smoke
Topic: Sandbox
 From Wikidoc - Reading time: 8 min
From Wikidoc - Reading time: 8 min
Template:Smoking cessation Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Seyedmahdi Pahlavani, M.D. [2],Usama Talib, BSc, MD [3],Aravind Kuchkuntla, M.B.B.S[4]
Overview
[edit | edit source]Tobacco use is the leading cause of preventable disease, disability, and death in the United States. Each year, nearly half a million Americans die prematurely of smoking or exposure to secondhand smoke and 16 million live with a serious illness caused by smoking. Smoking can cause repairable damage to various organs including the heart, lungs, kidneys, stomach and intestines. Smoking is associated with the causation of various cancers in the humans. Quitting smoking cuts cardiovascular risks, reduces risk for stroke to about half that of a nonsmoker’s, reduces risks for cancers of the mouth, throat, esophagus, and bladder by half within 5 years and ten years after quitting smoking, the risk for lung cancer drops by half. Smoking cessation can be achieved by some general, non-pharmacological and pharmacological strategies.
Epidemiology
[edit | edit source]- Tobacco use is the leading cause of preventable disease, disability, and death in the United States, accounting for more than 480,000 deaths every year, or 1 of every 5 deaths.[1]
- In 2015, about 15 of every 100 U.S. adults aged 18 years or older (15.1%) currently smoked cigarettes, this means an estimated 36.5 million adults in the United States currently smoke cigarettes.
- Current smoking has declined from nearly 21 of every 100 adults (20.9%) in 2005 to about 15 of every 100 adults (15.1%) in 2015.
- Nearly 40 million US adults still smoke cigarettes, and about 4.7 million middle and high school students use at least one tobacco product, including e-cigarettes.
- Every day, more than 3,800 youth younger than 18 years smoke their first cigarette.
- Each year, nearly half a million Americans die prematurely of smoking or exposure to secondhand smoke and more than 16 million Americans live with a smoking-related disease.
- Each year, the United States spends nearly $170 billion on medical care to treat smoking-related disease in adults.
The epidemiology of the current smoking status based on different descriptive characteristics is as follows:
Gender
[edit | edit source]- Nearly 17 of every 100 adult men (16.7%).
- More than 13 of every 100 adult women (13.6%).
Age
[edit | edit source]- 13 of every 100 adults aged 18–24 years (13.0%).
- Nearly 18 of every 100 adults aged 25–44 years (17.7%)
- 17 of every 100 adults aged 45–64 years (17.0%).
- More than 8 of every 100 adults aged 65 years and older (8.4%).
Race
[edit | edit source]- Nearly 22 of every 100 non-Hispanic American Indians/Alaska Natives (21.9%).
- More than 20 of every 100 non-Hispanic multiple race individuals (20.2%).
- Nearly 17 of every 100 non-Hispanic Blacks (16.7%).
- More than 16 of every 100 non-Hispanic Whites (16.6%).
- More than 10 of every 100 Hispanics (10.1%).
- 7 of every 100 non-Hispanic Asians* (7.0%).
Education
[edit | edit source]- More than 24 of every 100 adults with 12 or fewer years of education (no diploma) (24.2%).
- About 34 of every 100 adults with a GED certificate (34.1%).
- Nearly 20 of every 100 adults with a high school diploma (19.8%).
- More than 18 of every 100 adults with some college (no degree) (18.5%).
- More than 16 of every 100 adults with an associate's degree (16.6%).
- More than 7 of every 100 adults with an undergraduate college degree (7.4%).
- More than 3 of every 100 adults with a graduate degree (3.6%).
Socio-economic status
[edit | edit source]- About 26 of every 100 adults who live below the poverty level (26.1%).
- Nearly 14 of every 100 adults who live at or above the poverty level (13.9%).
Geographical Area
[edit | edit source]- Nearly 19 of every 100 adults who live in the Midwest (18.7%).
- More than 15 of every 100 adults who live in the South (15.3%).
- More than 13 of every 100 adults who live in the Northeast (13.5%).
- More than 12 of every 100 adults who live in the West (12.4%).
