Mesenteric ischemia pathophysiology
 From Wikidoc - Reading time: 9 min
From Wikidoc - Reading time: 9 min
|
Mesenteric ischemia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Mesenteric ischemia pathophysiology On the Web |
|
American Roentgen Ray Society Images of Mesenteric ischemia pathophysiology |
|
Risk calculators and risk factors for Mesenteric ischemia pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Feham Tariq, MD [2]
Overview
[edit | edit source]The factors that regulate the intestinal blood flow play a vital role in the development of mesenteric ischemia. Mucosa of the intestines has high metabolic activity and therefore requires high blood flow. The majority of blood supply of the intestine comes from the superior mesenteric artery, with a collateral blood supply from superior and inferior pancreaticoduodenal arteries (branches of the celiac artery) as well as the inferior mesenteric artery. The splanchnic circulation (arteries supplying the viscera) receives 15-35% of the cardiac output, making it sensitive to the effects of decreased perfusion. Mesenteric ischemia occurs when intestinal blood supply is compromised by more than 50% of the original blood flow without activation of adaptive responses. This can lead to disruption of mucosal barrier, allowing the release of bacterial toxins (present in the intestinal lumen) and vasoactive mediators which ultimately lead to complete necrosis (cell death) of the intestinal mucosa. This can further progress to depression in myocardial activity, sepsis, multiorgan failure, and without prompt intervention, death.
Pathophysiology
[edit | edit source]Pathogenesis
[edit | edit source]- Intestinal mucosal damage occurs in response to ischemic insult.
- In response to providing protection from ischemia, mesenteric vessels undergo intrinsic autoregulation, which is an adaptive response to ischemia.
- In order to compensate for the ischemia, there is vasoconstriction of mesenteric vessels resulting in increased tissue oxygen extraction along with vasodilation of the collateral vessels. Owing to this mechanism, intestine is able to compensate for around 75% reduction in blood flow.[1][2][3][4][5][6]
Factors contributing in the pathogenesis of mesenteric ischemia:[7][8]
[edit | edit source]- Mesenteric blood supply (general circulation)
- Collateral circulation
- Response of mesenteric vasculature to ischemia
- Vasoactive and humoral factors
(A) Mesenteric blood supply (General circulation)
[edit | edit source]- The mesenteric circulation receives approximately 25% of the resting and 35% of the postprandial cardiac output.
- Mucosal and submucosal layers of the intestine receive 70% of the mesenteric blood flow, with the rest supplying the muscularis and serosal layers.
- The arterial supply of the intestine originates from three major arteries which include superior mesenteric artery, inferior mesenteric artery, and celiac artery:[9][10][7]
| Arterial supply | Region supplied |
|---|---|
| Superior mesenteric artery (SMA) | Small intestine, proximal and mid colon up to the splenic flexure. |
| Inferior mesenteric artery (IMA) | Hindgut starting from the splenic flexure to the rectum. |
| Celiac artery (CA) | Foregut, hepatobiliary system and spleen. |
| Venous drainage | |
| The venous system parallels the arterial branches and drains into the portal venous system. | |
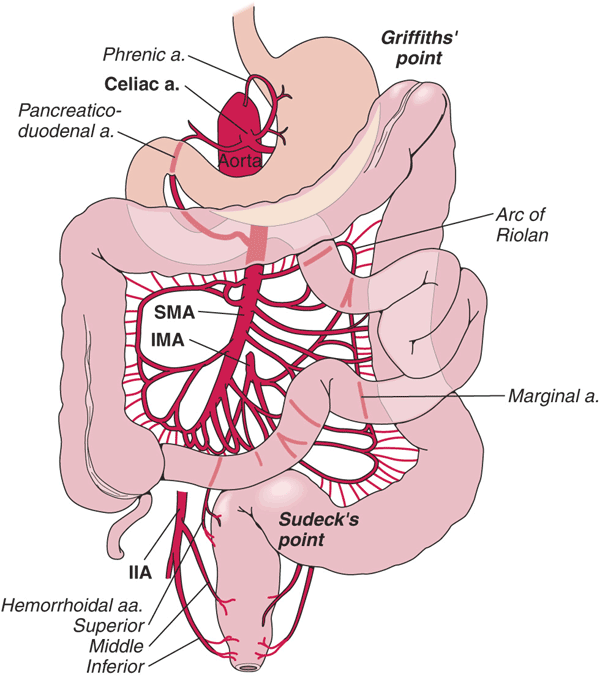
Source: By Anpol42 (Own work) [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)], via Wikimedia Commons
Commonly affected arteries:[11]
- Embolus can typically lodge into points of normal anatomic narrowing.
