Mpox
 From Wikipedia - Reading time: 31 min
From Wikipedia - Reading time: 31 min
| Mpox | |
|---|---|
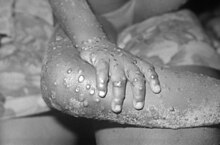 | |
| Mpox rash on arm and leg of a four-year-old girl in 1971 | |
| Pronunciation | |
| Specialty | Infectious disease[1] |
| Symptoms | Rash, fever, exhaustion, swollen lymph nodes, muscle aches, sore throat[2] |
| Complications | Secondary infections, pneumonia, sepsis, encephalitis, and loss of vision with severe eye infection[1] |
| Usual onset | 3–17 days post exposure[2] |
| Duration | 2 to 4 weeks[citation needed] |
| Types | Clade I, Clade II; subclades Ia, Ib, IIa, IIb[3] |
| Causes | Monkeypox virus |
| Diagnostic method | Testing for viral DNA[1] |
| Differential diagnosis | Chickenpox, smallpox[4] |
| Prevention | Smallpox & mpox vaccine, hand washing, covering rash, PPE, social distancing[1] |
| Treatment | Supportive[1] |
| Medication | Tecovirimat, antivirals[1] |
| Prognosis | Most recover[5] |
Mpox (/ˈɛmpɒks/, EM-poks; formerly known as monkeypox)[6] is an infectious viral disease that can occur in humans and other animals. Symptoms include a rash that forms blisters and then crusts over, fever, and swollen lymph nodes. The illness is usually mild, and most infected individuals recover within a few weeks without treatment. The time from exposure to the onset of symptoms ranges from three to seventeen days, and symptoms typically last from two to four weeks. However, cases may be severe, especially in children, pregnant women, or people with suppressed immune systems.[7][8][9]
The disease is caused by the monkeypox virus, a zoonotic virus in the genus Orthopoxvirus. The variola virus, which causes smallpox, is also in this genus.[1] Human-to-human transmission can occur through direct contact with infected skin or body fluids, including sexual contact.[1] People remain infectious from the onset of symptoms until all the lesions have scabbed and healed.[7] The virus may spread from infected animals through handling infected meat or via bites or scratches.[7] Diagnosis can be confirmed by polymerase chain reaction (PCR) testing a lesion for the virus's DNA.[1]
Vaccination is recommended for those at high risk of infection.[1] No vaccine has been developed specifically against mpox, but smallpox vaccines have been found to be effective.[10] There is no specific treatment for the disease, so the aim of treatment is to manage the symptoms and prevent complications.[1][11] Antiviral drugs such as tecovirimat can be used to treat mpox,[1] although their effectiveness has not been proved.[12]
Mpox is endemic in Central and Western Africa, where several species of mammals are suspected to act as a natural reservoir of the virus.[1] The first human cases were diagnosed in 1970 in Basankusu, Democratic Republic of the Congo.[13] Since then, the frequency and severity of outbreaks have significantly increased, possibly as a result of waning immunity since the cessation of routine smallpox vaccination.[13] A global outbreak of clade II in 2022–2023 marked the first incidence of widespread community transmission outside of Africa. In July 2022, the World Health Organization (WHO) declared the outbreak a public health emergency of international concern (PHEIC). The WHO reverted this status in May 2023,[14] as the outbreak came under control, citing a combination of vaccination and public health information as successful control measures.[15]
An outbreak of new variant of clade I mpox (known as clade Ib) was detected in the Democratic Republic of the Congo during 2023.[16] As of August 2024, it had spread to several African countries, raising concerns that it may have adapted to more sustained human transmission.[17][18] In August 2024, the WHO declared the outbreak a public health emergency of international concern.[19][14]
Nomenclature
[edit]The name monkeypox was originally coined because the disease was first identified in laboratory monkeys.[20] This name was later criticized by scientists as a misnomer since monkeys are not the main host or reservoir; it was also criticized by the Foreign Press Association of Africa because the name reinforced racism and stigma about African countries and their residents being a source of disease. In November 2022, the WHO announced that it "will adopt the term mpox in its communications, and encourages others to follow these recommendations".[21][22]
The subtypes of monkeypox virus were renamed in August 2022 after requests by several public health organisations and scientists, who argued that the former geographical names were hindering efforts to contain the disease. The clade formerly known as "Congo Basin (Central African)" was renamed clade I, and the clade formerly known as "West African" was renamed clade II.[23][24]
Signs and symptoms
[edit]



Initial symptoms of mpox infection are fever, muscle pains, and sore throat, followed by an itchy or painful rash, headache, swollen lymph nodes, and fatigue. Not everyone will exhibit the complete range of symptoms.[1][2]
People with mpox usually become symptomatic about a week after infection. However the incubation period can vary in a range between one day and four weeks.[1][26]
The rash comprises numerous small lesions, which may appear on the palms, soles, face, mouth, throat, genitals, or anus.[1] They begin as small flat spots, before developing into small bumps, which then fill with fluid, eventually bursting and scabbing over, typically lasting around ten days.[2] In rare cases, lesions may become necrotic, requiring debridement and taking longer to heal.[27][25]
Some people may manifest only a single sore from the disease, while others may have hundreds.[1] An individual can be infected with Orthopoxvirus monkeypox without showing any symptoms.[1] Symptoms typically last for two to four weeks but may persist longer in people with weakened immune systems.[2][1]
Complications
[edit]Complications include secondary infections, pneumonia, sepsis, encephalitis, and loss of vision following corneal infection.[1] Persons with weakened immune systems, whether due to medication, medical conditions, or HIV, are more likely to develop severe cases of the disease.[1] If infection occurs during pregnancy, this may lead to stillbirth or other complications.[7]
Outcome
[edit]Provided there are no complications, sequelae are rare; after healing, the scabs may leave pale marks before becoming darker scars.[28]
Deaths
[edit]Historically, the case fatality rate (CFR) of past outbreaks was estimated at between 1% and 10%, with clade I considered to be more severe than clade II.[29][30]
The case fatality rate of the 2022–2023 global outbreak caused by clade IIb was very low, estimated at 0.16%, with the majority of deaths in individuals who were already immunocompromized.[31] In contrast, as of April 2024[update], the outbreak of clade I in Democratic Republic of the Congo has a CFR of 4.9%.[32]
The difference between these estimates is attributed to:
- differences in the virulence of clade I versus clade II.[32]
- under-reporting of mild or asymptomatic cases in the endemic areas of Africa, which generally have poor healthcare infrastructure.[29]
- evolution of the virus to cause milder disease in humans.[33]
- better general health, and better health care, in the populations most affected by the 2022–2023 global outbreak.[29]
In other animals