Disability
[edit | edit source]- More than 21 of every 100 adults who reported having a disability/limitation (21.5%)
- Nearly 14 of every 100 adults who reported having no disability/limitation (13.8%)
Sexual Orientation
[edit | edit source]- More than 20 of every 100 lesbian/gay/bisexual adults (20.6%)
- Nearly 15 of every 100 straight adults (14.9%)
Adult Smokers Distribution
[edit | edit source]The distribution of smokers in the US can be depicted by this picture.[2]

Smoking and Health
[edit | edit source]The impact of smoking on the health can be summarized as follows:[3][4][5]
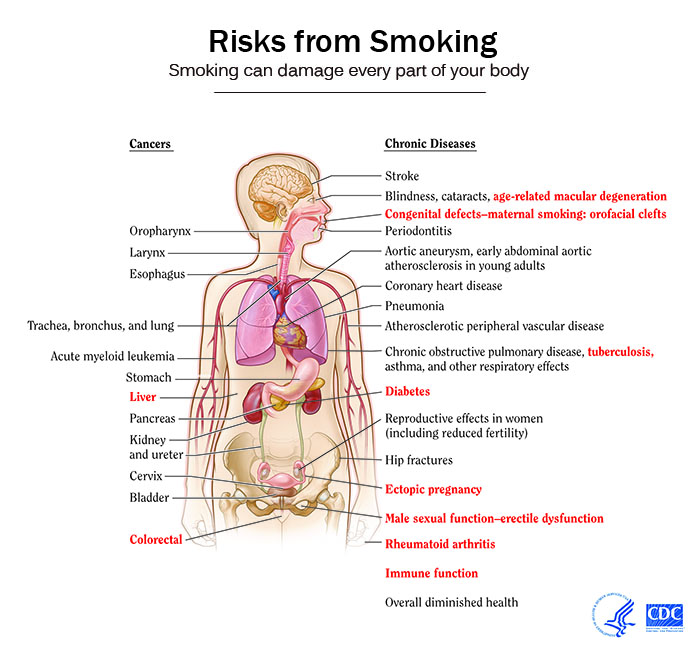
Death due to Smoking
[edit | edit source]- Cigarette smoking is the leading preventable cause of death in the United States.
- It causes more than 480,000 deaths each year in the United States. This is nearly one in five deaths.
- Cigarette smoking increases risk for death from all causes in men and women.
- The risk of dying from cigarette smoking has increased over the last 50 years in the U.S.
- 80% of all the deaths as a result of chronic obstructive pulmonary disease (COPD) are due to smoking.
Other Health Risks
[edit | edit source]Smoking has shown to increases the risk of:
- Coronary heart disease by 2 to 4 times
- Stroke by 2 to 4 times
- Men developing lung cancer by 25 times
- Women developing lung cancer by 25.7 times
Smoking causes diminished overall health, increased absenteeism from work, and increased health care utilization and cost
Smoking and Cardiovascular Disease
[edit | edit source]- Smoking causes stroke and coronary heart disease, which are among the leading causes of death in the United States.
- Even people who smoke fewer than five cigarettes a day can have early signs of cardiovascular disease.
- Smoking damages blood vessels and can make them thicker and grow narrower.
- A stroke may result when:
- A clot blocks the blood flow to part of your brain
- A blood vessel in or around your brain bursts
- Blockages caused by smoking can also diminish the blood flow to the legs and the skin.
Smoking and Respiratory Disease
[edit | edit source]Smoking can cause lung disease by damaging your airways and the small air sacs (alveoli) found in your lungs.
- Lung diseases caused by smoking include COPD, which includes emphysema and chronic bronchitis.
- Cigarette smoking causes most cases of lung cancer.
- If you have asthma, tobacco smoke can trigger an attack or make an attack worse.
- Smokers are 12 to 13 times more likely to die from COPD than nonsmokers.
Smoking and Cancer
[edit | edit source]Smoking can cause cancer almost anywhere in your body:
- Bladder
- Blood (acute myeloid leukemia)
- Cervix
- Colon and rectum (colorectal)
- Esophagus
- Kidney and ureter
- Larynx
- Liver
- Oropharynx (includes parts of the throat, tongue, soft palate, and the tonsils)
- Pancreas
- Stomach
- Trachea, bronchus, and lung
- Smoking also increases the risk of dying from cancer and other diseases in cancer patients and survivors.
- If nobody smoked, one of every three cancer deaths in the United States would not occur.
