Tooth
 From Wikidoc - Reading time: 23 min
From Wikidoc - Reading time: 23 min
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
[edit | edit source]|
WikiDoc Resources for Tooth |
|
Articles |
|---|
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Tooth at Clinical Trials.gov Clinical Trials on Tooth at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Tooth
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Directions to Hospitals Treating Tooth Risk calculators and risk factors for Tooth
|
|
Healthcare Provider Resources |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Teeth (singular, tooth) are structures found in the jaws of many vertebrates that are used to tear, scrape, and chew food. Some animals, particularly carnivores, also use teeth for hunting or defense. The roots of teeth are covered by gums.
Teeth are among the most distinctive (and long-lasting) features of mammal species. Paleontologists use teeth to identify fossil species and determine their relationships. The shape of an animal's teeth is related to its diet. For example, plant matter is hard to digest, so herbivores have many molars for chewing. Carnivores, on the other hand, need canines to kill and tear meat.
Humans are diphyodont, meaning that they develop two sets of teeth. The first set (the "baby," "milk," "primary" or "deciduous" set) normally starts to appear at about six months of age, although some babies are born with one or more visible teeth, known as neonatal teeth. Normal tooth eruption at about six months is known as teething and can be quite painful for an infant.
Some animals develop only one set of teeth (monophyodont) while others develop many sets (polyphyodont). Sharks, for example, grow a new set of teeth every two weeks to replace worn teeth. Rodent incisors grow and wear away continually through gnawing, maintaining relatively constant length. Some rodent species, such as the sibling vole and the guinea pig, have continuously growing molars in addition to incisors.[1][2]
Anatomy
[edit | edit source]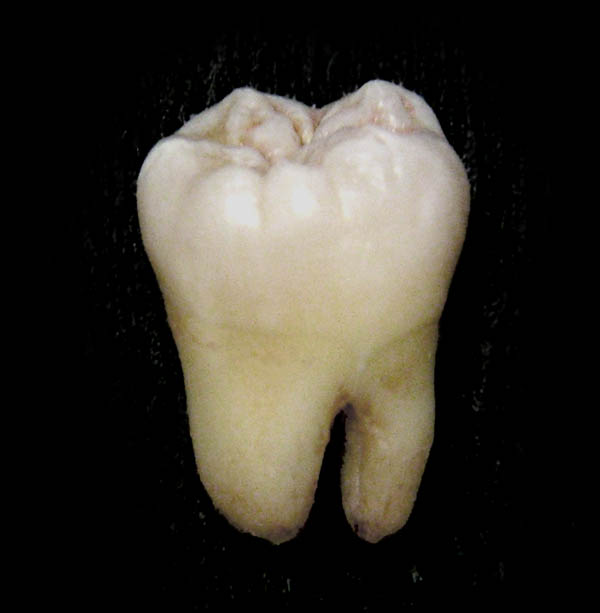
Dental anatomy is a field of anatomy dedicated to the study of tooth structures. The development, appearance, and classification of teeth fall within its purview, though dental occlusion, or contact among teeth, does not. Dental anatomy is also a taxonomical science as it is concerned with the naming of teeth and their structures. This information serves a practical purpose for dentists, enabling them to easily identify teeth and structures during treatment.
The anatomic crown of a tooth is the area covered in enamel above the cementoenamel junction (CEJ).[3] The majority of the crown is composed of dentin with the pulp chamber in the center.[4] The crown is within bone before eruption.[5] After eruption, it is almost always visible. The anatomic root is found below the cementoenamel junction and is covered with cementum. As with the crown, dentin composes most of the root, which normally have pulp canals. A tooth may have multiple roots or just one root. Canines and most premolars, except for maxillary (upper) first premolars, usually have one root. Maxillary first premolars and mandibular molars usually have two roots. Maxillary molars usually have three roots. Additional roots are referred to as supernumerary roots.
Humans usually have 20 primary teeth (also called deciduous, baby, or milk teeth) and 32 permanent teeth. Among primary teeth, 10 are found in the maxilla and the other 10 in the mandible. Teeth are classified as incisors, canines, and molars. In the primary set of teeth, there are two types of incisors, centrals and laterals, and two types of molars, first and second. All primary teeth are replaced with permanent counterparts except for molars, which are replaced by permanent premolars. Among permanent teeth, 16 are found in the maxilla with the other 16 in the mandible. The maxillary teeth are the maxillary central incisor, maxillary lateral incisor, maxillary canine, maxillary first premolar, maxillary second premolar, maxillary first molar, maxillary second molar, and maxillary third molar. The mandibular teeth are the mandibular central incisor, mandibular lateral incisor, mandibular canine, mandibular first premolar, mandibular second premolar, mandibular first molar, mandibular second molar, and mandibular third molar. Third molars are commonly called "wisdom teeth" and may never erupt into the mouth or form at all. If any additional teeth form, for example, fourth and fifth molars, which are rare, they are referred to as supernumerary teeth.[6]
Most teeth have identifiable features that distinguish them from others. There are several different notation systems to refer to a specific tooth. The three most commons systems are the FDI World Dental Federation notation, the universal numbering system, and Palmer notation method. The FDI system is used worldwide, and the universal is used widely in the United States.
