|---|
| Other names | viral haemorrhagic fever |
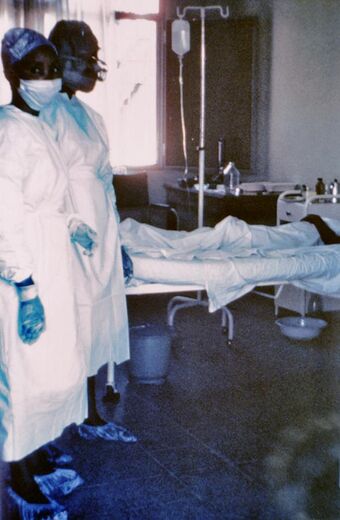 | |
| Two nurses standing near Mayinga N'Seka, a nurse with Ebola virus disease in the 1976 outbreak in Zaire. N'Seka died a few days later due to severe internal hemorrhage. | |
| Specialty | Infectious disease |
Viral hemorrhagic fevers (VHFs) are a diverse group of diseases. "Viral" means a health problem caused by infection from a virus, "hemorrhagic" means to bleed, and "fever" means an unusually high body temperature. Bleeding and fever are common signs of VHFs, which is how the group of infections got its common name.
There are five known families of RNA viruses which cause VHFs: Arenaviridae, Filoviridae, Flaviviridae, Hantaviridae, and Rhabdoviridae. Some VHFs are usually mild, such as nephropathia epidemica (within the family Hantaviridae). But some are usually severe and have a high death rate, such as Ebola virus (within the family Filoviridae). All VHFs can potentially cause severe blood loss, high fever, and death.
Both humans and non human animals can be infected.
Signs and symptoms
The following are signs and symptoms of most or all VHFs.
- Circulatory shock
- Diarrhea (feces which resemble more liquid than solid)
- Headache
- Hypotension (low blood pressure)
- Fever (high body temperature)
- Flushing (redness) of the face and chest
- Hemorrhage (bleeding) and sometimes bleeding diathesis (a person loses more blood than usual from an injury – for example, getting only a little cut, and losing a lot of blood)
- Malaise (a general feeling of sickness)
- Myalgia (muscle pain)
- Petechiae (small red or purple spots – about four millimeters in diameter, which is less than one fourth the width of a human finger)
- Swelling caused by edema
The severity of symptoms varies with the type of virus. The "VHF syndrome" causes bleeding diathesis, capillary leak, and circulatory shock. It happens to most people who have Filoviridae infections (such as Ebola virus or Marburg virus), Crimean–Congo hemorrhagic fever (CCHF), or the South American hemorrhagic fevers (which are caused by Arenaviridae). VHF syndrome only happens to a small minority of people who have dengue fever or Rift Valley fever.
Causes
Five families of RNA viruses have been recognized as being able to cause hemorrhagic fevers.[citation needed]
- The order Bunyavirales includes the families Arenaviridae, Fimoviridae, and all members of the former family Bunyaviridae, especially Peribunyaviridae.
- The family Arenaviridae include the viruses responsible for Lassa fever (Lassa virus), Lujo virus, Argentine (Junin virus), Bolivian (Machupo virus), Brazilian (Sabiá virus), Chapare hemorrhagic fever (Chapare virus), Venezuelan (Guanarito virus) and Whitewater Arroyo virus hemorrhagic fevers.
- The former family Bunyaviridae includes
- the causative agents of Hantavirus hemorrhagic fever with renal syndrome (HV-HFRS) (Hantaviridae),
- the Crimean-Congo hemorrhagic fever (CCHF) virus from the genus Orthonairovirus (Nairoviridae),
- Garissa virus and Ilesha virus from the genus Orthobunyavirus (Peribunyaviridae), and
- the Rift Valley fever (RVF) virus from the genus Phlebovirus (Phenuiviridae).
- The family Filoviridae (order Mononegavirales) includes Ebola virus and Marburg virus.
- The family Flaviviridae (order Amarillovirales) includes dengue, yellow fever, and two viruses in the tick-borne encephalitis group that cause VHF: Omsk hemorrhagic fever virus and Kyasanur Forest disease virus.
- The family Rhabdoviridae (order Mononegavirales). In September 2012 scientists writing in the journal PLOS Pathogens reported the isolation of a member of the Rhabdoviridae responsible for two fatal and two non-fatal cases of hemorrhagic fever in the Bas-Congo district of the Democratic Republic of Congo. The virus was named Bas-Congo virus. The non-fatal cases occurred in healthcare workers involved in the treatment of the other two, suggesting the possibility of person-to-person transmission.[1] This virus is related to the Ephemerovirus and Tibrovirus genera.
- The family Togaviridae (order Martellivirales) includes Chikungunya virus which causes Chikungunya fever.