- This makes superior mesenteric artery the most vulnerable site because of its relatively larger diameter (more blood flow) and low take off angle (more likely to from the aorta.
- The majority of emboli lodge 3-10 cm distal to the origin of superior mesenteric artery, classically sparing the proximal jejunum and colon.
(B) Collateral circulation
[edit | edit source]The role of collateral circulation in the development of mesenteric ischemia is as follows:[12][13][14][15][16]
- Intestines receive collateral blood supply at all levels from the superior and inferior pancreaticoduodenal arteries, branches of the celiac artery, which provide protection from ischemia.
- These arteries can compensate for 75% reduction in mesenteric blood flow for up to 12 hours, without substanial injury.
- An extensive collateral circulation protects the intestines from transient periods of inadequate perfusion. However, prolonged reduction in splanchnic blood flow leads to vasoconstriction in the affected vascular bed, and eventually reduces collateral blood flow.
- The SMA and IMA communicate via the marginal artery of Drummond and the meandering mesenteric artery.
- Collateralization between the IMA and systemic circulation occurs in the rectum as the superior rectal (hemorrhoidal) vessels merge with the middle rectal vessels from the internal iliac arteries.
- The areas lacking this collateralization are prone to ischemia.
(C) Response of mesenteric vasculature to ischemia
[edit | edit source]- Mesenteric ischemia occurs when the blood supply to mesentery is reduced leading to disruption of cellular metabolism owing to oxygen and nutrient deficiency.[17][18]
- In the first 4 hours following ischemia, necrosis of the mucosal villi occurs.
- Persistent ischemia for more than 6 hours results in transmural, mural or mucosal infarction, ultimately leading to bowel perforation.
- Prolonged ischemia leads to progressive vasoconstriction of the mesenetric vessels which raises the pressure in them resulting in lowering the collateral flow.
- This is followed by vasodilation, trying to restore blood flow to the area of ischemic insult.
The sequence of events that take place in the small intestine subsequent to decreased blood flow:
[edit | edit source]
| Ischemic insult | |||||||||||||||||||
| Decreased delivery of oxygen and nutrients | |||||||||||||||||||
| Disruption in cellular metabolism | |||||||||||||||||||
| Tissue injury due to hypoxia and reperfusion | |||||||||||||||||||
| Full thickness necrosis of the bowel | |||||||||||||||||||
| Perforation of the bowel wall | |||||||||||||||||||
| Post ischemic cellular changes: | |
|---|---|
| Time duration since ischemia | Pathological changes in the small intestine |
| 3-4 hours | Necrosis of the mucosal villi |
| 6 hours | Transmural, mural or mucosal infarction |
| 1-4 days | Bowel hemorrhage |
Reperfusion injury:
- Restoration of blood flow to the area of ischemic insult results in reperfusion injury.
- This leads to release of oxygen free radicals, toxic byproducts of ischemic injury and neutrophil activation.
- Immune cells remove dead and damaged cells releasing cytokines such as TNF-alpha.
- Blood vessels become more permeable leading to edema of the small intestine.
- As the ischemia progresses from mucosa to all the layers beneath (transmural), it leads to breaks in the epithelial lining.
- This allows bacteria in the intestinal lumen to enter into the peritoneal cavity causing peritonitis.
- If bacteria enter into the blood stream, it results in systemic inflammatory response syndrome, which ultimately results in sepsis and septic shock.
