Rosacea
 From Wikidoc - Reading time: 9 min
From Wikidoc - Reading time: 9 min
| Rosacea | |
 | |
|---|---|
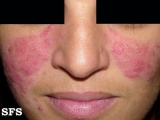
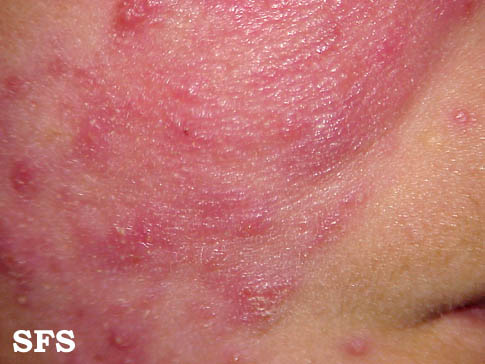
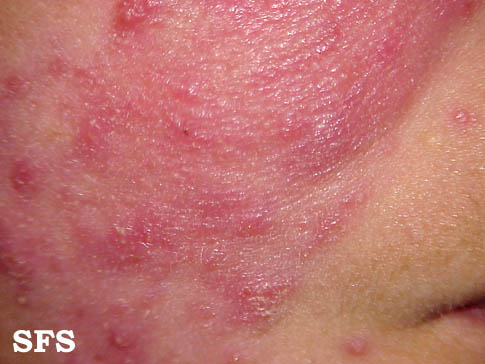
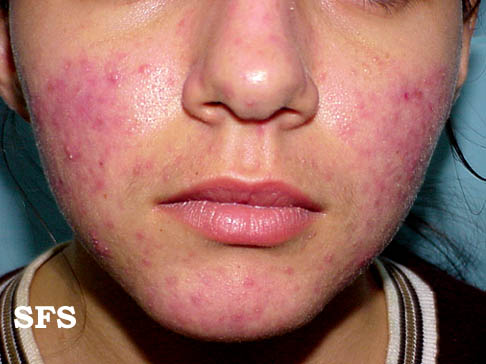
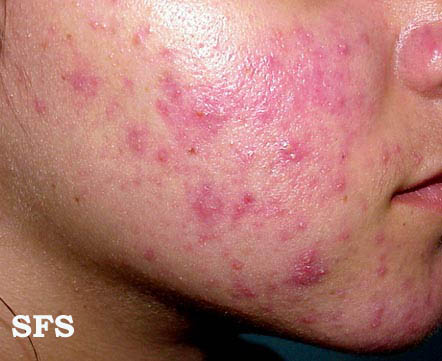
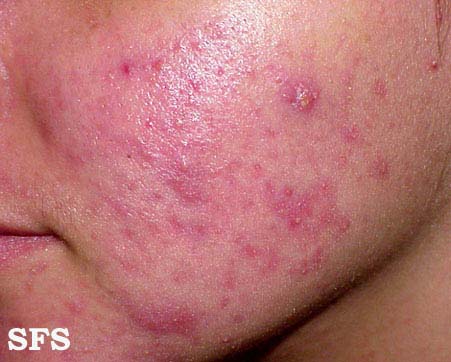
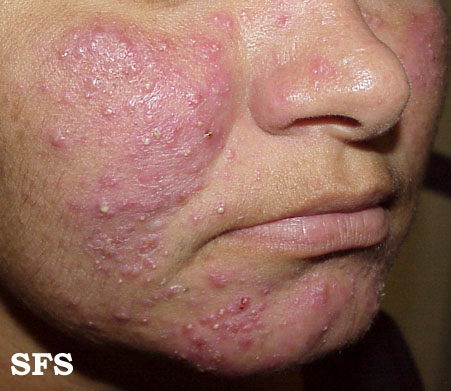
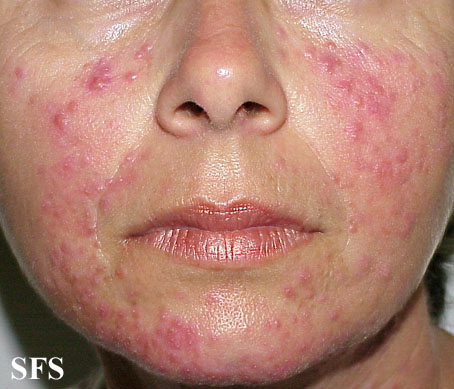
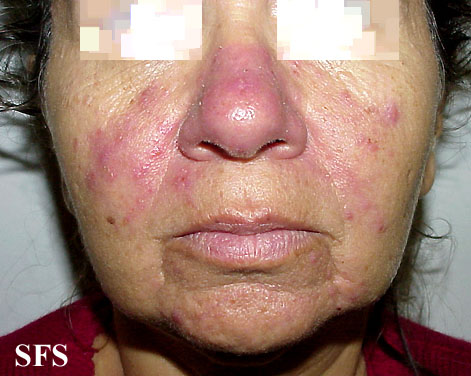
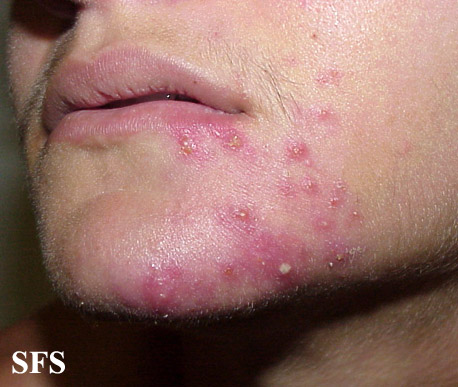
| Moderate erythematotelangiectatic and mild papulopustular rosacea. | |
| ICD-10 | L71 |
| ICD-9 | 695.3 |
| DiseasesDB | 96 |
| MedlinePlus | 000879 |
| eMedicine | derm/377 |
|
WikiDoc Resources for Rosacea |
|
Articles |
|---|
|
Most recent articles on Rosacea |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Rosacea at Clinical Trials.gov Clinical Trials on Rosacea at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Rosacea
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Directions to Hospitals Treating Rosacea Risk calculators and risk factors for Rosacea
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Rosacea |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Kiran Singh, M.D. [2]
Overview
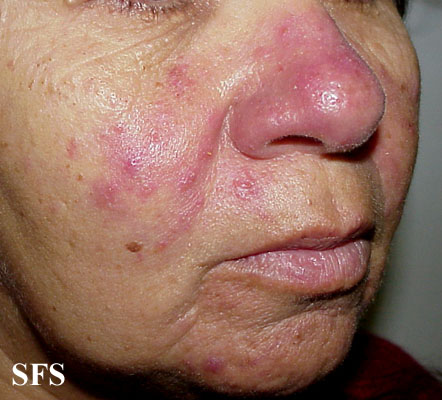
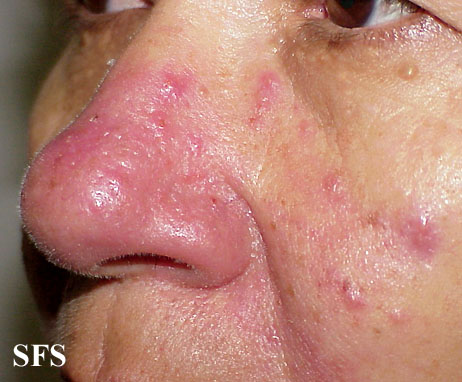
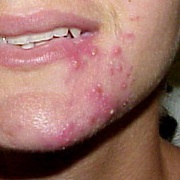