The pathogen that caused the cocoliztli epidemics in Mexico of 1545 and 1576 is still unknown, and the 1545 epidemic may have been bacterial rather than viral.[2][3]
Pathophysiology
The reasons for variation among patients infected with the same virus are unknown but stem from a complex system of virus-host interactions. Dengue fever becomes more virulent during a second infection by means of antibody-dependent enhancement. After the first infection, macrophages display antibodies on their cell membranes specific to the dengue virus. By attaching to these antibodies, dengue viruses from a second infection are better able to infect the macrophages, thus reducing the immune system's ability to fight off infection.[citation needed]
Diagnosis
Definitive diagnosis is usually made at a reference laboratory with advanced biocontainment capabilities. The findings of laboratory investigation vary somewhat between the viruses but in general, there is a decrease in the total white cell count (particularly the lymphocytes), a decrease in the platelet count, an increase in the blood serum liver enzymes, and reduced blood clotting ability measured as an increase in both the prothrombin (PT) and activated partial thromboplastin times (PTT). The hematocrit may be elevated. The serum urea and creatine may be raised but this is dependent on the hydration status of the patient. The bleeding time tends to be prolonged.[citation needed]
Prevention
With the exception of yellow fever vaccine and Ebola vaccines, vaccines for VHFs are generally not available. For someone exposed to CCHF, ribavirin is available as post-exposure prophylaxis (PEP).[4] Ribavirin may also help in exposure to Lassa fever.[5]
Any person who is taking care of a patient with any VHF (except dengue fever) should take multiple precautions against exposure and infection. The precautions include hand hygiene, double gloves, gowns, shoe and leg coverings, and face shields or goggles. Lassa, CCHF, Ebola, and Marburg viruses may be particularly prone to nosocomial (hospital-based) spread. Airborne precautions should be utilized including, at a minimum, a fit-tested, HEPA filter-equipped respirator (such as an N95 mask), a battery-powered, air-purifying respirator, or a positive pressure supplied air respirator to be worn by personnel coming within 1.8 meters (six feet) of a VHF patient. Groups of patients should be cohorted (sequestered) to a separate building or a ward with an isolated air-handling system. Environmental decontamination is typically accomplished with hypochlorite (e.g. bleach) or phenolic disinfectants.[6]
Management
Medical management of VHF patients may require intensive supportive care. Antiviral therapy with intravenous ribavirin may be useful in Bunyaviridae and Arenaviridae infections (specifically Lassa fever, RVF, CCHF, and HFRS due to Old World Hantavirus infection) and can be used only under an experimental protocol as IND approved by the U.S. Food and Drug Administration (FDA). Interferon may be effective in Argentine or Bolivian hemorrhagic fevers (also available only as IND).[citation needed]
Potential therapies
A potential novel treatment, the NMT inhibitor, has been shown to completely inhibit Lassa (LAS) and Junín (JUN) viral infections in cells based assays.[7]
Epidemiology
- Cocoliztli in Mexico 1545 and 1576 (suspected)[2][8][9][10][11]
- The Great Yellow Fever Epidemic of 1793 in Philadelphia, PA, US. Nearly 10% of the population of 50,000 died from the disease.
- Mékambo in Gabon is the site of several outbreaks of Ebola virus disease.
- Orientale Province, Democratic Republic of the Congo villages of Durba and Watsa were the epicenter of the 1998–2000 outbreak of Marburg virus disease.
- Uíge Province in Angola was the site of another outbreak of Marburg virus disease in 2005, the largest one to date of this disease.[12]
- A VHF outbreak in the village of Mweka, Democratic Republic of the Congo (DRC) that started in August 2007, and that has killed 103 people (100 adults and three children), has been shown to be caused (at least partially) by Ebola virus.
- A viral hemorrhagic fever is a possible cause of the Plague of Athens during the Peloponnesian War.[13]
- A viral hemorrhagic fever is an alternate theory of the cause of the Black Death and the Plague of Justinian[14]
- The initial, and currently only, outbreak of Lujo virus in September–October 2008 left four of five patients dead.[15]
- The 2014 West Africa Ebola outbreak, which was the biggest outbreak in history.
Biowarfare potential
The VHF viruses are spread in a variety of ways. Some may be transmitted to humans through a respiratory route. The viruses are considered by military medical planners to have a potential for aerosol dissemination, weaponization, or likelihood for confusion with similar agents that might be weaponized.[16][17]
Scientific Research Institute of Medicine of the Ministry of Defense in Sergiyev Posad was researching the military use potential of hemorrhagic fever viruses.
See also
- Biosafety
- Jordi Casals-Ariet
- Dr. Matthew Lukwiya (1957–2000)
- C. J. Peters
References
- ↑ "A novel rhabdovirus associated with acute hemorrhagic fever in central Africa". PLOS Pathog. 8 (9). September 2012. doi:10.1371/journal.ppat.1002924. PMID 23028323.
- ↑ 2.0 2.1 "Megadrought and megadeath in 16th century Mexico". Emerging Infect. Dis. 8 (4): 360–62. April 2002. doi:10.3201/eid0804.010175. PMID 11971767.
