Dengue fever history and symptoms
 From Wikidoc - Reading time: 5 min
From Wikidoc - Reading time: 5 min
|
Dengue Fever Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Dengue fever history and symptoms On the Web |
|
American Roentgen Ray Society Images of Dengue fever history and symptoms |
|
Risk calculators and risk factors for Dengue fever history and symptoms |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alonso Alvarado, M.D. [2]
Overview
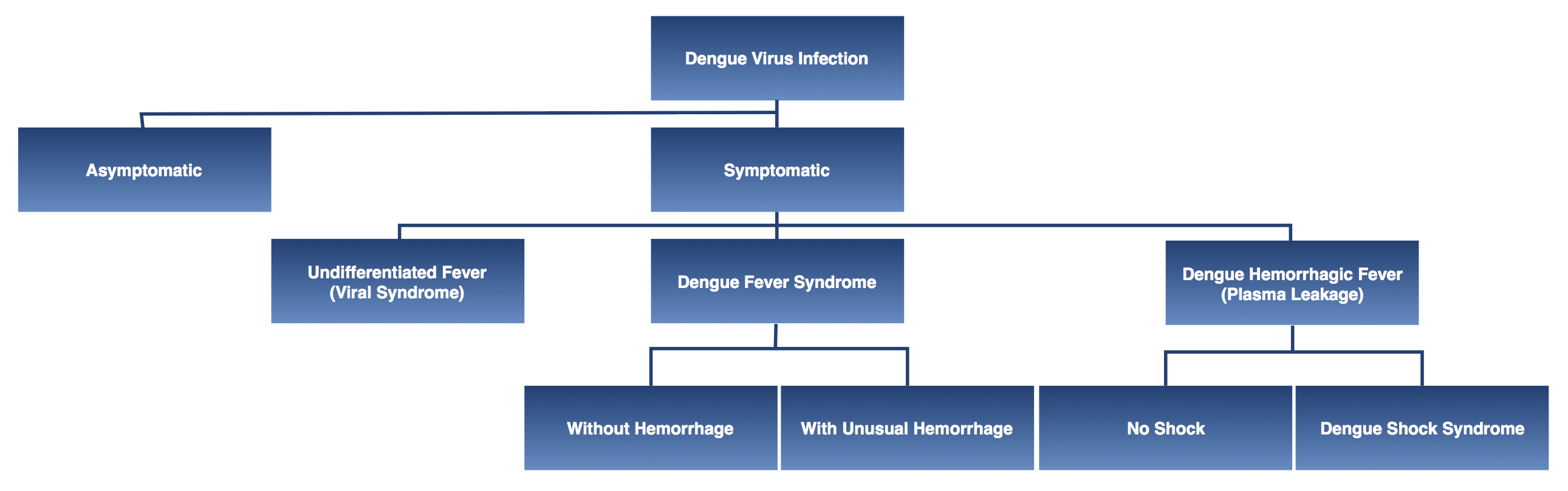
[edit | edit source]Dengue virus infection has a wide spectrum of clinical manifestations, ranging from asymptomic infection, to symptoms of non-severe disease (such as flu-like symptoms, fever, retro-orbital headache, fatigue, arthralgia, myalgia, nausea, vomiting, or lymphadenopathy), and to severe complications including signs of plasma leakage (such as pleural effusion or ascites), hemorrhagic tendencies (such as petechiae, ecchymoses, purpura, easy bruising at venipuncture sites, mucosal bleeding, gastrointestinal bleeding, hematemesis, or melena), and organ failure associated with shock.
History and Symptoms
[edit | edit source]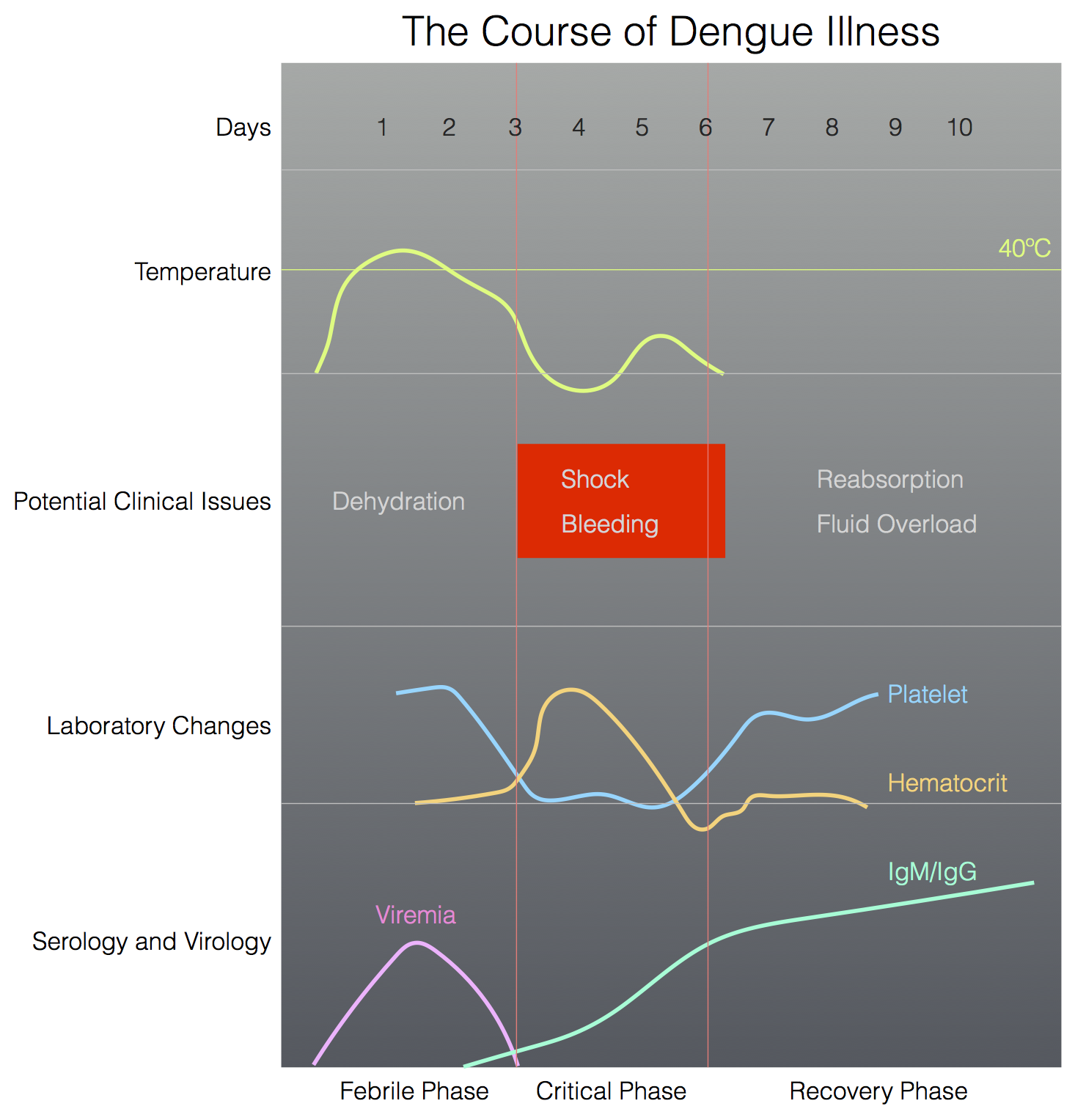 |
| Warning Signs Requiring Strict Observation and Medical Intervention |
|---|
|
| Complications in Febrile, Critical, and Recovery Phases of Dengue |
|
After an incubation period of 4–10 days, the illness begins abruptly and is followed by the three phases — the Febrile Phase, the Critical Phase, and the Recovery Phase.[2]
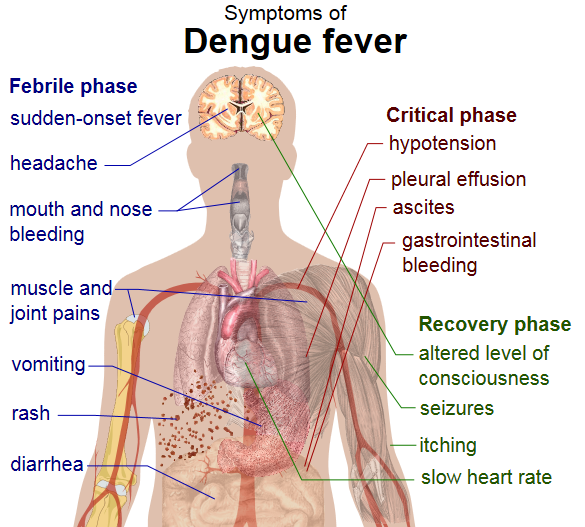
Febrile Phase