[edit]It is thought that small mammals provide a reservoir for the virus in endemic areas.[34] Spread among animals occurs via the fecal–oral route and through the nose, through wounds and eating infected meat.[35] The disease has also been reported in a wide range of other animals, including monkeys, anteaters, hedgehogs, prairie dogs, squirrels, and shrews. Signs and symptoms in animals are not well researched and further studies are in progress.[34]
There have been instances of animal infection outside of endemic Africa; during the 2003 US outbreak, prairie dogs (Cynomys ludovicianus) became infected and presented with fever, cough, sore eyes, poor feeding and rash.[36] There has also been an instance of a domestic dog (Canis familiaris) which became infected displaying lesions and ulceration.[37]
Cause
[edit]Mpox in both humans and animals is caused by infection with Orthopoxvirus monkeypox – a double-stranded DNA virus in the genus Orthopoxvirus, family Poxviridae, making it closely related to the smallpox, cowpox, and vaccinia viruses.[1]
The two major subtypes of virus are clade I and clade II. In April 2024, after detection of a new variant, clade I was split into subclades designated Ia and Ib. Clade II is similarly divided into subclades: clade IIa and clade IIb.[1][3][38]
Clade I is estimated to cause more severe disease and higher mortality than clade II.[11]

The virus is considered to be endemic in tropical rainforest regions of Central and West Africa.[39] In addition to monkeys, the virus has been identified in Gambian pouched rats (Cricetomys gambianus), dormice (Graphiurus spp.) and African squirrels (Heliosciurus, and Funisciurus). The use of these animals as food may be an important source of transmission to humans.[1]
Transmission
[edit]The natural reservoir of Orthopoxvirus monkeypox is thought to be small mammals in tropical Africa.[39] The virus can be transmitted from animal to human from bites or scratches, or during activities such as hunting, skinning, or cooking infected animals. The virus enters the body through broken skin, or mucosal surfaces such as the mouth, respiratory tract, or genitals.[1]
Mpox can be transmitted from one person to another through contact with infectious lesion material or fluid on the skin, in the mouth or on the genitals; this includes touching, close contact, and during sex. During the 2022–2023 global outbreak of clade II, transmission between people was almost exclusively via sexual contact.[1][40][41]
There is also a risk of infection from fomites (objects which can become infectious after being touched by an infected person) such as clothing or bedding which has been contaminated with lesion material.[40]
Diagnosis
[edit]Clinical differential diagnosis distinguishes between rash illnesses, such as chickenpox, measles, bacterial skin infections, scabies, poison ivy, syphilis, and medication-associated allergies.[medical citation needed]
Polymerase chain reaction (PCR) testing of samples from skin lesions is the preferred diagnostic test, although it has the disadvantage of being relatively slow to deliver a result.[1] In October 2024, the WHO approved the first diagnostic test under the Emergency Use Listing (EUL) procedure. The Alinity m MPXV assay enables the detection of the virus by laboratory testing swabs of skin lesions, giving a result in less than two hours.[42][43]
Prevention
[edit]Vaccine
[edit]Historically, smallpox vaccine had been reported to reduce the risk of mpox among previously vaccinated persons in Africa. The decrease in immunity to poxviruses in exposed populations is a factor in the increasing prevalence of human mpox. It is attributed to waning cross-protective immunity among those vaccinated before 1980, when mass smallpox vaccinations were discontinued, and to the gradually increasing proportion of unvaccinated individuals.[44]
As of August 2024, there are four vaccines in use to prevent mpox. All were originally developed to combat smallpox.[45]
- MVA-BN (marketed as Jynneos, Imvamune or Imvanex) manufactured by Bavarian Nordic. Licensed for use against mpox in Europe, United States and Canada.[46]
- LC16 from KMB Biologics (Japan) – licensed for use in Japan.[47]
- OrthopoxVac, licensed for use in Russia and manufactured by the State Research Center of Virology and Biotechnology VECTOR in Russia[48]
- ACAM2000, manufactured by Emergent BioSolutions. Approved for use against mpox in the United States as of August 2024.[49][50]
The MVA-BN vaccine, originally developed for smallpox, has been approved in the United States for use by persons who are either considered at high risk of exposure to mpox, or who may have recently been exposed to it.[51][52][53][54] The United States Centers for Disease Control and Prevention (CDC) recommends that persons investigating mpox outbreaks, those caring for infected individuals or animals, and those exposed by close or intimate contact with infected individuals or animals should receive a vaccination.[20]
Other measures
[edit]The CDC has made detailed recommendations in addition to the standard precautions for infection control. These include that healthcare providers don a gown, mask, goggles, and a disposable filtering respirator (such as an N95), and that an infected person should be isolated a private room to keep others from possible contact.[55]
Those living in countries where mpox is endemic should avoid contact with sick mammals such as rodents, marsupials, non-human primates (dead or alive) that could harbour Orthopoxvirus monkeypox and should refrain from eating or handling wild game (bush meat).[56][7]
During the 2022–2023 outbreak, several public health authorities launched public awareness campaigns in order to reduce spread of the disease.[57][58][59]
Treatment
[edit]Most cases of mpox present with mild symptoms and there is complete recovery within 2 to 4 weeks.[5][7] There is no specific treatment for the disease, although antivirals such as tecovirimat have been approved for the treatment of severe mpox.[12][60][11] A 2023 Cochrane review found no completed randomized controlled trials studying therapeutics for the treatment of mpox.[61] The review identified non-randomized controlled trials which evaluated the safety of therapeutics for mpox, finding no significant risks from tecovirimat and low certainty evidence that suggests brincidofovir may cause mild liver injury.[61] Pain is common and may be severe; supportive care such as pain or fever control may be administered.[7][62] People with mild disease should isolate at home, stay hydrated, eat well, and take steps to maintain their mental health.[1]
People who are at high risk from the disease include children, pregnant women, the elderly and those who are immunocompromized.[63] For these people, or those who have severe disease, hospital admission and careful monitoring of symptoms is recommended.[62] Symptomatic treatment is recommended for complications such as proctitis and pruritis.[62]
A trial in the Democratic Republic of the Congo found that the antiviral drug tecovirimat did not shorten the duration of mpox lesions in people with clade I mpox.[64] Despite this, the trial's overall mortality rate of 1.7% was notably lower than the 3.6% or higher mortality rate seen in the Democratic Republic of the Congo's general mpox cases.[65] This suggests that hospitalization and high-quality supportive care significantly improve outcomes for mpox people.[66] The trial was sponsored by the NIH and co-led by the Democratic Republic of the Congo's Institut National de Recherche Biomédicale.