Parts
[edit | edit source]Enamel
[edit | edit source]Enamel is the hardest and most highly mineralized substance of the body and is one of the four major tissues which make up the tooth, along with dentin, cementum, and dental pulp.[7] It is normally visible and must be supported by underlying dentin. Ninety-six percent of enamel consists of mineral, with water and organic material composing the rest.[8] The normal color of enamel varies from light yellow to grayish white. At the edges of teeth where there is no dentin underlying the enamel, the color sometimes has a slightly blue tone. Since enamel is semitranslucent, the color of dentin and any restorative dental material underneath the enamel strongly affects the appearance of a tooth. Enamel varies in thickness over the surface of the tooth and is often thickest at the cusp, up to 2.5 mm, and thinnest at its border, which is seen clinically as the cementoenamel junction (CEJ).[9]
Enamel's primary mineral is hydroxyapatite, which is a crystalline calcium phosphate.[10] The large amount of minerals in enamel accounts not only for its strength but also for its brittleness.[11] Dentin, which is less mineralized and less brittle, compensates for enamel and is necessary as a support.[10] Unlike dentin and bone, enamel does not contain collagen. Instead, it has two unique classes of proteins called amelogenins and enamelins. While the role of these proteins is not fully understood, it is believed that they aid in the development of enamel by serving as framework support among other functions.[12]
Dentin
[edit | edit source]Dentin is the substance between enamel or cementum and the pulp chamber. It is secreted by the odontoblasts of the dental pulp.[13] The formation of dentin is known as dentinogenesis. The porous, yellow-hued material is made up of 70% inorganic materials, 20% organic materials, and 10% water by weight.[14] Because it is softer than enamel, it decays more rapidly and is subject to severe cavities if not properly treated, but dentin still acts as a protective layer and supports the crown of the tooth.
Dentin is a mineralized connective tissue with an organic matrix of collagenous proteins. Dentin has microscopic channels, called dentinal tubules, which radiate outward through the dentin from the pulp cavity to the exterior cementum or enamel border.[15] The diameter of these tubules range from 2.5 μm near the pulp, to 1.2 μm in the midportion, and 900 nm near the dentino-enamel junction.[16] Although they may have tiny side-branches, the tubules do not intersect with each other. Their length is dictated by the radius of the tooth. The three dimensional configuration of the dentinal tubules is genetically determined.
Cementum
[edit | edit source]Cementum is a specialized bony substance covering the root of a tooth.[13] It is approximately 45% inorganic material (mainly hydroxyapatite), 33% organic material (mainly collagen) and 22% water. Cementum is excreted by cementoblasts within the root of the tooth and is thickest at the root apex. Its coloration is yellowish and it is softer than either dentin or enamel. The principle role of cementum is to serve as a medium by which the periodontal ligaments can attach to the tooth for stability. At the cementoenamel junction, the cementum is acellular due to its lack of cellular components, and this acellular type covers at least ⅔ of the root.[17] The more permeable form of cementum, cellular cementum, covers about ⅓ of the root apex.[18]
Pulp
[edit | edit source]The dental pulp is the central part of the tooth filled with soft connective tissue.[14] This tissue contains blood vessels and nerves that enter the tooth from a hole at the apex of the root.[19] Along the border between the dentin and the pulp are odontoblasts, which initiate the formation of dentin.[14] Other cells in the pulp include fibroblasts, preodontoblasts, macrophages and T lymphocytes.[20] The pulp is commonly called "the nerve" of the tooth.
Development
[edit | edit source]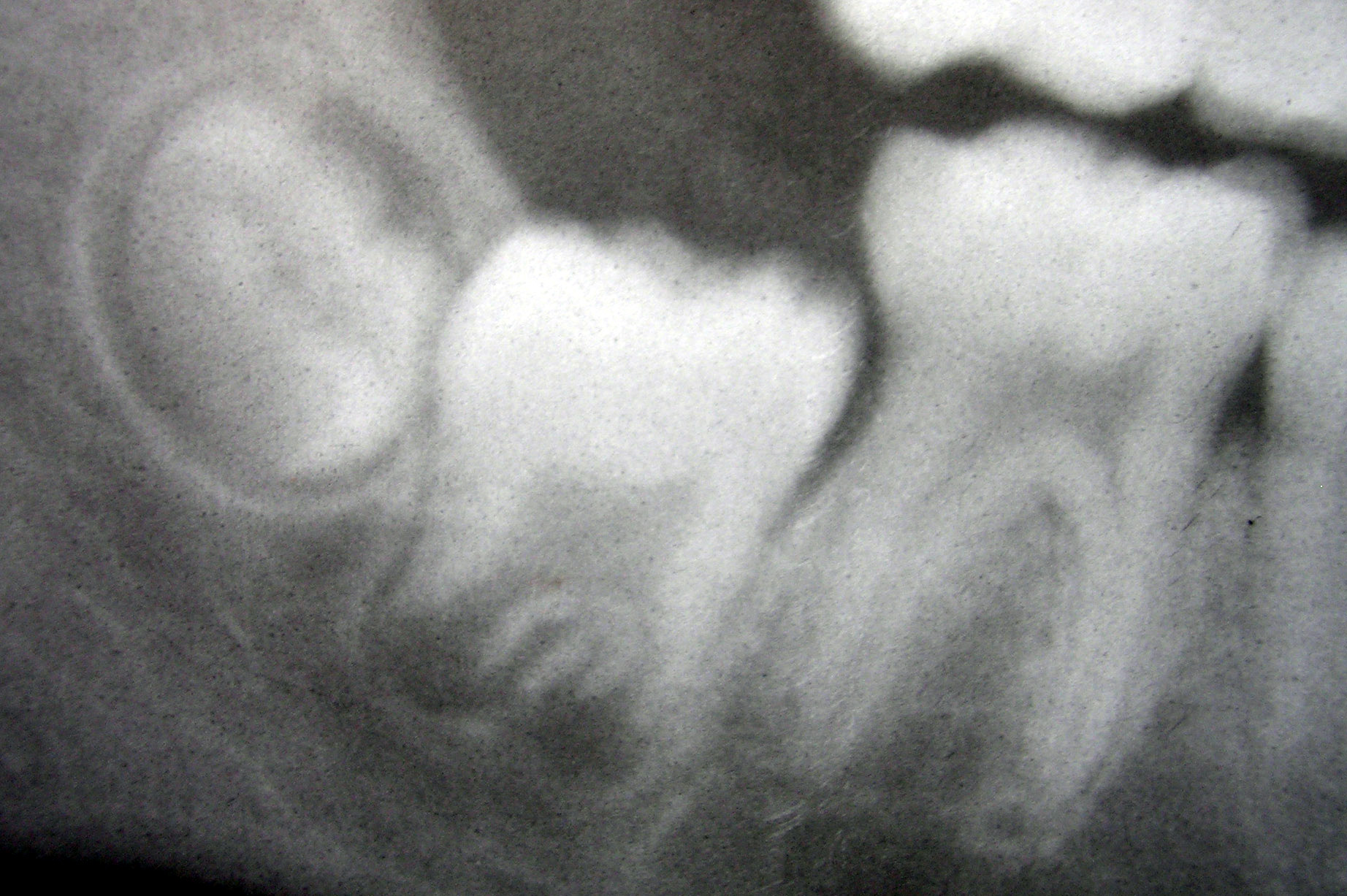
Tooth development is the complex process by which teeth form from embryonic cells, grow, and erupt into the mouth. Although many diverse species have teeth, non-human tooth development is largely the same as in humans. For human teeth to have a healthy oral environment, enamel, dentin, cementum, and the periodontium must all develop during appropriate stages of fetal development. Primary (baby) teeth start to form between the sixth and eighth weeks in utero, and permanent teeth begin to form in the twentieth week in utero.[21] If teeth do not start to develop at or near these times, they will not develop at all.