- ↑ "500 years later, scientists discover what probably killed the Aztecs". The Guardian. Agence France-Presse. 2018-01-16. https://www.theguardian.com/world/2018/jan/16/mexico-500-years-later-scientists-discover-what-killed-the-aztecs.
- ↑ "Systematic Review and Meta-analysis of Postexposure Prophylaxis for Crimean-Congo Hemorrhagic Fever Virus among Healthcare Workers.". Emerg Infect Dis 24 (9): 1642–1648. 2018. doi:10.3201/eid2409.171709. PMID 30124196.
- ↑ "Ribavirin for Lassa fever postexposure prophylaxis.". Emerg Infect Dis 16 (12): 2009–11. 2010. doi:10.3201/eid1612.100994. PMID 21122249.
- ↑ Woods, Lt Col Jon B., ed (2005). USAMRIID's Medical Management of Biological Casualties Handbook (6th ed.). Fort Detrick MA: U.S. Army Medical Institute of Infectious Diseases. pp. 143–44. http://www.usamriid.army.mil/education/bluebookpdf/USAMRIID%20BlueBook%206th%20Edition%20-%20Sep%202006.pdf. Retrieved 2007-06-09.
- ↑ Witwit, Haydar; Betancourt, Carlos Alberto; Cubitt, Beatrice; Khafaji, Roaa; Kowalski, Heinrich; Jackson, Nathaniel; Ye, Chengjin; Martinez-Sobrido, Luis et al. (2024-08-26). "Cellular N-Myristoyl Transferases Are Required for Mammarenavirus Multiplication" (in en). Viruses 16 (9): 1362. doi:10.3390/v16091362. ISSN 1999-4915. PMID 39339839.
- ↑ "Was the Huey Cocoliztli a Haemorrhagic Fever?". http://usmex.ucsd.edu/assets/022/10129.pdf.
- ↑ "Indigenous Hemorrhagic Fever and The Spanish Conquest". http://www.earthmatrix.com/linguistic/cocolitzli.pdf.
- ↑ "Large Epidemics of Hemorrhagic Fevers in Mexico 1545–1815". Am J Trop Med Hyg 62 (6): 733–39. June 2000. doi:10.4269/ajtmh.2000.62.733. PMID 11304065. http://www.ajtmh.org/cgi/reprint/62/6/733.pdf. Retrieved 2006-12-04.
- ↑ "Epidemics in New Spain". http://faculty.nwacc.edu/abrown/WesternCiv/Migrations%20Unit%202.rtf.
- ↑ Towner, J. S.; Khristova, M. L.; Sealy, T. K.; Vincent, M. J.; Erickson, B. R.; Bawiec, D. A.; Hartman, A. L.; Comer, J. A. et al. (2006). "Marburgvirus Genomics and Association with a Large Hemorrhagic Fever Outbreak in Angola". Journal of Virology 80 (13): 6497–516. doi:10.1128/JVI.00069-06. PMID 16775337.
- ↑ "The Thucydides syndrome: Ebola déjà vu? (or Ebola reemergent?)". Emerging Infect. Dis. 2 (2): 155–56. 1996. doi:10.3201/eid0202.960220. PMID 8964060.
- ↑ Scott, Susan and Duncan, Christopher. (2004). Return of the Black Death: The World's Greatest Serial Killer West Sussex; John Wiley and Sons. ISBN 0-470-09000-6.
- ↑ Briese, T.; Paweska, J.T.; McMullan, L.K.; Hutchison, S.K.; Street, C.; Palacios, G.; Khristova, M.L.; Weyer, J. et al. (2009). "Genetic Detection and Characterization of Lujo Virus, a New Hemorrhagic Fever–Associated Arenavirus from Southern Africa". PLOS Pathog 5 (5). doi:10.1371/journal.ppat.1000455. PMID 19478873.
- ↑ Woods 2005, p. 145
- ↑ Peters, C. (2000). "Are Hemorrhagic Fever Viruses Practical Agents for Biological Terrorism?". in Scheld, W. M.; Craig, W. A.; Hughes, J. M.. Emerging Infections. 4. Washington, D.C.: ASM Press. pp. 201–09. ISBN 978-1555811976. https://archive.org/details/emerginginfectio0004unse/page/201.
External links
- "Viral Haemorrhagic Fever". Public Health England (PHE). http://www.hpa.org.uk/infections/topics_az/VHF/menu.htm.
- "Viral Haemorrhagic Fevers". United Nations (UN). https://www.who.int/topics/haemorrhagic_fevers_viral/en/.
- "Viral Hemorrhagic Fevers (VHFs) Virus Families". U.S. Centers for Disease Control and Prevention (CDC). 2019-09-24. https://www.cdc.gov/vhf/virus-families/.
| Classification | |
|---|---|
| External resources |
 |
 KSF
KSF