An additional 2024 study on Siga Technologies’ antiviral drug, tecovirimat, found it ineffective in reducing lesion healing time or pain in adults with the clade II strain of mpox.[67] Based on interim results, a safety board recommended halting further patient enrollment. The trial, launched in September 2022 by the U.S. National Institute of Allergy and Infectious Diseases, involved patients from several countries, including the U.S., Argentina, and Japan, who had mpox symptoms for less than 14 days.[68] An interim analysis revealed no significant differences in lesion resolution or pain reduction between tecovirimat and a placebo.[69]
Diagnostics in resource limited settings
[edit]With the August 2024 outbreak in the DRC, the World Health Organization (WHO) urged manufacturers to submit their products for emergency review.[70] This initiative is part of the WHO's effort to ensure effective diagnostics, particularly for low-income populations. The agency has called for manufacturers to submit their tests for Emergency Use Listing, which would allow the WHO to approve these medical products more quickly.[71] This process is designed to help countries procure essential products through UN agencies and other partners. The urgency comes as a new, easily transmissible form of the 2024 outbreak has raised global concerns, leading the WHO to declare mpox a global public health emergency.[72]
Epidemiology
[edit]This section needs to be updated. The reason given is: More recent evidence is available. (May 2023) |

History
[edit]Mpox was first identified as a distinct illness in 1958 among laboratory monkeys in Copenhagen, Denmark.[73] The first documented human cases occurred in 1970, involving six unvaccinated children during the smallpox eradication efforts, with the first being a 9-month-old boy in the Democratic Republic of the Congo.[13][74] From 1981 to 1986, over 300 human cases of mpox were reported in the Democratic Republic of the Congo (then known as Zaire), primarily due to contact with animals.[75] The virus has been detected in Gambian pouched rats, dormice, and African squirrels, which are often used as food.[76][1]
Many more mpox cases have been reported in Central and West Africa, particularly in the Democratic Republic of the Congo, where 2,000 cases per year were recorded between 2011 and 2014. However, the collected data is often incomplete and unconfirmed, hindering accurate estimations of the number of mpox cases over time.[77] Originally thought to be uncommon in humans, cases have increased since the 1980s,[78][13] possibly as a result of waning immunity following the cessation of routine smallpox vaccination.[4]
Future threat
[edit]The natural reservoir of Orthopoxvirus monkeypox has not been conclusively determined. Small rodents are considered the most likely candidate. Without a major vaccination campaign, mpox outbreaks in humans will continue indefinitely in the endemic areas, with an ongoing risk that disease outbreaks will spread to non-endemic areas. Other evidence – that the virus is evolving to be more transmissible among humans, that it can infect a wide range of host species, and that human-to-animal transmission can occur – led to concerns that mpox may either become established in new natural reservoirs outside of Africa, or cause future global epidemics.[79][80][81][82]
Following the 2022–2023 outbreak, mpox (clade IIb) remains present in the human population outside Africa at very low levels.[83] In November 2023, the WHO reported increasing numbers of cases of mpox (clade I) in the Democratic Republic of the Congo, with 12,569 cases year-to-date and 651 fatalities; there was also the first evidence of sexual transmission of clade I.[84]
In 2024, the WHO added the monkeypox virus to its list of "priority pathogens" that could cause a pandemic.[85]
Outbreaks
[edit]This section is an incomplete list of disease outbreaks which have been reported, including significant outbreaks in the endemic countries in tropical Africa (Benin, Cameroon, the Central African Republic, the Democratic Republic of the Congo, Gabon, Ghana, Ivory Coast, Liberia, Nigeria, the Republic of the Congo, Sierra Leone, and South Sudan).[86] Outbreaks of mpox are frequent in areas where the disease is endemic – these areas often have poor healthcare infrastructure and outbreaks are rarely documented.[87][88][89]
| Year | Country | Clade | Human cases | Human deaths | Case fatality rate | Notes |
|---|---|---|---|---|---|---|
| 1970 | Clade I | 5 | no data | N/A | ||
| 1971 | Clade II | 2 | no data | N/A | ||
| 1981–1986 | Clade I | 338 | no data | N/A | ||
| 1995–1996 | Clade I | >500 | no data | N/A | ||
| 2001–2004 | Clade I | 2,734 | no data | N/A | ||
| 2003 | Clade II | 71 | 0 | 0% | ||
| 2015 | Clade I | 10 | 2 | 20% | ||
| 2017–2022 | Clade II | 558 | 8 | 1.4% | ||
| 2020 | Clade I | 4,600 | 171 | 3.7% | ||
| 2022–2023 | Global outbreak | Clade IIb | 93,327 | 208 | 0.2% | *ongoing[92] |
| 2023–2024* | Clade I Clade Ib |
>18,245 | >919 | ~5% | *ongoing[93] |
United States
[edit]In May 2003, a young child became ill with fever and rash after being bitten by a prairie dog purchased at a local swap meet near Milwaukee, Wisconsin.[94] In total, 71 cases of mpox were reported through 20 June 2003. All cases were traced to Gambian pouched rats imported from Accra, Ghana, in April 2003 by a Texas exotic animal distributor. No deaths resulted.[95] Electron microscopy and serologic studies were used to confirm that the disease was human mpox.[96] Everyone affected reported direct or close contact with prairie dogs, later found to be infected with the Orthopoxvirus monkeypox.[97]
In July 2021, in the US, an American returning from a trip in Nigeria was diagnosed with mpox. Subsequent testing identified the virus as belonging to clade II. The patient was hospitalized and treated with tecovirimat and was discharged after 32 days.[98]
The first case of clade I mpox in the United States was identified in November 2024; the California Department of Public Health reported that an unidentified individual outside San Francisco had tested positive following travel to and from East Africa.[99] Clade II mpox continues to circulate at low levels.[100][101]
Sudan
[edit]During 2022, an outbreak of clade I mpox was reported in refugee camps in Sudan.[1] The first case in the country was recorded in August, and in September, six additional cases were discovered in Khartoum.[102] In October, more than 100 cases were reported among Ethiopian refugee camps.[102]
Nigeria