A significant amount of research has focused on determining the processes that initiate tooth development. It is widely accepted that there is a factor within the tissues of the first branchial arch that is necessary for the development of teeth.[22]
Tooth development is commonly divided into the following stages: the bud stage, the cap, the bell, and finally maturation. The staging of tooth development is an attempt to categorize changes that take place along a continuum; frequently it is difficult to decide what stage should be assigned to a particular developing tooth.[22] This determination is further complicated by the varying appearance of different histologic sections of the same developing tooth, which can appear to be different stages.
The tooth bud (sometimes called the tooth germ) is an aggregation of cells that eventually forms a tooth. It is organized into three parts: the enamel organ, the dental papilla and the dental follicle.[23] The enamel organ is composed of the outer enamel epithelium, inner enamel epithelium, stellate reticulum and stratum intermedium.[23] These cells give rise to ameloblasts, which produce enamel and the reduced enamel epithelium. The growth of cervical loop cells into the deeper tissues forms Hertwig's Epithelial Root Sheath, which determines a tooth's root shape. The dental papilla contains cells that develop into odontoblasts, which are dentin-forming cells.[23] Additionally, the junction between the dental papilla and inner enamel epithelium determines the crown shape of a tooth.[24] The dental follicle gives rise to three important entities: cementoblasts, osteoblasts, and fibroblasts. Cementoblasts form the cementum of a tooth. Osteoblasts give rise to the alveolar bone around the roots of teeth. Fibroblasts develop the periodontal ligaments which connect teeth to the alveolar bone through cementum.[25]
Eruption
[edit | edit source]Tooth eruption in humans is a process in tooth development in which the teeth enter the mouth and become visible. Current research indicates that the periodontal ligaments play an important role in tooth eruption. Primary teeth erupt into the mouth from around six months until two years of age. These teeth are the only ones in the mouth until a person is about six years old. At that time, the first permanent tooth erupts. This stage, during which a person has a combination of primary and permanent teeth, is known as the mixed stage. The mixed stage lasts until the last primary tooth is lost and the remaining permanent teeth erupt into the mouth.
There have been many theories about the cause of tooth eruption. One theory proposes that the developing root of a tooth pushes it into the mouth.[26] Another, known as the cushioned hammock theory, resulted from microscopic study of teeth, which was thought to show a ligament around the root. It was later discovered that the "ligament" was merely an artifact created in the process of preparing the slide.[27] Currently, the most widely held belief is that the periodontal ligaments provide the main impetus for the process.[28]
Supporting structures
[edit | edit source]
A: tooth
B: gingiva
C: bone
D: periodontal ligaments
The periodontium is the supporting structure of a tooth, helping to attach the tooth to surrounding tissues and to allow sensations of touch and pressure.[29] It consists of the cementum, periodontal ligaments, alveolar bone, and gingiva. Of these, cementum is the only one that is a part of a tooth. Periodontal ligaments connect the alveolar bone to the cementum. Alveolar bone surrounds the roots of teeth to provide support and creates what is commonly called an alveolus, or "socket". Lying over the bone is the gingiva, which is readily visible in the mouth.
Periodontal ligaments
[edit | edit source]The periodontal ligament is a specialized connective tissue that attaches the cementum of a tooth to the alveolar bone. This tissue covers the root of the tooth within the bone. Each ligament has a width of 0.15 - 0.38 mm, but this size decreases over time.[30] The functions of the periodontal ligaments include attachment of the tooth to the bone, support for the tooth, formation and resorption of bone during tooth movement, sensation, and eruption.[31] The cells of the periodontal ligaments include osteoblasts, osteoclasts, fibroblasts, macrophages, cementoblasts, and epithelial cell rests of Malassez.[32] Consisting of mostly Type I and III collagen, the fibers are grouped in bundles and named according to their location. The groups of fibers are named alveolar crest, horizontal, oblique, periapical, and interradicular fibers.[33] The nerve supply generally enters from the bone apical to the tooth and forms a network around the tooth toward the crest of the gingiva.[34] When pressure is exerted on a tooth, such as during chewing or biting, the tooth moves slightly in its socket and stretches the periodontal ligaments. The nerve fibers can then send the information to the central nervous system for interpretation.
Alveolar bone
[edit | edit source]The alveolar bone is the bone of the jaw which forms the alveolus around teeth.[35] Like any other bone in the human body, alveolar bone is modified throughout life. Osteoblasts create bone and osteoclasts destroy it, especially if force is placed on a tooth.[29] As is the case when movement of teeth is attempted through orthodontics, an area of bone under compressive force from a tooth moving toward it has a high osteoclast level, resulting in bone resorption. An area of bone receiving tension from periodontal ligaments attached to a tooth moving away from it has a high number of osteoblasts, resulting in bone formation.