[edit | edit source]Rosacea (Template:IPAEng) is a common but often misunderstood condition that is estimated to affect over 45 million people worldwide. It affects white-skinned people of mostly north-western European descent, and has been nicknamed the 'curse of the Celts' by some in Ireland. It begins as erythema (flushing and redness) on the central face and across the cheeks, nose, or forehead but can also less commonly affect the neck and chest. As rosacea progresses, other symptoms can develop such as semi-permanent erythema, telangiectasia (dilation of superficial blood vessels on the face), red domed papules (small bumps) and pustules, red gritty eyes, burning and stinging sensations, and in some advanced cases, a red lobulated nose (rhinophyma). The disorder can be confused and co-exist with acne vulgaris and/or seborrheic dermatitis. Rosacea affects both sexes, but is almost three times more common in women, and has a peak age of onset between 30 and 60. The presence of rash on the scalp or ears suggests a different or co-existing diagnosis, as rosacea is primarily a facial diagnosis.
Subtypes and symptoms
[edit | edit source]There are four identified rosacea subtypes[1] and patients may have more than one subtype present.
- Erythematotelangiectatic rosacea: Permanent redness (erythema) with a tendency to flush and blush easily. It is also common to have small blood vessels visible near the surface of the skin (telangiectasias) and possibly burning or itching sensations.
- Papulopustular rosacea: Some permanent redness with red bumps (papules) with some pus filled (pustules) (which typically last 1-4 days); this subtype can be easily confused with acne.