[edit]Two cases of human mpox infections were identified in Nigeria in 1971. In September 2017, Orthopoxvirus monkeypox was reported in Nigeria. The subsequent outbreak was, at that time, the largest ever outbreak of clade II of the virus, with 118 confirmed cases. Unlike previous outbreaks of this clade, infection was predominantly among young male adults and human-to-human transmission appears to have readily occurred. Seven deaths (5 male, 2 female, case fatality rate of 6%) were reported, including a baby and four HIV/AIDS people. Additionally, a pregnant woman in her second trimester had a spontaneous miscarriage attributed to Orthopoxvirus monkeypox infection.[103]
In May 2022, the Nigerian government released a report stating that between 2017 and 2022, 558 cases were confirmed across 32 states and the Federal Capital Territory. There were 8 deaths reported, making for a 1.4% Case Fatality Ratio. In 2022, NCDC implemented a National Technical Working Group for reporting and monitoring infections, strengthening response capacity.[104]
United Kingdom
[edit]In September 2018, the United Kingdom's first case of mpox was recorded. The person, a Nigerian national, is believed to have contracted mpox in Nigeria before travelling to the United Kingdom.[105] A second case was confirmed in the town of Blackpool, with a further case that of a medical worker who cared for the infected person from Blackpool.[106]
In December 2019, mpox was diagnosed in a person in South West England who had traveled to the UK from Nigeria.[107]
In May 2021, two cases of mpox from a single household were identified by Public Health Wales in the UK. The index case had traveled from Nigeria. Covid guidance to isolate after travel helped detection of the outbreak and to prevent further transmission.[108]
Singapore
[edit]In May 2019, a 38-year-old man who traveled from Nigeria was hospitalized in an isolation ward at the National Centre for Infectious Diseases in Singapore, after being confirmed as the country's first case of mpox. As a result, 22 people were quarantined.[109] The case may have been linked to a simultaneous outbreak in Nigeria.[110]
2022–2023 global outbreak
[edit]An outbreak of mpox caused by clade IIb of the virus was first identified in May 2022.[111] The first case was detected in London, United Kingdom, on 6 May, in a patient with a recent travel history from Nigeria, where the disease is endemic.[112][113] Subsequent cases were reported in an increasing number of countries and regions.[120] In July 2022, the WHO declared the outbreak a public health emergency of international concern. This status was terminated in May 2023 due to steady progress in controlling the spread of the disease, attributed to a combination of vaccination and public health information.[121] As of August 2024[update], clade IIb mpox cases outside of endemic regions in Africa continued to be reported at a low level.[92]
2023–2024 Central Africa outbreak
[edit]During 2023, a clade I outbreak of mpox disease in the Democratic Republic of the Congo resulted in 14,626 suspected cases being reported, with 654 associated deaths, making for a case-fatality rate of 4.5%. The outbreak continued into 2024, with 3,576 suspected mpox cases and 265 deaths reported in the Democratic Republic of the Congo through the first nine weeks of the year, making for an estimated CFR of 7.4%.[122]
Transmission of the virus in the outbreak appears to be primarily through sexual and close familial contact, with cases occurring in areas without a history of mpox, such as South Kivu and Kinshasa. An estimated 64% of the cases and 85% of fatalities have occurred in children. The outbreak consists of two separate sub-variants of clade I, with one of the sub-variants having a novel mutation, making detection with standard assays unreliable.[122][123]
The outbreak spread to the neighbouring country of the Republic of the Congo, with 43 cases reported in March 2024.[122] By August 2024, the outbreak spread further into central and southern Africa with cases of clade I and clade II strains reported in Burundi, Rwanda, Uganda, Kenya, Côte d'Ivoire, and South Africa.[93][18]
The WHO declared a global health emergency in August 2024.[19][14][124] Sweden became the first non-African country to report a case of clade I mpox.[125] A case of mpox was confirmed in Pakistan.[126]
See also
[edit]- 1964 outbreak of mpox at Rotterdam Zoo, in the Netherlands (with no cases in humans)
- 2022–2023 mpox outbreak
- 2022–2023 mpox outbreak in Canada
- 2022–2023 mpox outbreak in the United States
- 2022–2023 mpox outbreak in the United Kingdom
Notes
[edit]References
[edit]- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac ad "WHO Factsheet – Mpox (Monkeypox)". World Health Organization (WHO). 18 April 2023. Archived from the original on 21 April 2022. Retrieved 21 May 2023.
- ^ a b c d e "Mpox Symptoms". U.S. Centers for Disease Control and Prevention (CDC). 15 March 2024. Archived from the original on 2 April 2024. Retrieved 22 August 2024.
- ^ a b "Mpox: background information". UK Health Security Agency. 19 August 2024. Retrieved 21 August 2024.
- ^ a b McCollum AM, Damon IK (January 2014). "Human monkeypox". Clinical Infectious Diseases. 58 (2): 260–267. doi:10.1093/cid/cit703. PMID 24158414.
- ^ a b "Mpox: background information". UK Health Security Agency. 19 August 2024. Archived from the original on 20 August 2024. Retrieved 22 August 2024.
- ^ "WHO recommends new name for monkeypox disease" (Press release). World Health Organization (WHO). 28 November 2022. Archived from the original on 1 December 2022. Retrieved 29 November 2022.
- ^ a b c d e f g "Mpox". World Health Organization (WHO). 17 August 2024. Archived from the original on 19 August 2024. Retrieved 22 August 2024.
- ^ "WHO Factsheet – Mpox (Monkeypox)". World Health Organization (WHO). 18 April 2023. Archived from the original on 21 April 2022. Retrieved 21 May 2023.
- ^ "Mpox Symptoms". U.S. Centers for Disease Control and Prevention (CDC). 15 March 2024. Archived from the original on 2 April 2024. Retrieved 22 August 2024.
- ^ Christodoulidou MM, Mabbott NA (1 January 2023). "Efficacy of smallpox vaccines against Mpox infections in humans". Immunotherapy Advances. 3 (1): ltad020. doi:10.1093/immadv/ltad020. PMC 10598838. PMID 37886620.
- ^ a b c "Mpox (formerly Monkeypox)". NIH: National Institute of Allergy and Infectious Diseases. 6 December 2022. Archived from the original on 23 May 2023. Retrieved 24 May 2023.
- ^ a b "Patient's Guide to Mpox Treatment with Tecovirimat (TPOXX)". U.S. Centers for Disease Control and Prevention (CDC). 28 November 2022. Archived from the original on 24 May 2023. Retrieved 24 May 2023.