Gingiva
[edit | edit source]The gingiva ("gums") is the mucosal tissue that overlays the jaws. There are three different types of epithelium associated with the gingiva: gingival, junctional, and sulcular epithelium. These three types form from a mass of epithelial cells known as the epithelial cuff between the tooth and the mouth.[36] The gingival epithelium is not associated directly with tooth attachment and is visible in the mouth. The junctional epithelium, composed of the basal lamina and hemidesmosomes, forms an attachment to the tooth.[31] The sulcular epithelium is nonkeratinized stratified squamous tissue on the gingiva which touches but is not attached to the tooth.[37] This leaves a small potential space between the gingiva and tooth which can collect bacteria, plaque, and calculus.
Tooth decay
[edit | edit source]Plaque
[edit | edit source]Plaque is a biofilm consisting of large quantities of various bacteria that form on teeth.[38] If not removed regularly, plaque buildup can lead to dental cavities (caries) or periodontal problems such as gingivitis. Given time, plaque can mineralize along the gingiva, forming tartar. The microorganisms that form the biofilm are almost entirely bacteria (mainly streptococcus and anaerobes), with the composition varying by location in the mouth.[39] Streptococcus mutans is the most important bacteria associated with dental caries.
Certain bacteria in the mouth live off the remains of foods, especially sugars and starches. In the absence of oxygen they produce lactic acid, which dissolves the calcium and phosphorus in the enamel.[13] [40] This process, known as "demineralisation", leads to tooth destruction. Saliva gradually neutralises the acids which cause the pH of the tooth surface to rise above the critical pH. This causes 'remineralisation', the return of the dissolved minerals to the enamel. If there is sufficient time between the intake of foods then the impact is limited and the teeth can repair themselves. Saliva is unable to penetrate through plaque, however, to neutralize the acid produced by the bacteria.
Caries (Cavities)
[edit | edit source]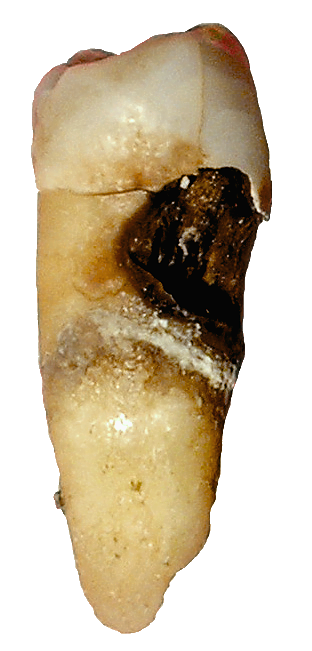
Dental caries, also described as "tooth decay" or "dental cavities", is an infectious disease which damages the structures of teeth.[41] The disease can lead to pain, tooth loss, infection, and, in severe cases, death. Dental caries has a long history, with evidence showing the disease was present in the Bronze, Iron, and Middle ages but also prior to the neolithic period.[42] The largest increases in the prevalence of caries have been associated with diet changes.[42][43] Today, caries remains one of the most common diseases throughout the world. In the United States, dental caries is the most common chronic childhood disease, being at least five times more common than asthma.[44] Countries that have experienced an overall decrease in cases of tooth decay continue to have a disparity in the distribution of the disease.[45] Among children in the United States and Europe, 60-80% of cases of dental caries occur in 20% of the population.[46]
Tooth decay is caused by certain types of acid-producing bacteria which cause the most damage in the presence of fermentable carbohydrates such as sucrose, fructose, and glucose.[47][48] The resulting acidic levels in the mouth affect teeth because a tooth's special mineral content causes it to be sensitive to low pH. Depending on the extent of tooth destruction, various treatments can be used to restore teeth to proper form, function, and aesthetics, but there is no known method to regenerate large amounts of tooth structure. Instead, dental health organizations advocate preventative and prophylactic measures, such as regular oral hygiene and dietary modifications, to avoid dental caries.[49]
Tooth care
[edit | edit source]
Oral hygiene is the practice of keeping the mouth clean and is a means of preventing dental caries, gingivitis, periodontal disease, bad breath, and other dental disorders. It consists of both professional and personal care. Regular cleanings, usually done by dentists and dental hygienists, remove tartar (mineralized plaque) that may develop even with careful brushing and flossing. Professional cleaning includes tooth scaling, using various instruments or devices to loosen and remove deposits from teeth.
The purpose of cleaning teeth is to remove plaque, which consists mostly of bacteria.[50] Healthcare professionals recommend regular brushing twice a day (in the morning and in the evening, or after meals) in order to prevent formation of plaque and tartar.[49] A toothbrush is able to remove most plaque, excepting areas between teeth. As a result, flossing is also considered a necessity to maintain oral hygiene. When used correctly, dental floss removes plaque from between teeth and at the gum line, where periodontal disease often begins and could develop caries. Electric toothbrushes are not considered more effective than manual brushes for most people.[51] The most important advantage of electric toothbrushes is their ability to aid people with dexterity difficulties, such as those associated with rheumatoid arthritis.
In addition, fluoride therapy is often recommended to protect against dental caries. Water fluoridation and fluoride supplements decrease the incidence of dental caries. Fluoride helps prevent dental decay by binding to the hydroxyapatite crystals in enamel.[52] The incorporated fluoride makes enamel more resistant to demineralization and thus more resistant to decay.[53] Topical fluoride, such as a fluoride toothpaste or mouthwash, is also recommended to protect teeth surfaces. Many dentists include application of topical fluoride solutions as part of routine cleanings.
Restorations
[edit | edit source]After a tooth has been damaged or destroyed, restoration of the missing structure can be achieved with a variety of treatments. Restorations may be created from a variety of materials, including amalgam, gold, porcelain, and composite.[54] Small restorations placed inside a tooth are referred to as "intracoronal restorations". These restorations may be formed directly in the mouth or may be cast using the lost-wax technique, such as for some inlays and onlays. When larger portions of a tooth are lost, an "extracoronal restoration" may be fabricated, such as a crown or a veneer, to restore the involved tooth.