[edit | edit source]- The febrile phase is characterized by an abrupt onset of high fever which usually lasts 2–7 days, with a smaller peak at the trailing end of the fever (the so-called biphasic pattern). Accompanying symptoms include facial flushing, skin erythema, generalized body aches, myalgia, arthralgia, retro-orbital eye pain, photophobia, rubeliform exanthem and headache. The joint pain can be excruciating, hence the name breakbone fever or bonecrusher disease. Some patients may have sore throat, injected pharynx or conjunctiva, swollen lymph nodes, anorexia, nausea, or vomiting.
- Mild hemorrhagic manifestations such as petechiae and mucosal membrane bleeding (e.g. of the nose and gums) may be seen. Easy bruising and bleeding at venipuncture sites are present in some cases. The petechial rash usually appears first on the lower extremities and the chest and may spread to other parts of the body. Massive vaginal bleeding in women of childbearing age and gastrointestinal bleeding occur less commonly in this phase.[3] A positive tourniquet test in the febrile phase indicates an increased probability of dengue.[3][4]
- These clinical features do not predict the severity of dengue fever. Therefore, it is crucial to monitor for warning signs and other clinical parameters in order to recognize progression to the critical phase.
- The earliest abnormality in the complete blood count is leukopenia, which should alert the physician to a high probability of dengue. The platelet count usually begins to drop when the temperature is returning to normal.