- ^ a b c d Bunge EM, Hoet B, Chen L, Lienert F, Weidenthaler H, Baer LR, et al. (February 2022). "The changing epidemiology of human monkeypox-A potential threat? A systematic review". PLOS Neglected Tropical Diseases. 16 (2): e0010141. doi:10.1371/journal.pntd.0010141. PMC 8870502. PMID 35148313.
- ^ a b c "WHO Director-General declares mpox outbreak a public health emergency of international concern". World Health Organization (WHO) (Press release). 14 August 2024. Retrieved 19 October 2024.
- ^ "Mpox (monkeypox) Outbreak". World Health Organization (WHO). Archived from the original on 31 July 2022. Retrieved 13 May 2023.
- ^ "Clade I Mpox Outbreak Originating in Central Africa". U.S. Centers for Disease Control and Prevention (CDC). 10 October 2024. Retrieved 20 October 2024.
- ^ "How scientists are racing to understand the new Mpox strain in the Democratic Republic of the Congo". Gavi, the Vaccine Alliance. 30 July 2024. Retrieved 6 August 2024.
- ^ a b "WHO considers public health emergency as mpox cases mount in Africa". Center for Infectious Disease Research and Policy (CIDRAP). 5 August 2024. Archived from the original on 6 August 2024. Retrieved 6 August 2024.
- ^ a b "WHO declares mpox a public health emergency as newer strain spreads in Africa". MSN. 14 August 2024. Retrieved 14 August 2024.
- ^ a b "About Mpox". U.S. Centers for Disease Control and Prevention (CDC). Archived from the original on 11 March 2023. Retrieved 13 March 2023.
- ^ Taylor L (June 2022). "Monkeypox: WHO to rename disease to prevent stigma". BMJ. 377: o1489. doi:10.1136/bmj.o1489. PMID 35710105.
- ^ "WHO recommends new name for monkeypox disease" (Press release). World Health Organization (WHO). 28 November 2022. Archived from the original on 1 December 2022. Retrieved 29 November 2022.
- ^ "Urgent need for a non-discriminatory and non-stigmatizing nomenclature for monkeypox virus". Virological. 16 August 2022. Archived from the original on 25 May 2023. Retrieved 25 May 2023.
- ^ "Monkeypox: experts give virus variants new names". World Health Organization (WHO). Retrieved 16 August 2024.
- ^ a b Caldas JP, Valdoleiros SR, Rebelo S, Tavares M (December 2022). "Monkeypox after Occupational Needlestick Injury from Pustule". Emerging Infectious Diseases. 28 (12): 2516–2519. doi:10.3201/eid2812.221374. PMC 9707600. PMID 36252152. S2CID 252969061.
- ^ McFarland SE, Marcus U, Hemmers L, Miura F, Iñigo Martínez J, Martínez FM, et al. (July 2023). "Estimated incubation period distributions of mpox using cases from two international European festivals and outbreaks in a club in Berlin, May to June 2022". Euro Surveillance. 28 (27). doi:10.2807/1560-7917.ES.2023.28.27.2200806. PMC 10370040. PMID 37410383.
- ^ Prasad S, Galvan Casas C, Strahan AG, Fuller LC, Peebles K, Carugno A, et al. (March 2023). "A dermatologic assessment of 101 mpox (monkeypox) cases from 13 countries during the 2022 outbreak: Skin lesion morphology, clinical course, and scarring". Journal of the American Academy of Dermatology. 88 (5): 1066–1073. doi:10.1016/j.jaad.2022.12.035. ISSN 0190-9622. PMC 9833815. PMID 36641010.
- ^ Petersen BW, Damon IK (2020). "348. Smallpox, monkeypox and other poxvirus infections". In Goldman L, Schafer AI (eds.). Goldman-Cecil Medicine. Vol. 2 (26th ed.). Philadelphia: Elsevier. pp. 2180–2183. ISBN 978-0-323-53266-2. Archived from the original on 19 January 2023. Retrieved 28 May 2022.
- ^ a b c Vogel L (August 2022). "Making sense of monkeypox death rates". CMAJ. 194 (31): E1097. doi:10.1503/cmaj.1096012. PMC 9377567. PMID 35970550.
- ^ Gessain A, Nakoune E, Yazdanpanah Y (November 2022). "Monkeypox". The New England Journal of Medicine. 387 (19): 1783–1793. doi:10.1056/NEJMra2208860. PMID 36286263.
- ^ "Mpox (monkeypox) – Prognosis". BMJ Best Practice. Archived from the original on 31 May 2023. Retrieved 31 May 2023.
- ^ a b McQuiston JH, Luce R, Kazadi DM, Bwangandu CN, Mbala-Kingebeni P, Anderson M, et al. (May 2024). "U.S. Preparedness and Response to Increasing Clade I Mpox Cases in the Democratic Republic of the Congo – United States, 2024" (PDF). MMWR. Morbidity and Mortality Weekly Report. 73 (19): 435–440. doi:10.15585/mmwr.mm7319a3. PMC 11115432. PMID 38753567.
- ^ Dumonteil E, Herrera C, Sabino-Santos G (February 2023). "Monkeypox Virus Evolution before 2022 Outbreak". Emerging Infectious Diseases. 29 (2): 451–453. doi:10.3201/eid2902.220962. PMC 9881786. PMID 36692511.
- ^ a b "Mpox in Animals". U.S. Centers for Disease Control and Prevention (CDC). 4 January 2023. Archived from the original on 15 August 2024. Retrieved 25 May 2023.
- ^ Nash SL, Palmer SB, Wingfield WE (2009). "1.11. Zoonoses and zoonotic diseases". In Wingfield WE, Palmer SB (eds.). Veterinary Disaster Response. Iowa: John Wiley & Sons. pp. 167–168. ISBN 978-0-8138-1014-0. Archived from the original on 15 August 2024. Retrieved 1 June 2022.
- ^ "Examining Animals With Suspected Monkeypox". U.S. Centers for Disease Control and Prevention (CDC). 19 November 2019. Archived from the original on 19 May 2022. Retrieved 24 May 2022.
- ^ Seang S, Burrel S, Todesco E, Leducq V, Monsel G, Le Pluart D, et al. (August 2022). "Evidence of human-to-dog transmission of monkeypox virus". Lancet. 400 (10353): 658–659. doi:10.1016/S0140-6736(22)01487-8. PMC 9536767. PMID 35963267.