When a tooth is lost, dentures, bridges, or implants may be used as replacements.[55] Dentures are usually the least costly whereas implants are usually the most expensive. Dentures may replace complete arches of the mouth or only a partial number of teeth. Bridges replace smaller spaces of missing teeth and use adjacent teeth to support the restoration. Dental implants may be used to replace a single tooth or a series of teeth. Though implants are the most expensive treatment option, they are often the most desirable restoration because of their esthetics and function. To improve the function of dentures, implants may be used as support.[56]
Abnormalities
[edit | edit source]Tooth abnormalities may be categorized according to whether they have environmental or developmental causes.[57] While environmental abnormalities may appear to have an obvious cause, there may not appear to be any known cause for some developmental abnormalities. Environmental forces may affect teeth during development, destroy tooth structure after development, discolor teeth at any stage of development, or alter the course of tooth eruption. Developmental abnormalities most commonly affect the number, size, shape, and structure of teeth.
Environmental
[edit | edit source]Alteration during tooth development
[edit | edit source]Tooth abnormalities caused by environmental factors during tooth development have long-lasting effects. Enamel and dentin do not regenerate after they mineralize initially. Enamel hypoplasia is a condition in which the amount of enamel formed is inadequate.[58] This results either in pits and grooves in areas of the tooth or in widespread absence of enamel. Diffuse opacities of enamel does not affect the amount of enamel but changes its appearance. Affected enamel has a different translucency than the rest of the tooth. Demarcated opacities of enamel have sharp boundaries where the translucency decreases and manifest a white, cream, yellow, or brown color. All these may be caused by a systemic event, such as an exanthematous fever.[59] Turner's hypoplasia is a portion of missing or diminished enamel on a permanent tooth usually from a prior infection of a nearby primary tooth. Hypoplasia may also result from antineoplastic therapy. Dental fluorosis is condition which results from ingesting excessive amounts of fluoride and leads to teeth which are spotted, yellow, brown, black or sometimes pitted. Enamel hypoplasia resulting from syphilis is frequently referred to as Hutchinson's teeth, which is considered one part of Hutchinson's triad.[60]
Destruction after development
[edit | edit source]Tooth destruction from processes other than dental caries is considered a normal physiologic process but may become severe enough to become a pathologic condition. Attrition is the loss of tooth structure by mechanical forces from opposing teeth.[61] Attrition initially affects the enamel and, if unchecked, may proceed to the underlying dentin. Abrasion is the loss of tooth structure by mechanical forces from a foreign element.[62] If this force begins at the cementoenamel junction, then progression of tooth loss can be rapid since enamel is very thin in this region of the tooth. A common source of this type of tooth wear is excessive force when using a toothbrush. Erosion is the loss of tooth structure due to chemical dissolution by acids not of bacterial origin.[63][64] Signs of tooth destruction from erosion is a common characteristic in the mouths of people with bulimia since vomiting results in exposure of the teeth to gastric acids. Another important source of erosive acids are from frequent sucking of lemon juice. Abfraction is the loss of tooth structure from flexural forces. As teeth flex under pressure, the arrangement of teeth touching each other, known as occlusion, causes tension on one side of the tooth and compression on the other side of the tooth. This is believed to cause V-shaped depressions on the side under tension and C-shaped depressions on the side under compression. When tooth destruction occurs at the roots of teeth, the process is referred to as internal resorption, when caused by cells within the pulp, or external resorption, when caused by cells in the periodontal ligament.
Discoloration
[edit | edit source]Discoloration of teeth may result from bacteria stains, tobacco, tea, coffee, foods with an abundance of chlorophyll, restorative materials, and medications.[65] Stains from bacteria may cause colors varying from green to black to orange. Green stains also result from foods with chlorophyll or excessive exposure to copper or nickel. Amalgam, a common dental restorative material, may turn adjacent areas of teeth black or gray. Chlorhexidine, a mouthwash, is associated with causing yellow-brown stains near the gingiva on teeth. Systemic disorders also can cause tooth discoloration. Congenital erythropoietic porphyria causes porphyrins to be deposited in teeth, causing a red-brown coloration. Blue discoloration may occur with alkaptonuria and rarely with Parkinson's disease. Erythroblastosis fetalis and biliary atresia are diseases which may cause teeth to appear green from the deposition of biliverdin. Also, trauma may change a tooth to a pink, yellow, or dark gray color. Pink and red discolorations are also associated in patients with lepromatous leprosy. Some medications, such as tetracycline antibiotics, may become incorporated into the structure of a tooth, causing intrinsic staining of the teeth.
Alteration of eruption
[edit | edit source]Tooth eruption may be altered by some environmental factors. When eruption is prematurely stopped, the tooth is said to be impacted. The most common cause of tooth impaction is lack of space in the mouth for the tooth.[66] Other causes may be tumors, cysts, trauma, and thickened bone or soft tissue. Ankylosis of a tooth occurs when the tooth has already erupted into the mouth but the cementum or dentin has fused with the alveolar bone. This may cause a person to retain their primary tooth instead of having it replaced by a permanent one.
A technique for altering the natural progression of eruption is employed by orthodontists who wish to delay or speed up the eruption of certain teeth for reasons of space maintenance or otherwise preventing crowding and/or spacing. If a primary tooth is extracted prior to the root of its succeeding permanent tooth reaching ⅓ of its total growth, the eruption of the permanent tooth will be delayed. Conversely, if the roots of the permanent tooth are more than ⅔ complete, the eruption of the permanent tooth will be accelerated. Between ⅓ and ⅔, it is unknown exactly what will occur to the speed of eruption.
Developmental
[edit | edit source]Abnormality in number
[edit | edit source]Anodontia is the total lack of tooth development. Hyperdontia is the presence of a higher-than-normal number of teeth, where as Hypodontia is the lack of some teeth. Usually, hypodontia refers to the lack of development of one or more teeth, and oligodontia may be used to describe the absence of 6 or more teeth. Some systemic disorders which may result in hyperdontia include Apert syndrome, Cleidocranial dysostosis, Crouzon syndrome, Ehlers-Danlos syndrome, Gardner syndrome, and Sturge-Weber syndrome.[67] Some systemic disorders which may result in hypodontia include Crouzon syndrome, Ectodermal dysplasia, Ehlers-Danlos syndrome, and Gorlin syndrome.[68]
Abnormality in size
[edit | edit source]Microdontia is a condition where teeth are smaller than the usual size, and macrodontia is where teeth are larger than the usual size. Microdontia of a single tooth is more likely to occur in a maxillary lateral incisor. The second most likely tooth to have microdontia are third molars. Macrodontia of all the teeth is known to occur in pituitary gigantism and pineal hyperplasia. It may also occur on one side of the face in cases of hemifacial hyperplasia.