(D) Vasoactive and humoral factors regulating the mesenteric blood flow
[edit | edit source]- Vasoactive and humoral factors control the regulation of vascular tone of mesenteric circulation in response to periods of stress such as systemic hypotension or postprandial state.
Intrinsic regulation:
(a) Metabolic factors:
- Reduction in blood supply to the mesentery causes adaptive changes in the splanchnic circulation.
- A discrepancy between tissue oxyegn demand and supply raises the concentration of local metabolites such as hydrogen, potassium, carbon dioxide, and adenosine, resulting in vasodilation, and hyperemia.
(b) Myogenic factors:
- Myogenic theory suggests that arteriolar wall tension receptors act to regulate vascular resistance in accordance with the transmural pressure.
- An acute decrease in perfusion pressure is compensated for by a reduction in arteriolar wall tension, thereby maintaining splanchnic blood flow.
Extrinsic regulation:
(a) Neural component:
[edit | edit source]- The extrinsic neural component of splanchnic circulatory regulation comprises the alpha-activated vasoconstrictor fibers.
- Intense activation of vasoconstrictor fibers through alpha-adrenergic stimulation results in vasoconstriction of small vessels and a decrease in mesenteric blood flow.
- After periods of prolonged alpha-adrenergic vasoconstriction, blood flow increases, presumably through β-adrenergic stimulation, which acts as a protective response.
- Although numerous types of neural stimulation (e.g. vagal, cholinergic, histaminergic, and sympathetic) can affect the blood supply of the gut, the adrenergic limb of the autonomic nervous system is the predominant neural influence on splanchnic circulation.
(b) Humoral component:
[edit | edit source]- Numerous endogenous and exogenous humoral factors affect the splanchnic circulation.
- Norepinephrine and high doses of epinephrine produce intense vasoconstriction by stimulating the adrenergic receptors.
- Other pharmacologic compounds that decrease splanchnic blood flow include:
- Low-dose dopamine causes splanchnic vasodilation, whereas higher doses lead to vasoconstriction by stimulating alpha adrenergic receptors.
- Exogenous agents that increase mesenteric blood flow include:
- In addition, numerous natural neurotransmitters can serve as splanchnic vasodilators, such as:
| Factors regulating mesenteric blood flow | |||
|---|---|---|---|
| Extrinsic reguatory system | |||
| Humoral (endogenous and exogenous) | Neural component | ||
| Decrease blood flow | Increase blood flow | Decrease blood flow | Increase blood flow |
|
|
|
|
| Intrinsic regulatory component | |||
| Decrease blood flow (Myogenic factors) | Increase blood flow (Metabolic factors) | ||
|
|||
Areas prone to ischemia
[edit | edit source]| Areas prone to ischemia | Blood supply |
|---|---|
| Splenic flexure | End arteries of superior mesenteric artery |
| Rectosigmoid junction | End arteries of inferior mesenteric artery |
| Middle segment of jejunum |
Watershed areas lacking collateralization:
[edit | edit source]- Splenic flexure
- Supplied by the end arteries of SMA with no collateral circulation.
- Rectosigmoid junction
- Supplied by the end arteries of IMA with no collateral circulation.