- Phymatous rosacea: This subtype is most commonly associated with rhinophyma, an enlargement of the nose. Symptoms include thickening skin, irregular surface nodularities, and enlargement. Phymatous rosacea can also affect the chin (gnatophyma), forehead (metophyma), cheeks, eyelids (blepharophyma), and ears (otophyma).[2] Small blood vessels visible near the surface of the skin (telangiectasias) may be present.
- Ocular rosacea: Red, dry and irritated eyes and eyelids. Some other symptoms include foreign body sensations, itching and burning.
-
Opthalmic rosacea. Adapted from Dermatology Atlas.[3]
-
Opthalmic rosacea. Adapted from Dermatology Atlas.[3]
-
Opthalmic rosacea. Adapted from Dermatology Atlas.[3]
There have been other descriptive terms applied to presentations of rosacea, but these are not formally accepted as subtyes of rosacea:[4]
- Granulomatous rosacea.[5]
- The rare and severely scarring Rosacea fulminans (pyoderma faciale) occurring exclusively in women after adolescence and most commonly in their early 20s,[6][7]
- Perioral dermatitis, which is better described as periorificial dermatitis, but similarly treated with topical metronidazole.[8]
- Persistent edema of rosacea.[citation needed]
- Rosacea Conglobata.[citation needed]
- Persisting redness and oedema of the upper half of the face has been termed Morbihan disease.[9][10]
Rosacea sufferers often report periods of depression stemming from cosmetic disfigurement, painful burning sensations, and decreases in quality of life.[11]
Causes
[edit | edit source]Richard L. Gallo and colleagues recently noticed that patients with rosacea had elevated levels of the peptide cathelicidin and elevated levels of stratum corneum tryptic enzymes (SCTEs). Antibiotics have been used in the past to treat rosacea, but antibiotics may only work because they inhibit some SCTEs. See the August 5, 2007 issue of Nature Medicine for details.
Rosacea has a hereditary component and those that are fair-skinned of European or Celtic ancestry have a higher genetic predisposition to developing it. Women are more commonly affected but when men develop rosacea it tends to be more severe. People of all ages can get rosacea but there is a higher instance in the 30-50 age group. The first signs of rosacea are said to be persisting redness due to exercise, changes in temperature, and cleansing.
Triggers that cause episodes of flushing and blushing play a part in the development of rosacea. Exposure to temperature extremes can cause the face to become flushed as well as strenuous exercise, heat from sunlight, severe sunburn, stress, anxiety, cold wind, moving to a warm or hot environment from a cold one such as heated shops and offices during the winter. There are also some foods and drinks that can trigger flushing, these include alcohol, foods and beverages containing caffeine (especially, hot tea and coffee), foods high in histamines and spicy food, as well as fruits containing high levels of antioxidants, such as red grapes.
Certain medications and topical irritants can quickly progress rosacea. If redness persists after using a treatment then it should be stopped immediately. Some acne and wrinkle treatments that have been reported to cause rosacea include microdermabrasion, chemical peels, high dosages of isotretinoin, benzoyl peroxide and tretinoin. Steroid induced rosacea is the term given to rosacea caused by the use of topical or nasal steroids. These steroids are often prescribed for seborrheic dermatitis. Dosage should be slowly decreased and not immediately stopped to avoid a flare up.
Studies of rosacea and demodex mites have revealed that some people with rosacea have increased numbers of the mite, especially those with steroid induced rosacea.[12] When large numbers are present they may play a role along with other triggers. On other occasions Demodicidosis (Mange) is a separate condition that may have "rosacea-like" appearances.[13]
It has also been suggested that rosacea might be a neurological disorder resulting from hypersensitization of sensory neurons following activation of the plasma kallikrein-kinin system by exposure to intestinal bacteria in the digestive tract.[14]
Physical Examination
[edit | edit source]Gallery
[edit | edit source]-
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6 -
Acne rosacea.
Adapted from [http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=6
Treatments
[edit | edit source]Treating rosacea varies from patient to patient depending on severity and subtypes. Dermatologists are recommended to take a subtype-directed approach to treating rosacea patients.[15]
Trigger avoidance can help reduce the onset of rosacea but alone will not normally cause remission for all but mild cases. The National Rosacea Society recommends that a diary be kept to help identify and reduce triggers.
It is important to have a gentle skin cleansing regimen using non-irritating cleansers. Protection from the sun is important and daily use of a sunscreen of at least SPF 15 containing a physical blocker such as zinc oxide or titanium dioxide is advised although chemical sunscreens, if non-irritating to the skin, are also an option.