Abnormality in shape
[edit | edit source]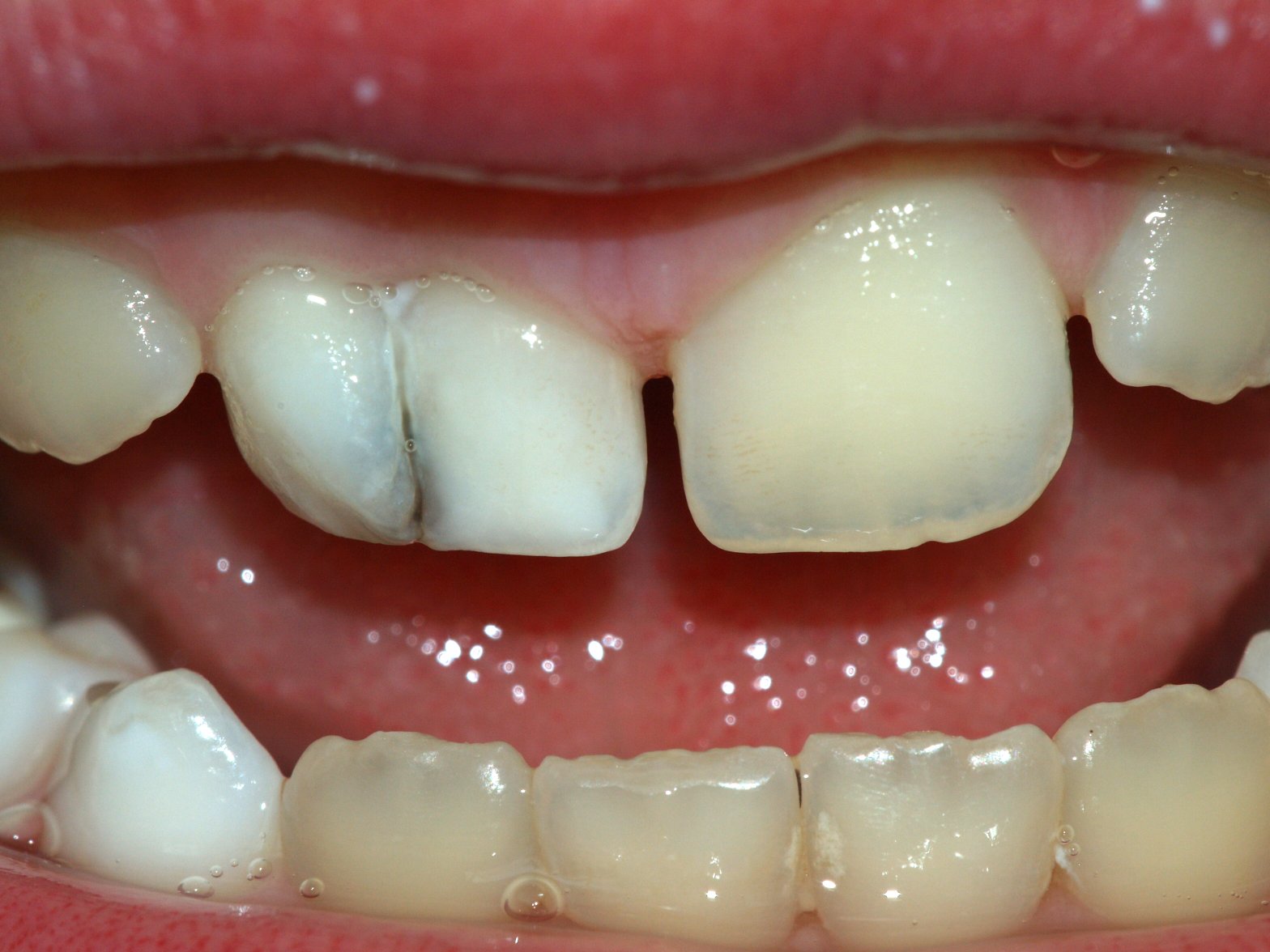
Gemination occurs when a developing tooth incompletely splits into the formation of two teeth. Fusion is the union of two adjacent teeth during development. Concrescence is the fusion of two separate teeth only in their cementum. Accessory cusps are additional cusps on a tooth and may manifest as a Talon cusp, Cusp of Carabelli, or Dens evaginatus. Dens invaginatus, also called Dens in dente, is a deep invagination in a tooth causing the appearance of a tooth within a tooth. Ectopic enamel is enamel found in an unusual location, such as the root of a tooth. Taurodontism is a condition where the body of the tooth and pulp chamber is enlarged, and is associated with Klinefelter syndrome, Tricho-dento-osseous syndrome, Triple X syndrome, and XYY syndrome.[69] Hypercementosis is excessive formation of cementum, which may result from trauma, inflammation, acromegaly, rheumatic fever, and Paget's disease of bone.[69] A dilaceration is a bend in the root which may have been caused by trauma to the tooth during formation. Supernumerary roots is the presence of a greater number of roots on a tooth than expected.