- ^ "New mpox clade 1 lineage identified in DR Congo outbreak". Center for Infectious Disease Research and Policy (CIDRAP). 17 April 2024. Retrieved 21 August 2024.
- ^ a b Moore MJ, Rathish B, Zahra F (30 November 2022), Mpox (Monkeypox), StatPearls Publishing, PMID 34662033, archived from the original on 16 March 2023, retrieved 26 May 2023
- ^ a b "Mpox – How It Spreads". U.S. Centers for Disease Control and Prevention (CDC). 2 February 2023. Archived from the original on 21 May 2023. Retrieved 23 May 2023.
- ^ "Mpox Q&A". World Health Organization (WHO). 17 August 2024. Retrieved 8 September 2024.
- ^ "WHO approves first mpox test for faster diagnoses". Al Jazeera. Retrieved 4 October 2024.
- ^ "Alinity m Monkeypox Assay". Abbott Laboratories. Retrieved 4 October 2024.
- ^ Kantele A, Chickering K, Vapalahti O, Rimoin AW (August 2016). "Emerging diseases-the monkeypox epidemic in the Democratic Republic of the Congo". Clinical Microbiology and Infection. 22 (8): 658–659. doi:10.1016/j.cmi.2016.07.004. PMC 9533887. PMID 27404372.
- ^ Rigby J (14 August 2024). "Mpox vaccines likely months away even as WHO, Africa CDC discuss emergency". Reuters.
- ^ Cornall J (25 July 2022). "Bavarian Nordic gets European monkeypox approval for smallpox vaccine". Labiotech UG. Retrieved 15 August 2024.
- ^ "Mpox – Prevention". British Medical Journal. Retrieved 15 August 2024.
- ^ "The Vector center will soon commence the production of the smallpox vaccine". GxP News. 26 September 2023. Retrieved 15 August 2024.
- ^ "FDA Roundup: August 30, 2024". U.S. Food and Drug Administration (FDA) (Press release). 30 August 2024. Retrieved 1 September 2024.
- ^ "Emergent BioSolutions' ACAM2000, (Smallpox and Mpox (Vaccinia) Vaccine, Live) Receives U.S. FDA Approval for Mpox Indication; Public Health Mpox Outbreak Continues Across Africa & Other Regions" (Press release). Emergent Biosolutions. 29 August 2024. Retrieved 1 September 2024 – via GlobeNewswire.
- ^ "Interim Clinical Considerations for Use of Jynneos Vaccine for Mpox Prevention in the United States". U.S. Centers for Disease Control and Prevention (CDC). 22 April 2024. Retrieved 15 August 2024.
- ^ "Jynneos Vaccine Effectiveness". U.S. Centers for Disease Control and Prevention (CDC). 19 May 2023. Archived from the original on 24 May 2023. Retrieved 24 May 2023.
- ^ "Considerations on posology for the use of the vaccine Jynneos/ Imvanex (MVA-BN) against monkeypox" (PDF). European Medicines Agency (EMA). 19 August 2022. Archived (PDF) from the original on 28 May 2023. Retrieved 28 May 2023.
- ^ "Protecting you from mpox (monkeypox): information on the smallpox vaccination". GOV.UK. Archived from the original on 28 May 2023. Retrieved 28 May 2023.
- ^ "Infection Prevention and Control of Mpox in Healthcare Settings". U.S. Centers for Disease Control and Prevention (CDC). 31 October 2022. Archived from the original on 18 May 2022. Retrieved 21 May 2022.
- ^ "Multi-country monkeypox outbreak in non-endemic countries: Update". World Health Organization (WHO). Archived from the original on 30 May 2022. Retrieved 28 May 2023.
- ^ "CDC's Mpox Toolkit for Event Organizers". U.S. Centers for Disease Control and Prevention (CDC). 23 May 2023. Archived from the original on 28 May 2023. Retrieved 28 May 2023.
- ^ "Monkeypox – Campaign details". Department of Health and Social Care – Campaign Resource Centre. Archived from the original on 28 May 2023. Retrieved 28 May 2023.
- ^ "Mpox (Monkeypox) awareness campaign: Communications toolkit for stakeholders". Western Australia Department of Health. 10 June 2022. Archived from the original on 28 May 2023. Retrieved 28 May 2023.
- ^ "Tecovirimat SIGA". European Medicines Agency (EMA). 28 January 2022. Archived from the original on 16 May 2022. Retrieved 19 May 2022.
- ^ a b Fox T, Gould S, Princy N, Rowland T, Lutje V, Kuehn R, et al. (Cochrane Infectious Diseases Group) (March 2023). "Therapeutics for treating mpox in humans". The Cochrane Database of Systematic Reviews. 2023 (3): CD015769. doi:10.1002/14651858.CD015769. PMC 10012405. PMID 36916727.
- ^ a b c "Mpox (monkeypox) – Treatment algorithm". BMJ Best Practice. Archived from the original on 4 December 2022. Retrieved 14 March 2023.
- ^ "Factsheet for health professionals on mpox (monkeypox)". European Centre for Disease Prevention and Control. 25 October 2022. Archived from the original on 20 June 2022. Retrieved 29 May 2023.
- ^ "The antiviral tecovirimat is safe but did not improve clade I mpox resolution in Democratic Republic of the Congo". National Institutes of Health (NIH). 14 August 2024. Retrieved 16 August 2024.
- ^ Mast J (15 August 2024). "Antiviral used for mpox no better than placebo, NIH says". STAT. Retrieved 16 August 2024.
- ^ Priyan V (16 August 2024). "NIAID reports preliminary data from trial of SIGA's Mpox treatment". Clinical Trials Arena. Retrieved 16 August 2024.
- ^ "Siga's mpox drug did not improve lesion resolution or pain, NIH study finds". Reuters. 10 December 2024.
- ^ "NIH Study Finds Tecovirimat Safe, But Ineffective for Treating Mpox". ContagionLive. 11 December 2024. Retrieved 15 December 2024.
- ^ "NIH Study Finds Tecovirimat Was Safe but Did Not Improve Mpox Resolution or Pain". National Institutes of Health (NIH). 10 December 2024. Retrieved 15 December 2024.
- ^ "WHO invites makers of mpox tests for emergency review in push for rapid access". Reuters. 29 August 2024.
- ^ "WHO urges rapid access to mpox diagnostic tests, invites manufacturers to emergency review". World Health Organization (WHO). Retrieved 31 August 2024.