Oral tetracycline antibiotics (tetracycline, doxycycline, minocycline) and topical antibiotics such as metronidazole are usually the first line of defense prescribed by doctors to relieve papules, pustules, inflammation and some redness.[16] Topical Azelaic acid such as Finacea maya help reduce inflammation. Oral antibiotics may help to relieve symptoms of ocular rosacea. If papules and pustules persist, then sometimes isotretinoin can be prescribed.[17] Isotretinoin has many side effects and is normally used to treat severe acne but in low dosages is proven to be effective against papulopustular and phymatous rosacea.
The treatment of flushing and blushing has been attempted by means of the centrally acting α-2 agonist clonidine, but there is no evidence whatsoever that this is of any benefit. The same is true of the beta-blockers nadolol and propanolol. If flushing occurs with red wine consumption, then complete avoidance helps. There is no evidence at all that antihistamines are of any benefit in rosacea.
People who develop infections of the eyelids must practice frequent eyelid hygiene. Daily scrubbing the eyelids gently with diluted baby shampoo or an over-the-counter eyelid cleaner and applying warm (but not hot) compresses several times a day is recommended.
Dermatological vascular laser (single wavelength) or Intense Pulsed Light (broad spectrum) machines offer one of the best treatments for rosacea, in particular the erythema (redness) of the skin.[18] They use light to penetrate the epidermis to target the capillaries in the dermis layer of the skin. The light is absorbed by oxy-hemoglobin which heat up causing the capillary walls to heat up to 70ºC, damaging them, causing them to be absorbed by the body's natural defence mechanism.
CO2 lasers can be used to remove excess tissue caused by phymatous rosacea. CO2 lasers emit a wavelength that is absorbed directly by the skin. The laser beam can be focused into a thin beam and used as a scalpel or defocused and used to vaporise tissue. Low level light therapies have also been used to treat rosacea. One alternative skin treatment, fashionable in the Victorian and Edwardian eras, was Sulphur. Recently Sulphur has re-gained some credibility as a safe alternative to steroids and coal tar.
Antibiotic Regimen
[edit | edit source]- Acne rosacea [19]
- 1. Facial erythema
- Preferred regimen: Brimonidine gel Topical bid, applied to the affected area
- 2. Papulopustular rosacea
- Preferred regimen (1): Azelaic acid gel Topical bid
- Preferred regimen (2): Metronidazole cream Topical qd
Famous people
[edit | edit source]Famous people with Rosacea include:
- Bill Clinton.[20]
- J. P. Morgan
- Diana, Princess of Wales[21]
- W. C. Fields
- Alex Ferguson
- Rosie O'Donnell[22]
- Mariah Carey[23]
- Margaret Bobonich[24]
- Ricky Wilson[25]
- Lisa Faulkner[26]
- Davina Wong
- Rembrandt[27]
See also
[edit | edit source]- Acne Vulgaris
- Seborrheic dermatitis
- Keratosis pilaris
- Demodicosis a rash caused by the Demodex mite that may have rosacea-like appearances.[13]
Footnotes
[edit | edit source]- ↑ Wilkin J, Dahl M, Detmar M, Drake L, Liang MH, Odom R, Powell F (2004). "Standard grading system for rosacea: report of the National Rosacea Society Expert Committee on the classification and staging of rosacea" (PDF reprint). J Am Acad Dermatol. 50 (6): 907–12. PMID 15153893.
- ↑ Jansen T, Plewig G (1998). "Clinical and histological variants of rhinophyma, including nonsurgical treatment modalities". Facial Plast Surg. 14 (4): 241–53. PMID 11816064.
- ↑ 3.0 3.1 3.2 "Dermatology Atlas".
- ↑ Wilkin J, Dahl M, Detmar M, Drake L, Feinstein A, Odom R, Powell F (2002). "Standard classification of rosacea: Report of the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea" (PDF reprint). J Am Acad Dermatol. 46: 584–7. PMID 15153893. - this earlier classification noted terms of Granulomatous Rosacea, Rosacea fulminans and Perioral dermatitis as probably not meeting the accepted definitions for Rosacea. Such terms not mentioned in the later 2004 classification.
- ↑ Helm K, Menz J, Gibson L, Dicken C (1991). "A clinical and histopathologic study of granulomatous rosacea". J Am Acad Dermatol. 25 (6 Pt 1): 1038–43. PMID 1839796.
- ↑ Jansen T, Plewig G, Kligman A (1994). "Diagnosis and treatment of rosacea fulminans". Dermatology. 188 (4): 251–4. PMID 8193395.
- ↑ Helm T, Schechter J (2006). "Biopsy may help identify early pyoderma faciale (rosacea fulminans)". Cutis. 77 (4): 225–7. PMID 16706239.