- When no rash is present, mild symptoms of dengue fever may be misdiagnosed as influenza or other viral infection. Travelers from endemic areas may inadvertently pass on dengue in their home countries, having not been properly diagnosed at the height of their illness. Patients with dengue can only pass on the infection through mosquitoes or blood products while they are still febrile.
Critical Phase
[edit | edit source]- During the transition from the febrile to afebrile phase, patients without an increase in capillary permeability will improve without going through the critical phase. Instead of improving with the subsidence of fever, patients with increased capillary permeability may manifest with symptoms indicative of plasma leakage and enter what is termed the critical phase.
- The critical phase is heralded by the development of warning signs. These patients become worse around the time of defervescence, when the temperature drops to 37.5–38°C or less and remains below this level, usually on days 3 through 8 of the illness. Progressive leukopenia (≤5000 cells/mm3) with a rapid decline in platelet count to about 100,000 cells/mm3 typically precedes plasma leakage and the capillary leak syndrome.
- A rising hematocrit above baseline may be one of the earliest signs of plasma leakage. The extent of hemoconcentration reflects the severity of plasma leakage. However, this may be abated by early intravenous fluid administration. Frequent hematocrit determinations are essential for guiding intravenous fluid therapy. Pleural effusion and ascites may be clinically detectable only after intravenous fluid therapy, unless plasma leakage is significant.[5]
- In addition to plasma leakage, hemorrhagic manifestations such as easy bruising and bleeding at venipuncture sites occur frequently.
- Shock occurs when there is a dramatic volume loss due to plasma leakage. With profound and/or prolonged shock, tissue hypoperfusion results in metabolic acidosis, progressive organ impairment, and disseminated intravascular coagulation. This in turn leads to severe hemorrhage causing the hematocrit to decrease in severe shock. Rather than leukopenia, white cell count may increase as a stress response in patients with severe bleeding.
Recovery Phase
[edit | edit source]- As the patient survives the 24–48 hours of the critical phase, a gradual reabsorption of fluid from the extravascular compartment takes place in the following 48–72 hours. Appetite returns, gastrointestinal symptoms abate, hemodynamic status stabilizes, and diuresis ensues.
- Some patients have a confluent erythematous or petechial rash with small areas of normal skin termed as isles of white in the sea of red. Some may experience generalized pruritus. Bradycardia and other electrocardiographic changes are common during this stage.
- The hematocrit normalizes or may be lower than the baseline value due to hemodilution. The white cell count usually starts to rise soon after defervescence, while the recovery of the platelet count is typically delayed.
- Respiratory distress from massive pleural effusion and ascites, pulmonary edema, or congestive heart failure may occur during the recovery phase if excessive intravenous fluids have been administered.
 |
References
[edit | edit source]- ↑ "Dengue: guidelines for diagnosis, treatment, prevention and control" (PDF).
- ↑ Thong, Meow-Keong (1998). "Dengue shock syndrome and acute respiratory distress syndrome". The Lancet. 352 (9141): 1712. doi:10.1016/S0140-6736(05)61496-1. ISSN 0140-6736.
- ↑ 3.0 3.1 Kalayanarooj, S.; Vaughn, D. W.; Nimmannitya, S.; Green, S.; Suntayakorn, S.; Kunentrasai, N.; Viramitrachai, W.; Ratanachu‐eke, S.; Kiatpolpoj, S.; Innis, B. L.; Rothman, A. L.; Nisalak, A.; Ennis, F. A. (1997). "Early Clinical and Laboratory Indicators of Acute Dengue Illness". The Journal of Infectious Diseases. 176 (2): 313–321. doi:10.1086/514047. ISSN 0022-1899.
- ↑ Mayxay, Mayfong; Phetsouvanh, Rattanaphone; Moore, Catrin E; Chansamouth, Vilada; Vongsouvath, Manivanh; Sisouphone, Syho; Vongphachanh, Pankham; Thaojaikong, Thaksinaporn; Thongpaseuth, Soulignasack; Phongmany, Simmaly; Keolouangkhot, Valy; Strobel, Michel; Newton, Paul N. (2011). "Predictive diagnostic value of the tourniquet test for the diagnosis of dengue infection in adults". Tropical Medicine & International Health. 16 (1): 127–133. doi:10.1111/j.1365-3156.2010.02641.x. ISSN 1360-2276.
- ↑ Srikiatkhachorn, Anon; Krautrachue, Anchalee; Ratanaprakarn, Warangkana; Wongtapradit, Lawan; Nithipanya, Narong; Kalayanarooj, Siripen; Nisalak, Ananda; Thomas, Stephen J.; Gibbons, Robert V.; Mammen, Mammen P.; Libraty, Daniel H.; Ennis, Francis A.; Rothman, Alan L.; Green, Sharone (2007). "Natural History of Plasma Leakage in Dengue Hemorrhagic Fever". The Pediatric Infectious Disease Journal. 26 (4): 283–290. doi:10.1097/01.inf.0000258612.26743.10. ISSN 0891-3668.
- ↑ "Dengue haemorrhagic fever: diagnosis, treatment, prevention and control" (PDF).
 KSF
KSF