- ^ "Mpox global strategic preparedness and response plan". World Health Organization (WHO). Retrieved 31 August 2024.
- ^ Parker S, Buller RM (February 2013). "A review of experimental and natural infections of animals with Orthopoxvirus monkeypox between 1958 and 2012". Future Virology. 8 (2): 129–157. doi:10.2217/fvl.12.130. PMC 3635111. PMID 23626656.
- ^ Cho CT, Wenner HA (March 1973). "Monkeypox virus". Bacteriological Reviews. 37 (1): 1–18. doi:10.1128/br.37.1.1-18.1973. PMC 413801. PMID 4349404.
- ^ Meyer H, Perrichot M, Stemmler M, Emmerich P, Schmitz H, Varaine F, et al. (August 2002). "Outbreaks of disease suspected of being due to human Orthopoxvirus monkeypox infection in the Democratic Republic of Congo in 2001". Journal of Clinical Microbiology. 40 (8): 2919–2921. doi:10.1128/JCM.40.8.2919-2921.2002. PMC 120683. PMID 12149352.
- ^ Falendysz EA, Lopera JG, Lorenzsonn F, Salzer JS, Hutson CL, Doty J, et al. (30 October 2015). "Further Assessment of Monkeypox Virus Infection in Gambian Pouched Rats (Cricetomys gambianus) Using In Vivo Bioluminescent Imaging". PLOS Neglected Tropical Diseases. 9 (10): e0004130. doi:10.1371/journal.pntd.0004130. PMC 4627722. PMID 26517839.
- ^ Sklenovská N, Van Ranst M (September 2018). "Emergence of Monkeypox as the Most Important Orthopoxvirus Infection in Humans". Frontiers in Public Health. 6: 241. doi:10.3389/fpubh.2018.00241. PMC 6131633. PMID 30234087.
- ^ James WD, Elston D, Treat JR, Rosenbach MA, Neuhaus I (2020). "19. Viral diseases". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. p. 389. ISBN 978-0-323-54753-6. Archived from the original on 19 January 2023. Retrieved 9 June 2022.
- ^ Johnson PL, Bergstrom CT, Regoes RR, Longini IM, Halloran ME, Antia R (October 2022). "Evolutionary consequences of delaying intervention for monkeypox". Lancet. 400 (10359): 1191–1193. doi:10.1016/S0140-6736(22)01789-5. PMC 9534010. PMID 36152668.
- ^ "Monkeypox cases waning, but global threat remains". Gavi, the Vaccine Alliance. Archived from the original on 1 June 2023. Retrieved 1 June 2023.
- ^ Adetifa I, Muyembe JJ, Bausch DG, Heymann DL (May 2023). "Mpox neglect and the smallpox niche: a problem for Africa, a problem for the world". Lancet. 401 (10390): 1822–1824. doi:10.1016/S0140-6736(23)00588-3. PMC 10154003. PMID 37146622. S2CID 258441920.
- ^ "Mpox (monkeypox) and animals". Public Health Agency of Canada. 30 December 2022. Archived from the original on 1 June 2023. Retrieved 1 June 2023.
- ^ Mathieu E, Spooner F, Dattani S, Ritchie H, Roser M (24 May 2022). "Mpox (monkeypox)". Our World in Data. Archived from the original on 3 July 2022. Retrieved 5 October 2023.
- ^ "Mpox (monkeypox)- Democratic Republic of the Congo". World Health Organization (WHO). 23 November 2023. Archived from the original on 24 November 2023. Retrieved 25 November 2023.
- ^ Mallapaty S (2 August 2024). "The pathogens that could spark the next pandemic". Nature. 632 (8025): 488. Bibcode:2024Natur.632..488M. doi:10.1038/d41586-024-02513-3. PMID 39095457. Archived from the original on 2 August 2024. Retrieved 2 August 2024.
- ^ "Multi-country monkeypox outbreak in non-endemic countries". World Health Organization (WHO). Archived from the original on 22 May 2022. Retrieved 31 May 2023.
- ^ Besombes C, Mbrenga F, Schaeffer L, Malaka C, Gonofio E, Landier J, et al. (December 2022). "National Monkeypox Surveillance, Central African Republic, 2001–2021". Emerging Infectious Diseases. 28 (12): 2435–2445. doi:10.3201/eid2812.220897. PMC 9707566. PMID 36328951.
- ^ Kozlov M (February 2023). "WHO may soon end mpox emergency - but outbreaks rage in Africa". Nature. 614 (7949): 600–601. Bibcode:2023Natur.614..600K. doi:10.1038/d41586-023-00391-9. PMID 36765257. S2CID 256764657. Archived from the original on 16 May 2023. Retrieved 30 May 2023.
- ^ "In Central Africa, a deadly monkeypox variant is surging". National Geographic. 20 October 2022. Archived from the original on 30 May 2023. Retrieved 30 May 2023.
- ^ Nakoune E, Lampaert E, Ndjapou SG, Janssens C, Zuniga I, Van Herp M, et al. (2017). "A Nosocomial Outbreak of Human Monkeypox in the Central African Republic". Open Forum Infectious Diseases. 4 (4): ofx168. doi:10.1093/ofid/ofx168. PMC 5920348. PMID 29732376.
- ^ "Monkeypox - Democratic Republic of the Congo October 2020". World Health Organization (WHO). Archived from the original on 5 June 2022. Retrieved 20 March 2024.
- ^ a b "Joint ECDC-WHO Regional Office for Europe Monkeypox Surveillance Bulletin: 15 August 2024". World Health Organization (WHO). Retrieved 24 August 2024.
- ^ a b Cohen J (3 August 2024). "Deadlier strain of mpox spreads to multiple African countries". Science. Archived from the original on 15 August 2024. Retrieved 5 August 2024.
- ^ Anderson MG, Frenkel LD, Homann S, Guffey J (December 2003). "A case of severe monkeypox virus disease in an American child: emerging infections and changing professional values". The Pediatric Infectious Disease Journal. 22 (12): 1093–1096. doi:10.1097/01.inf.0000101821.61387.a5. PMID 14688573.
- ^ Bartlett J. "Medscape Monkeypox Review". Medscape. Archived from the original on 2 December 2012. Retrieved 22 March 2013.
- ^ "Monkeypox in the United States". U.S. Centers for Disease Control and Prevention (CDC). 19 November 2021. Archived from the original on 27 April 2022. Retrieved 27 April 2022.