Pathogenesis of occlusive mesenteric ischemia:
[edit | edit source]
| Vascular occlusion | |||||||||||||||||||||||||||||||||||||||||||
| Blood flow<metabolic demand | |||||||||||||||||||||||||||||||||||||||||||
| Mucosal barrier disruption and bacterial translocation into the circulation | Anaerobic glycolysis in mucosa and lactate production | Activation of vascular and humoral factors leading to vasoconstriction | |||||||||||||||||||||||||||||||||||||||||
| Systemic activation of inflammatory response | Lactic acidosis | Intestinal necrosis | |||||||||||||||||||||||||||||||||||||||||
| Multiorgan failure | |||||||||||||||||||||||||||||||||||||||||||
Pathogenesis of non-occlusive mesenteric ischemia:
[edit | edit source]
| Hypovolemia | Cardiac failure | ||||||||||||||||||||||||||||||||||||||||||
| Endogenous vasoconstriction | |||||||||||||||||||||||||||||||||||||||||||
| Splanchnic vasoconstriction | |||||||||||||||||||||||||||||||||||||||||||
| Gut mucosal hypoperfusion | |||||||||||||||||||||||||||||||||||||||||||
| Restoration of blood by vasodilation of collaterals | Gut mucosal barrier disruption | ||||||||||||||||||||||||||||||||||||||||||
| Ischemia-reperfusion injury | Increased mucosal perfusion to bacterial toxins | ||||||||||||||||||||||||||||||||||||||||||
| Activation of inflammatory response | |||||||||||||||||||||||||||||||||||||||||||
Gross Pathology
[edit | edit source]Gross pathology shows following changes:
- Early stage of ischemia
- Late stage of ischemia
- Edematous, friable and hemorrhagic bowel wall.
Microscopic pathology
[edit | edit source]Mesenteric ischemia is classified histopathologically into five grades:[26]
- Grade 1. Normal. Vascular congestion is absent, and both the villous architecture and muscular layer are preserved.
- Grade 2. Villous architecture is preserved, with some mucosal congestion and dilated capillaries.
- Grade 3. There is congestion of mucosa with loss of superficial glandular architecture, but deep villous architecture is preserved.
- Grade 4. Muscular layer is preserved, but the mucosa is completely involved, with loss of all superficial and deep glandular architecture.
- Grade 5. There is total loss of glandular architecture, and the muscularis propria shows degeneration, fragmentation, and myocyte death, all of which indicate transmural infarction.
References
[edit | edit source]- ↑ Sánchez-Fernández P, Mier y Díaz J, Blanco-Benavides R (2000). "[Acute mesenteric ischemia. Profile of an aggressive disease]". Rev Gastroenterol Mex. 65 (3): 134–40. PMID 11464607.
- ↑ Savlania A, Tripathi RK (2017). "Acute mesenteric ischemia: current multidisciplinary approach". J Cardiovasc Surg (Torino). 58 (2): 339–350. doi:10.23736/S0021-9509.16.09751-2. PMID 27901324.
- ↑ Yasuhara H (2005). "Acute mesenteric ischemia: the challenge of gastroenterology". Surg Today. 35 (3): 185–95. doi:10.1007/s00595-004-2924-0. PMID 15772787 : 15772787 Check
|pmid=value (help). - ↑ Deitch, Edwin A. (2012). "Gut-origin sepsis: Evolution of a concept". The Surgeon. 10 (6): 350–356. doi:10.1016/j.surge.2012.03.003. ISSN 1479-666X.
- ↑ Kvietys PR, Granger DN (1982). "Relation between intestinal blood flow and oxygen uptake". Am J Physiol. 242 (3): G202–8. PMID 7065183.
- ↑ Granger DN, Granger HJ (1983). "Systems analysis of intestinal hemodynamics and oxygenation". Am J Physiol. 245 (6): G786–96. PMID 6660300.
- ↑ 7.0 7.1 Granger DN, Richardson PD, Kvietys PR, Mortillaro NA (1980). "Intestinal blood flow". Gastroenterology. 78 (4): 837–63. PMID 6101568.
- ↑ Rosenblum JD, Boyle CM, Schwartz LB (1997). "The mesenteric circulation. Anatomy and physiology". Surg Clin North Am. 77 (2): 289–306. PMID 9146713.
- ↑ Kumar S, Sarr MG, Kamath PS (2001). "Mesenteric venous thrombosis". N Engl J Med. 345 (23): 1683–8. doi:10.1056/NEJMra010076. PMID 11759648.
- ↑ Ha C, Magowan S, Accortt NA, Chen J, Stone CD (2009). "Risk of arterial thrombotic events in inflammatory bowel disease". Am J Gastroenterol. 104 (6): 1445–51. doi:10.1038/ajg.2009.81. PMID 19491858.
