Hereditary Breast And Ovarian Cancer Syndrome
 From Mdwiki
From Mdwiki | Hereditary breast and ovarian cancer syndrome | |
|---|---|
| Other names: HBOC | |
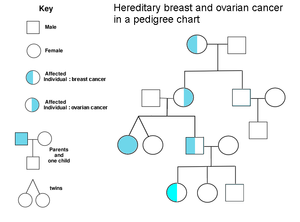 | |
| Ovarian and breast cancer patients in a pedigree chart of a family | |
| Specialty | Oncology[1] |
| Causes | Mostly mutations of the BRCA1 and BRCA2 genes[2] |
Hereditary breast and ovarian cancer syndrome (HBOC) is an inherited condition that increases the chance of developing breast cancer, ovarian cancer and additional cancers such as of the fallopian tube, peritoneum, prostate, pancreas and endometrium, among others.[1]
It is most often caused by passing down in a family of mutations of the BRCA1 and BRCA2 genes, and to much lesser extent, other gene mutations.[2] The BRCA mutation is more likely if there is a personal or family history of breast cancer diagnosed at age 45 years or younger in females, age 46-to-50 years with one or more immediate relative with breast cancer, breast cancer in males, triple negative breast cancer at age 60 or younger in females, cancer in both breasts, a known BRCA mutation in the family.[2] Other risk factors include ovarian, fallopian tube, or primary peritoneal cancer, high grade prostate cancer, Eastern European Jewish ancestry, and having several family members with breast, ovarian, pancreatic, or prostate cancer.[2]
Screening family members of people diagnosed with breast, ovarian, tubal, or peritoneal cancer is recommended in the US.[2]
In 1971, David E. Anderson described the autosomal dominant inheritance of a predisposition to both breast and ovarian cancers.[3] The collective term 'hereditary breast and ovarian cancer syndrome' was coined in 1994 by Henry Lynch.[3]
Causes[edit | edit source]
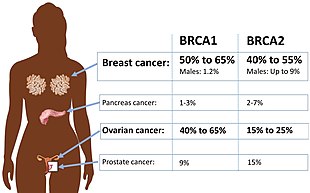
A number of genes are associated with HBOC.[5] The most common of the known causes of HBOC are:
- BRCA mutations:[5] Harmful mutations in the BRCA1 and BRCA2 genes can produce very high rates of breast and ovarian cancer, as well as increased rates of other cancers. Mutations in BRCA1 are associated with a 39-46% risk of ovarian cancer and mutations in BRCA2 are associated with a 10-27% risk of ovarian cancer.[6]
Other identified genes include:
- MLH1, MSH2, MSH6, PMS2: mutations in genes that lead to Lynch Syndrome put individuals at risk for ovarian cancer.[7]
- TP53: Mutations cause Li-Fraumeni syndrome. It produces particularly high rates of breast cancer among younger women with mutated genes, and despite being rare, 4% of women with breast cancer under age 30 have a mutation in this gene.[5]
- PTEN: Mutations cause Cowden syndrome, which produces hamartomas (benign polyps) in the colon, skin growths, and other clinical signs, as well as an increased risk for many cancers.[5]
- CDH1: Mutations are associated with lobular breast cancer and gastric cancer.[5]
- STK11: Mutations produce Peutz–Jeghers syndrome. It is extremely rare, and creates a predisposition to breast cancer, intestinal cancer, and pancreatic cancer.[5]
- CHEK2: Approximately one out of 40 northern Europeans have a mutation in this gene, making it a common mutation. It is also one of the most frequently mutated genes after BRCA among Hispanics in the United States.[8] Considered a moderate-risk mutation, it may double or triple the carrier's lifetime risk of breast cancer, and also increase the risk of colon cancer and prostate cancer.[5]
- ATM: Mutations cause ataxia telangectasia; female carriers have approximately double the normal risk of developing breast cancer.[5]
- PALB2: Studies vary in their estimate of the risk from mutations in this gene and the frequency of mutations in this gene may be different among different populations.[8] It may be moderate risk, or as high as BRCA2.[5]
Approximately 45% of HBOC cases involve unidentified genes, or multiple genes.[5]
It accounts for 90% of the hereditary cancers.[9] The hereditary factors may be proven or suspected to cause the pattern of breast and ovarian cancer occurrences in the family.[10] The name HBOC may be misleading because it implies that this genetic susceptibility to cancer is mainly in women. In reality, both sexes have the same rates of gene mutations and HBOC can predispose to other cancers including prostate cancer and pancreatic cancer.[11]
Prevention[edit | edit source]
People with BRCA1 and BRCA2 mutations are recommended to have a transvaginal ultrasound 1-2 times per year. Screening with CA-125 is also recommended. Prophylactic salpingo-oophorectomy (removal of the ovaries and Fallopian tubes to prevent cancer) is recommended at age 35-40 for people with BRCA1 mutations and at age 40-45 for people with BRCA2 mutations.[6]
History[edit | edit source]
Paul Broca first described a high prevalence of breast cancer in a family in 1866.[3] In 1971, David E. Anderson described the autosomal dominant inheritance of a predisposition to both breast and ovarian cancers.[3] The collective term 'hereditary breast and ovarian cancer syndrome' was coined in 1994 by Henry Lynch.[3]
References[edit | edit source]
- ↑ 1.0 1.1 WHO Classification of Tumours Editorial Board, ed. (2020). "16. Genetic tumour syndromes of the female genital tract: BRCA1/2-associated hereditary breast and ovarian cancer syndrome". Female genital tumours: WHO Classification of Tumours. Vol. 4 (5th ed.). Lyon (France): International Agency for Research on Cancer. pp. 544–545. ISBN 978-92-832-4504-9. Archived from the original on 2022-06-17. Retrieved 2022-06-24.