- ^ Centers for Disease Control and Prevention (CDC) (July 2003). "Update: multistate outbreak of monkeypox—Illinois, Indiana, Kansas, Missouri, Ohio, and Wisconsin, 2003" (PDF). MMWR. Morbidity and Mortality Weekly Report. 52 (27): 642–646. PMID 12855947. Archived (PDF) from the original on 8 December 2022. Retrieved 4 December 2022.
- ^ "A Case of Monkeypox in a Returned Traveler". ProQuest. Archived from the original on 31 May 2022. Retrieved 23 May 2022.
- ^ Apoorva Mandavilli (17 November 2024). "First U.S. Case of Severe Form of Mpox Reported in California". nytimes.com. Retrieved 17 November 2024.
- ^ "Mpox in the United States and Around the World: Current Situation". U.S. Centers for Disease Control and Prevention (CDC). 26 September 2024. Retrieved 20 October 2024.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "U.S. Case Trends". U.S. Centers for Disease Control and Prevention (CDC). 15 October 2024. Retrieved 20 October 2024.
- ^ a b Dafallah MA (June 2023). "The current status of monkeypox in Sudan". Annals of Medicine & Surgery. 85 (6): 3202–3203. doi:10.1097/MS9.0000000000000284. PMC 10289688. PMID 37363511.
- ^ Yinka-Ogunleye A, Aruna O, Dalhat M, Ogoina D, McCollum A, Disu Y, et al. (August 2019). "Outbreak of human monkeypox in Nigeria in 2017–18: a clinical and epidemiological report". The Lancet. Infectious Diseases. 19 (8): 872–879. doi:10.1016/S1473-3099(19)30294-4. PMC 9628943. PMID 31285143. S2CID 195842553.
- ^ Ileyemi M (10 May 2022). "Monkeypox: Nigeria records 558 cases, eight deaths in five years". Premium Times. Archived from the original on 10 May 2022. Retrieved 25 May 2022.
- ^ "First ever case of monkeypox recorded in the UK". The Guardian. 8 September 2018. Archived from the original on 8 September 2018. Retrieved 8 September 2018.
- ^ Damien G (26 September 2018). "Medic becomes third person infected with monkeypox in England". The Guardian. Archived from the original on 26 September 2018. Retrieved 26 September 2018.
- ^ "Monkeypox case confirmed in England". Public Health England. 4 December 2019. Archived from the original on 12 December 2019. Retrieved 12 December 2019.
- ^ Hobson G, Adamson J, Adler H, Firth R, Gould S, Houlihan C, et al. (August 2021). "Family cluster of three cases of monkeypox imported from Nigeria to the United Kingdom, May 2021". Euro Surveillance. 26 (32). doi:10.2807/1560-7917.ES.2021.26.32.2100745. PMC 8365177. PMID 34387184.
- ^ "News Scan for May 09, 2019". Center for Infectious Disease Research and Policy (CIDRAP). 9 May 2019. Archived from the original on 10 May 2019. Retrieved 10 May 2019.
- ^ "Monkeypox – Singapore". World Health Organization (WHO). 16 May 2019. Archived from the original on 1 July 2019. Retrieved 17 May 2019.
- ^ "Multi-country monkeypox outbreak in non-endemic countries". World Health Organization (WHO). 21 May 2022. Archived from the original on 22 May 2022. Retrieved 25 May 2022.
- ^ "Monkeypox cases confirmed in England – latest updates". GOV.UK. 6 September 2022. Archived from the original on 16 May 2022. Retrieved 25 September 2022.
- ^ "Monkeypox – United Kingdom of Great Britain and Northern Ireland". World Health Organization (WHO). 16 May 2022. Archived from the original on 17 May 2022. Retrieved 17 May 2022.
- ^ "Viruela del mono: confirmaron el primer caso del virus en el país" (in Spanish). 26 May 2022. Archived from the original on 24 June 2022. Retrieved 26 May 2022.
- ^ "UAE reports first case of monkeypox in the country". Al Arabiya. 24 May 2022. Archived from the original on 24 May 2022. Retrieved 24 May 2022.
- ^ Efrati I. "Israel Confirms First Case of Monkeypox Virus". Haaretz. Archived from the original on 20 May 2022. Retrieved 21 May 2022.
- ^ "Monkeypox confirmed in Melbourne and Sydney". Australian Broadcasting Corporation. 20 May 2022. Archived from the original on 20 May 2022. Retrieved 20 May 2022.
- ^ "Morocco Reports First Monkeypox Case". Morocco World News. Archived from the original on 21 June 2022. Retrieved 2 June 2022.
- ^ Christian Y (8 June 2022). "5 cases of monkeypox confirmed in Ghana". MyJoyOnline.com. Archived from the original on 21 June 2022. Retrieved 8 June 2022.
- ^ [114][115][116][117][118][119]
- ^ Kimball S (11 May 2023). "WHO says mpox outbreak, the largest in history, no longer global health emergency". CNBC. Archived from the original on 11 May 2023. Retrieved 11 May 2023.
- ^ a b c Van Beusekom M (16 March 2024). "More than 600 dead in spreading DR Congo mpox outbreak as Republic of Congo reports its first cases". Center for Infectious Disease Research and Policy (CIDRAP). Archived from the original on 19 March 2024. Retrieved 19 March 2024.
- ^ Stawiska Z (13 March 2024). "Deadly Mpox Transmission in DR Congo Happening Under Radar; Most Victims are Children". Health Policy Watch. Archived from the original on 15 August 2024. Retrieved 6 August 2024.
- ^ Mandavilli A (14 August 2024). "W.H.O. Declares Global Emergency over New Mpox Outbreak". The New York Times. Archived from the original on 14 August 2024. Retrieved 14 August 2024.
- ^ "Sweden confirms first case of mpox strain outside Africa". Al Jazeera. 15 August 2024. Retrieved 16 August 2024.
- ^ "Pakistan registers 1st case of mpox". DW. 16 August 2024. Retrieved 7 September 2024.
External links
[edit]- Mpox US Centers for Disease Control and Prevention (CDC)
- Monkeypox Fact Sheet World Health Organization (WHO)
- "Could Monkeypox Take Over Where Smallpox Left Off?". Scientific American, 4 March 2013.
- MonkeypoxTracker – Monkeypox statistics visualization site
- PoxApp – the mpox app – Assesses skin lesions and symptoms with artificial intelligence developed by Stanford University
 KSF
KSF