- ↑ Wyers, Mark C. (2010). "Acute Mesenteric Ischemia: Diagnostic Approach and Surgical Treatment". Seminars in Vascular Surgery. 23 (1): 9–20. doi:10.1053/j.semvascsurg.2009.12.002. ISSN 0895-7967.
- ↑ McKinsey JF, Gewertz BL (1997). "Acute mesenteric ischemia". Surg Clin North Am. 77 (2): 307–18. PMID 9146714.
- ↑ Walker TG (2009). "Mesenteric vasculature and collateral pathways". Semin Intervent Radiol. 26 (3): 167–74. doi:10.1055/s-0029-1225663. PMC 3036491. PMID 21326561.
- ↑ Fisher DF, Fry WJ (1987). "Collateral mesenteric circulation". Surg Gynecol Obstet. 164 (5): 487–92. PMID 3554567.
- ↑ Bulkley GB, Womack WA, Downey JM, Kvietys PR, Granger DN (1985). "Characterization of segmental collateral blood flow in the small intestine". Am J Physiol. 249 (2 Pt 1): G228–35. PMID 4025549.
- ↑ Bulkley GB, Womack WA, Downey JM, Kvietys PR, Granger DN (1986). "Collateral blood flow in segmental intestinal ischemia: effects of vasoactive agents". Surgery. 100 (2): 157–66. PMID 3738747 : 3738747 Check
|pmid=value (help). - ↑ Mastoraki A, Mastoraki S, Tziava E, Touloumi S, Krinos N, Danias N; et al. (2016). "Mesenteric ischemia: Pathogenesis and challenging diagnostic and therapeutic modalities". World J Gastrointest Pathophysiol. 7 (1): 125–30. doi:10.4291/wjgp.v7.i1.125. PMC 4753178. PMID 26909235.
- ↑ Corcos, Olivier; Nuzzo, Alexandre (2013). "Gastro-Intestinal Vascular Emergencies". Best Practice & Research Clinical Gastroenterology. 27 (5): 709–725. doi:10.1016/j.bpg.2013.08.006. ISSN 1521-6918.
- ↑ Hansen MB, Dresner LS, Wait RB (1998). "Profile of neurohumoral agents on mesenteric and intestinal blood flow in health and disease". Physiol Res. 47 (5): 307–27. PMID 10052599.
- ↑ Schoenberg MH, Beger HG (1993). "Reperfusion injury after intestinal ischemia". Crit Care Med. 21 (9): 1376–86. PMID 8370303.
- ↑ Patel, Amit; Kaleya, Ronald N.; Sammartano, Robert J. (1992). "Pathophysiology of Mesenteric Ischemia". Surgical Clinics of North America. 72 (1): 31–41. doi:10.1016/S0039-6109(16)45626-4. ISSN 0039-6109.
- ↑ Takala J (1996). "Determinants of splanchnic blood flow". Br J Anaesth. 77 (1): 50–8. PMID 8703630.
- ↑ Granger HJ, Norris CP (1980). "Intrinsic regulation of intestinal oxygenation in the anesthetized dog". Am J Physiol. 238 (6): H836–43. PMID 7386643.
- ↑ Granger HJ, Shepherd AP (1973). "Intrinsic microvascular control of tissue oxygen delivery". Microvasc Res. 5 (1): 49–72. PMID 4684756.
- ↑ Cappell MS (1998). "Intestinal (mesenteric) vasculopathy. I. Acute superior mesenteric arteriopathy and venopathy". Gastroenterol Clin North Am. 27 (4): 783–825, vi. PMID 9890114.
- ↑ Rosow DE, Sahani D, Strobel O, Kalva S, Mino-Kenudson M, Holalkere NS; et al. (2005). "Imaging of acute mesenteric ischemia using multidetector CT and CT angiography in a porcine model". J Gastrointest Surg. 9 (9): 1262–74, discussion 1274-5. doi:10.1016/j.gassur.2005.07.034. PMC 3807105. PMID 16332482.
 KSF
KSF