Abnormality in structure
[edit | edit source]Amelogenesis imperfecta is a condition in which enamel does not form properly or at all.[70] Dentinogenesis imperfecta is a condition in which dentin does not form properly and is sometimes associated with osteogenesis imperfecta.[71] Dentin dysplasia is a disorder in which the roots and pulp of teeth may be affected. Regional odontodysplasia is a disorder affecting enamel, dentin, and pulp and causes the teeth to appear "ghostly" on radiographs.[72]
In animals
[edit | edit source]Teeth vary greatly among animals. Some animals, such as turtles and tortoises, are toothless. Others, such as sharks, may go through many teeth in their lifetime. Walrus tusks are canine teeth that grow continuously throughout life.[73] Dog teeth are less likely than human teeth to form dental caries because of the very high pH of dog saliva, which prevents enamel from demineralizing.[74] Unlike humans whose ameloblasts die after tooth development, rodents continually produce enamel and must wear down their teeth by gnawing on various materials.[75] Horse teeth include twelve premolars, twelve molars, and twelve incisors. The structure of horse teeth is different from human teeth as the enamel and dentin layers are intertwined.[76]
References
[edit | edit source]- ↑ Tummers M and Thesleff I. Root or crown: a developmental choice orchestrated by the differential regulation of the epithelial stem cell niche in the tooth of two rodent species. Development (2003). 130(6):1049-57.
- ↑ AM Hunt. A description of the molar teeth and investing tissues of normal guinea pigs. J Dent Res. (1959) 38(2):216-31.
- ↑ Ash, Major M. and Stanley J. Nelson, 2003. Wheeler’s Dental Anatomy, Physiology, and Occlusion. 8th edition. Page 6. ISBN 0-7216-9382-2.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 3. ISBN 0-8151-2952-1.
- ↑ Ash, Major M. and Stanley J. Nelson, 2003. Wheeler’s Dental Anatomy, Physiology, and Occlusion. 8th edition. Page 9. ISBN 0-7216-9382-2.
- ↑ Kokten G, Balcioglu H, Buyukertan M. Supernumerary Fourth and Fifth Molars: A Report of Two Cases. Journal of Contemporary Dental Practice, 2003 November; (4)4:067-076. Page accessed February 10, 2007.
- ↑ Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina, "Histology: a Text and Atlas", 4th ed. (Baltimore: Lippincott Williams & Wilkins, 2002), p. 441.
- ↑ Cate, A. R. Ten, "Oral Histology: Development, Structure, and Function", 5th ed. (Saint Louis: Mosby-Year Book, 1998), p. 1.
- ↑ Cate, A. R. Ten, "Oral Histology: Development, Structure, and Function", 5th ed. (Saint Louis: Mosby-Year Book, 1998), p. 219.
- ↑ 10.0 10.1 Johnson, Clarke. "Biology of the Human Dentition," 1998. Page accessed on January 24, 2007.
- ↑ Cate, A. R. Ten, "Oral Histology: Development, Structure, and Function", 5th ed. (Saint Louis: Mosby-Year Book, 1998), p. 219.
- ↑ Cate, A. R. Ten, "Oral Histology: Development, Structure, and Function", 5th ed. (Saint Louis: Mosby-Year Book, 1998), p. 198.
- ↑ 13.0 13.1 13.2 Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina, 2003. Histology: a text and atlas. 4th edition. Page 448. ISBN 0-683-30242-6.
- ↑ 14.0 14.1 14.2 Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 150. ISBN 0-8151-2952-1.
- ↑ Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina, 2003. Histology: a text and atlas. 4th edition. Page 450. ISBN 0-683-30242-6.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 152. ISBN 0-8151-2952-1.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 236. ISBN 0-8151-2952-1.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 241. ISBN 0-8151-2952-1.
- ↑ Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina, 2003. Histology: a text and atlas. 4th edition. Page 451. ISBN 0-683-30242-6.
- ↑ Walton, Richard E. and Mahmoud Torabinejad. Principles and Practice of Endodontics. 3rd ed. 2002. Pages 11-13. ISBN 0-7216-9160-9.
- ↑ A. R. Ten Cate, Oral Histology: Development, Structure, and Function, 5th ed. (Saint Louis: Mosby-Year Book, 1998), p. 95. ISBN 0-8151-2952-1.
- ↑ 22.0 22.1 A. R. Ten Cate, Oral Histology: Development, Structure, and Function, 5th ed. (Saint Louis: Mosby-Year Book, 1998), p. 81. ISBN 0-8151-2952-1.
- ↑ 23.0 23.1 23.2 *University of Texas Medical Branch. "Lab Exercises: Tooth development." Page found here.
- ↑ A. R. Ten Cate, Oral Histology: Development, Structure, and Function, 5th ed. (Saint Louis: Mosby-Year Book, 1998), pp. 86 and 102. ISBN 0-8151-2952-1.
- ↑ *Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina. Histology: a text and atlas. 4th edition, p. 453. 2003. ISBN 0-683-30242-6.
- ↑ Harris, Edward F. Craniofacial Growth and Development. In the section entitled "Tooth Eruption." 2002. pp. 1-3.
- ↑ Harris, Edward F. Craniofacial Growth and Development. In the section entitled "Tooth Eruption." 2002. p. 3.
- ↑ Harris, Edward F. Craniofacial Growth and Development. In the section entitled "Tooth Eruption." 2002. p. 5.
- ↑ 29.0 29.1 Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina, 2003. Histology: a text and atlas. 4th edition. Page 452. ISBN 0-683-30242-6.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 256. ISBN 0-8151-2952-1.
- ↑ 31.0 31.1 Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina, 2003. Histology: a text and atlas. 4th edition. Page 453. ISBN 0-683-30242-6.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 260. ISBN 0-8151-2952-1.
- ↑ Listgarten, Max A. "Histology of the Periodontium: Principal fibers of the periodontal ligament," hosted on the University of Pennsylvania and Temple University website. Created May 8, 1999, revised 01/16/2007. Page accessed April 2, 2007.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 270. ISBN 0-8151-2952-1.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 274. ISBN 0-8151-2952-1.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Pages 247 and 248. ISBN 0-8151-2952-1.
- ↑ Cate, A.R. Ten. Oral Histology: development, structure, and function. 5th ed. 1998. Page 280. ISBN 0-8151-2952-1.
- ↑ "Oral Health Topics: Plaque", hosted on the American Dental Association website. Page accessed April 2, 2007.
- ↑ Introduction to dental plaque, hosted on the http://www.dentistry.leeds.ac.uk Leeds Dental Institute] website. Page accessed April 2, 2007.