Other Health Risks due to Smoking
[edit | edit source]Smoking harms nearly every organ of the body and affects a person’s overall health.Smoking can make it harder for a woman to become pregnant. It can also affect her baby’s health before and after birth. Smoking increases risks for:
- Preterm (early) delivery
- Stillbirth (death of the baby before birth)
- Low birth weight
- Sudden infant death syndrome (known as SIDS or crib death)
- Ectopic pregnancy
- Orofacial clefts in infants
- Smoking can also affect men’s sperm, which can reduce fertility and also increase risks for birth defects and miscarriage.
- Smoking can affect bone health.
- Women past childbearing years who smoke have weaker bones than women who never smoked. They are also at greater risk for broken bones.
- Smoking affects the health of your teeth and gums and can cause tooth loss.
- Smoking can increase your risk for cataracts (clouding of the eye’s lens that makes it hard for you to see). It can also cause age-related macular degeneration (AMD). AMD is damage to a small spot near the center of the retina, the part of the eye needed for central vision.
- Smoking is a cause of type 2 diabetes mellitus and can make it harder to control. The risk of developing diabetes is 30–40% higher for active smokers than nonsmokers.
- Smoking causes general adverse effects on the body, including inflammation and decreased immune function.
- Smoking is a cause of rheumatoid arthritis.
Effect of Smoking Cessation on various Risks
[edit | edit source]- Quitting smoking cuts cardiovascular risks. Just 1 year after quitting smoking, your risk for a heart attack drops sharply.
- Within 2 to 5 years after quitting smoking, your risk for stroke may reduce to about that of a nonsmoker’s.
- If you quit smoking, your risks for cancers of the mouth, throat, esophagus, and bladder drop by half within 5 years.
- Ten years after you quit smoking, your risk for lung cancer drops by half.
Smoking cessation
[edit | edit source]General Principles
[edit | edit source]The 5As are an evidence-based framework for structuring smoking cessation in health care settings. The 5As include: Ask, Assess, Advise, Assist and Arrange follow-up.
|
Pharmacological
[edit | edit source]First-line pharmacotherapy includes the multiple forms of nicotine replacement therapy (patch, nasal spray, losenge, gum, inhaler), sustained- release bupropion hydrochloride, and varenicline. Second line therapy includes clonidine and nortriptyline and have been found to be efficacious.[6]
The following is a description of the various treatment modalities available:[7]
- Sustained release bupropion hydrochloride:
- Nicotine gum:
- Dose: 1–24 cigarettes/day: 2mg gum (up to 24 pieces/day). ≥ 25 cigarettes/day: 4 mg gum (up to 24 pieces/day).
- Duration: Up to 12 weeks
- Adverse effects: Mouth soreness and dyspepsia
- Nicotine inhaler:
- Dose: 6–16 cartridges/day
- Duration: Up to 6 months
- Adverse effects: Local irritation of mouth and throat
- Nicotine lozenges:
- Nicotine nasal spray:
- Dose: 8–40 doses/day
- Duration: 3–6 months
- Adverse effects: Nasal irritation
- Varenicline:
- Dose: 0.5 mg/day for 3 days followed by 0.5 mg twice/day for 4 days. Then, 1 mg twice/day
- Duration: 3–6 months
- Adverse effects: Nausea, trouble sleeping, vivid/strange dreams and depressed mood
References
[edit | edit source]- ↑ "CDC - Fact Sheet - Current Cigarette Smoking Among Adults in the United States - Smoking & Tobacco Use".
- ↑ "Map of Cigarette Use Among Adults | STATE System | CDC".
- ↑ "CDC - 2010 Surgeon General's Report - Consumer Booklet - Smoking & Tobacco Use".
- ↑ "QuickStats: Number of Deaths from 10 Leading Causes — National Vital Statistics System, United States, 2010".
- ↑ "CDC - 2014 Surgeon General's Report - Smoking & Tobacco Use".
- ↑ "www.vapremier.com" (PDF).
- ↑ Clinical Practice Guideline Treating Tobacco Use and Dependence 2008 Update Panel, Liaisons, and Staff (2008). "A clinical practice guideline for treating tobacco use and dependence: 2008 update. A U.S. Public Health Service report". Am J Prev Med. 35 (2): 158–76. doi:10.1016/j.amepre.2008.04.009. PMC 4465757. PMID 18617085.
 KSF
KSF