- ↑ 2.0 2.1 2.2 2.3 2.4 "Hereditary Breast and Ovarian Cancer Syndrome: A Guide for Patients and Their Families | CDC". www.cdc.gov. 11 January 2016. Archived from the original on 9 July 2022. Retrieved 25 June 2022.
- ↑ 3.0 3.1 3.2 3.3 3.4 Yoshida, Reiko (2021). "1. History, advancements, and future strategies". In Nakamura, Seigo; Aoki, Daisuke; Miki, Yoshio (eds.). Hereditary Breast and Ovarian Cancer: Molecular Mechanism and Clinical Practice. Springer. ISBN 978-981-16-4521-1. Archived from the original on 2022-07-09. Retrieved 2022-07-09.
- ↑ Petrucelli N, Daly MB, Pal T (December 2016) [September 1998]. "BRCA1- and BRCA2-Associated Hereditary Breast and Ovarian Cancer". In Adam MP, Ardinger HH, Pagon RA, Wallace SE, Bean LJ, Mirzaa G, Amemiya A (eds.). GeneReviews. University of Washington, Seattle. PMID 20301425. Archived from the original on 2020-05-28. Retrieved 2021-12-26.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 5.9 Morris, Joi L.; Gordon, Ora K. (Ora Karp) (2010). Positive results : making the best decisions when you're at high risk for breast or ovarian cance. Amherst, N.Y.: Prometheus Books. pp. 337–340. ISBN 978-1-59102-776-8.
- ↑ 6.0 6.1 Ring, Kari L.; Garcia, Christine; Thomas, Martha H.; Modesitt, Susan C. (November 2017). "Current and future role of genetic screening in gynecologic malignancies". American Journal of Obstetrics and Gynecology. 217 (5): 512–521. doi:10.1016/j.ajog.2017.04.011. ISSN 1097-6868. PMID 28411145. S2CID 29024566.
- ↑ Woolderink, J. M.; De Bock, G. H.; de Hullu, J. A.; Hollema, H.; Zweemer, R. P.; Slangen, B. F. M.; Gaarenstroom, K. N.; van Beurden, M.; van Doorn, H. C. (August 2018). "Characteristics of Lynch syndrome associated ovarian cancer". Gynecologic Oncology. 150 (2): 324–330. doi:10.1016/j.ygyno.2018.03.060. hdl:1887/96199. ISSN 1095-6859. PMID 29880284. S2CID 46967266.
- ↑ 8.0 8.1 Weitzel, Jeffrey N.; Neuhausen, Susan L.; Adamson, Aaron; Tao, Shu; Ricker, Charité; Maoz, Asaf; Rosenblatt, Margalit; Nehoray, Bita; Sand, Sharon (2019-06-17). "Pathogenic and likely pathogenic variants in PALB2, CHEK2, and other known breast cancer susceptibility genes among 1054 BRCA-negative Hispanics with breast cancer". Cancer. 125 (16): 2829–2836. doi:10.1002/cncr.32083. ISSN 1097-0142. PMC 7376605. PMID 31206626.
- ↑ Bickerstaff, Helen (2017). Gynaecology by Ten Teachers. United Kingdom: CRC Press. p. 330. ISBN 978-1-4987-4428-7.
- ↑ "Hereditary Breast Ovarian Cancer Syndrome (BRCA1 / BRCA2)". Stanford University. Archived from the original on 2009-11-15. Retrieved 2008-09-02.
- ↑ Pritchard, Colin C. (July 2019). "New name for breast-cancer syndrome could help to save lives". Nature. 571 (7763): 27–29. Bibcode:2019Natur.571...27P. doi:10.1038/d41586-019-02015-7. PMID 31270479.
External links[edit | edit source]
| Classification | |
|---|---|
| External resources |
Categories: [Ovarian cancer] [Breast cancer] [Hereditary cancers] [Rare cancers] [Syndromes affecting the breast] [Syndromes in females]
↧ Download as ZWI file | Last modified: 04/10/2024 13:47:38 | 3 views
☰ Source: https://mdwiki.org/wiki/Hereditary_breast_and_ovarian_cancer_syndrome | License: CC BY-SA 3.0
 KSF
KSF