- ↑ Ophardt, Charles E. "Sugar and tooth decay", hosted on the Elmhurst College website. Page accessed April 2, 2007.
- ↑ Dental Cavities, MedlinePlus Medical Encyclopedia, page accessed August 14, 2006.
- ↑ 42.0 42.1 Epidemiology of Dental Disease, hosted on the University of Illinois at Chicago website. Page accessed January 9, 2007.
- ↑ Suddick, Richard P. and Norman O. Harris. "Historical Perspectives of Oral Biology: A Series". Critical Reviews in Oral Biology and Medicine, 1(2), pages 135-151, 1990.
- ↑ Healthy People: 2010. Html version hosted on Healthy People.gov website. Page accessed August 13, 2006.
- ↑ "Dental caries", from the Disease Control Priorities Project. Page accessed August 15, 2006.
- ↑ Touger-Decker, Riva and Cor van Loveren. Sugars and dental caries, The American Journal of Clinical Nutrition, 78, 2003, pages 881S–892S.
- ↑ Hardie, J.M. (1982). The microbiology of dental caries. Dental Update, 9, 199-208.
- ↑ Holloway, P.J. (1983). The role of sugar in the etiology of dental caries. Journal of Dentistry, 11, 189-213.
- ↑ 49.0 49.1 Oral Health Topics: Cleaning your teeth and gums. Hosted on the American Dental Association website. Page accessed August 15, 2006.
- ↑ Introduction to Dental Plaque. Hosted on the Leeds Dental Institute Website, page accessed August 14, 2006.
- ↑ Thumbs down for electric toothbrush, hosted on the BBC News website, posted January 21, 2003. Page accessed January 23, 2007.
- ↑ Cate, A.R. Ten. "Oral Histology: development, structure, and function." 5th edition, 1998, p. 223. ISBN 0-8151-2952-1.
- ↑ Ross, Michael H., Gordon I. Kaye, and Wojciech Pawlina, 2003. "Histology: a text and atlas." 4th edition, p. 453. ISBN 0-683-30242-6.
- ↑ "Oral Health Topics: Dental Filling Options", hosted on the ADA website, page accessed May 8, 2007.
- ↑ "Prosthodontic Procedures", hosted on the The American College of Prosthodontists website. Page accessed May 16, 2007.
- ↑ "Dental Implants", hosted on the American Association of Oral and Maxillofacial Surgeons website. Page accessed May 16, 2007.
- ↑ Neville, B.W., D. Damm, C. Allen, J. Bouquot. Oral & Maxillofacial Pathology. Second edition. 2002. Page 50. ISBN 0-7216-9003-3.
- ↑ Ash, Major M. and Stanley J. Nelson, 2003. "Wheeler’s Dental Anatomy, Physiology, and Occlusion," 8th edition, p. 31.
- ↑ Neville, B.W., D. Damm, C. Allen, J. Bouquot. Oral & Maxillofacial Pathology. Second edition. 2002. Page 51. ISBN 0-7216-9003-3.
- ↑ Syphilis: Complications, hosted on the Mayo Clinic website. Page accessed January 21, 2007.
- ↑ "Loss of Tooth Structure", hosted on the American Dental Hygiene Association website. Page accessed April 25, 2007.
- ↑ "Abnormalities of Teeth", hosted on the University of Missouri-Kansas City School of Dentistry website. Page accessed April 25, 2007.
- ↑ Yip, Kevin H-K., Roger J. Smales, John A. Kaidonis. "The diagnosis and control of extrinsic acid erosion of tooth substance", hosted on the Academy of General Dentistry website. Page accessed April 25, 2007.
- ↑ Gandara B.K., Truelove E.L. "Diagnosis and Management of Dental Erosion", online version hosted on the The Journal of Contemporary Dental Practice website. Journal of Contemporary Dental Practice, 1999 October; (1)1, pages 16-23. Page accessed April 25, 2007.
- ↑ Neville, B.W., D. Damm, C. Allen, J. Bouquot. Oral & Maxillofacial Pathology. Second edition. 2002. Page 63. ISBN 0-7216-9003-3.
- ↑ Neville, B.W., D. Damm, C. Allen, J. Bouquot. Oral & Maxillofacial Pathology. Second edition. 2002. Page 66. ISBN 0-7216-9003-3.
- ↑ Neville, B.W., D. Damm, C. Allen, J. Bouquot. Oral & Maxillofacial Pathology. Second edition. 2002. Page 70. ISBN 0-7216-9003-3.
- ↑ Neville, B.W., D. Damm, C. Allen, J. Bouquot. Oral & Maxillofacial Pathology. Second edition. 2002. Page 69. ISBN 0-7216-9003-3.
- ↑ 69.0 69.1 Neville, B.W., D. Damm, C. Allen, J. Bouquot. Oral & Maxillofacial Pathology. Second edition. 2002. Page 85. ISBN 0-7216-9003-3.
- ↑ Amelogenesis imperfecta, hosted on the Genetics Home Reference website, a service of the U.S. National Library of Medicine. Page accessed April 1, 2007.
- ↑ Dentinogenesis imperfecta, hosted on the Genetics Home Reference website, a service of the U.S. National Library of Medicine. Page accessed April 1, 2007.
- ↑ Cho, Shiu-yin, Conservative Management of Regional Odontodysplasia: Case Report, hosted on the Canadian Dental Association website. Issue 72(8): pp. 735–8. Page accessed April 1, 2007.
- ↑ The Permanent Canine Teeth, hosted on the University of Illinois at Chicago website. Page accessed February 5, 2007.
- ↑ Chris C. Pinney, The Illustrated Veterinary Guide for Dogs, Cats, Birds, and Exotic Pets (Blue Ridge Summit, PA: TAB Books, 1992), p. 187.
- ↑ Caceci, Thomas. Veterinary Histology with subtitle "Digestive System: Oral Cavity" found here.
- ↑ Encarta article found here and Randall-Bowman, whose link can be found here
Template:Human anatomical features
Template:Head and neck general
Template:Tooth abnormalities
Template:Link FA
 KSF
KSF