- ↑ Nguyen V, Eichenfield L (2006). "Periorificial dermatitis in children and adolescents". J Am Acad Dermatol. 55 (5): 781–5. PMID 17052482.
- ↑ Hölzle E, Jansen T, Plewig G (1995). "[Morbihan disease--chronic persistent erythema and edema of the face]". Hautarzt. 46 (11): 796–8. PMID 8641887.
- ↑ Landow K (2002). "Unraveling the mystery of rosacea -- Keys to getting the red out". Postgraduate Medicine. 112 (6). Unknown parameter
|month=ignored (help) - ↑ Panconesi, E. (1984). "Psychosomatic dermatology". Clin Dermatol. 2: 94–179. PMID 6242532.
- ↑ Erbagcaronci Z, Özgöztascedili O (1998). "The significance of Demodex folliculorum density in rosacea". Int J Dermatol. 37 (6): 421–5. doi:10.1046/j.1365-4362.1998.00218.x. PMID 9646125. Unknown parameter
|month=ignored (help) - ↑ 13.0 13.1 Baima B, Sticherling M (2002). "Demodicidosis revisited". Acta Derm Venereol. 82 (1): 3–6. PMID 12013194.
- ↑ Kendall SN (2004). "Remission of rosacea induced by reduction of gut transit time". Clin Exp dermatol. 29 (3): 297–9. doi:10.1111/j.1365-2230.2004.01461.x. PMID 15115515. Unknown parameter
|month=ignored (help) - ↑ Aaron F. Cohen, MD, and Jeffrey D. Tiemstra, MD (2002). "Diagnosis and treatment of rosacea". J Am Board Fam Pract. 15 (3): 214–7. PMID 12038728. Unknown parameter
|month=ignored (help) - ↑ Dahl MV, Katz HI, Krueger GG, Millikan LE, Odom RB, Parker F, Wolf JE Jr, Aly R, Bayles C, Reusser B, Weidner M, Coleman E, Patrignelli R, Tuley MR, Baker MO, Herndon JH Jr, Czernielewski JM (1998). "Topical metronidazole maintains remissions of rosacea". Arch Dermatol. 134 (6): 679–83. PMID 9645635. Unknown parameter
|month=ignored (help) - ↑ Hoting E, Paul E, Plewig G (1986). "Treatment of rosacea with isotretinoin". Int J Dermatol. 25 (10): 660–3. PMID 2948928. Unknown parameter
|month=ignored (help) - ↑ Marla C Angermeier (1999). "Treatment of facial vascular lesions with intense pulsed light". J Cutan Laser Ther. 1 (2): 95–100. PMID 11357295.
- ↑ Gilbert, David (2015). The Sanford guide to antimicrobial therapy. Sperryville, Va: Antimicrobial Therapy. ISBN 978-1930808843.
- ↑ Jane E. Brody (March 16, 2004). "Sometimes Rosy Cheeks Are Just Rosy Cheeks". New York Times.
- ↑ http://www.metrogel.com/CopingWithRosacea/CopingWithRosacea.aspx
- ↑ http://www.elle.com/featurefullstory/11455/rosie-odonnell-page3.html
- ↑ http://women.timesonline.co.uk/tol/life_and_style/women/fashion/article1390492.ece
- ↑ http://www.pharmalive.com/News/Index.cfm?articleid=433576
- ↑ http://observer.guardian.co.uk/omm/qanda/story/0,,1550882,00.html
- ↑ http://www.nowmagazine.co.uk/body/celeb_health/Lisa_Faulkner_My_unslightly_rosacea_article_118152.html
- ↑ http://www.about-rosacea.com/famous.htm
External links
[edit | edit source]- Researchers discover cause of rosacea
- Directory of rosacea organisations and websites
- National Rosacea Society (U.S.)
- Rosacea photo library at Dermnet
- Rosacea Research & Development Instititute (U.S.)
- Rosacea Support Group
- Physician Discussion Forum for Rosacea
bg:Розацея de:Rosazea it:Acne rosacea nl:Rosacea no:Rosacea sl:Kuperoza fi:Ruusufinni sv:Rosacea
 KSF
KSF![Opthalmic rosacea. Adapted from Dermatology Atlas.[3]](https://www.wikidoc.org/images/d/df/Opthalmic_rosacea02.jpg)
![Opthalmic rosacea. Adapted from Dermatology Atlas.[3]](https://www.wikidoc.org/images/c/cd/Opthalmic_rosacea03.jpg)